Re-sensitizing Drug-resistant Human Tumor Cells
Understanding how cancer cells avoid death despite their DNA being damaged will create new strategies to enhance cancer cell killing through chemotherapy treatment. Even though the most widely used drugs are DNA-damaging agents (DDAs), their therapeutic success has been often halted by drug resistance. Addressing the challenges of drug resistance is crucial in the field of clinical cancer treatments.
Watch the short video below to learn more about drug-resistant cancer:
Now, a recent study published in the Nature Structural and Molecular Biology discusses a new way of re-sensitizing drug-resistant human tumor cells to the potency of DDAs and paving the way to new strategies to overcome chemotherapeutic drug resistance.
The researchers found that protein, called Schlafen 11, inhibits the production of two other proteins ATM and ATR that are found in tumor cells. "We found that if you expose cells that have Schlafen 11 to DNA damaging agents, the Schlafen 11 protein gets activated and suppresses the synthesis of ATM and ATR -- that's essentially what kills the tumor cells," explains Professor Michael David, a professor in the Biological Sciences Section of Molecular Biology and UC San Diego Moores Cancer Center. "In cells that do not express Schlafen 11, you do not get this downregulation of ATM/ATR and that essentially allows the tumor cells to survive."

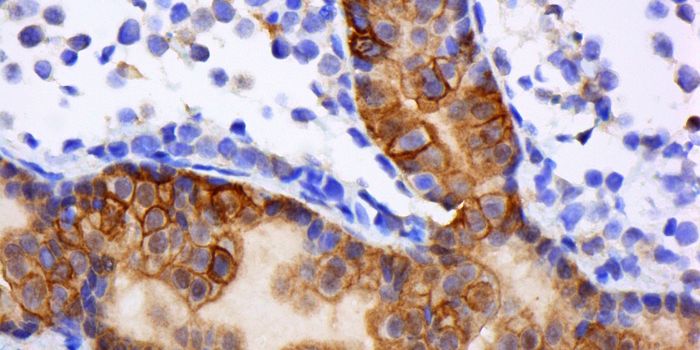
Image: “Pancreatic cancer cells deficient in the expression of the human gene known as Schlafen 11 and resistant to chemotherapy (left panels) were re-sensitized to chemotherapeutic treatment (middle and right panels) by inhibiting the expression of the transfer RNA known as tRNA-Leu-TAA through specially designed antisense oligonucleotides.”- ScienceDaily
Digging deeper into the mechanism of Schlafen 11 works on a molecular level, the researchers discovered that most of the genes involved in DNA damage repair pathways will display a similar skewing of their transfer RNA seen in HIV, specifically towards tRNA-Leu-TAA—prompting a new tecnhique to re-sensitize Schlafen 11-deficient tumor cells to drugs via the targeting of tRNA-Leu-TAA.
Such intervention may influence the entire DNA damage repair pathway -- including ATM and ATR – to not just inhibit the function of one specific component at a time. "These results suggest two ways to enhance the killing of cancer cells by DNA-damaging drugs by adding 1) ATR inhibitors or 2) tRNA inhibitors," said study coauthor Jean Wang, professor emeritus in UC San Diego's School of Medicine. "The paper is also of significance to the basic research on DNA damage response because it shows for the first time that regulation of tRNAs determines when a damaged cell will survive or die."
Despite being relevant to DNA damage and cancer, the research holds applications in immunology and virology, particularly in HIV treatments, because of the fundamental mechanisms behind Schlafen 11.
Source: Nature Structural & Molecular Biology, Science Daily
-
APR 30, 2024Immuno-Oncology Virtual Event Series 2024
-
MAY 07, 20243rd International Biosecurity Virtual Symposium
-
JUN 06, 2024The Future of Scientific Conferencing
- See More