Waging a War on Antibiotic Resistant Bacteria
In a world where we are constantly exposed to microbes and bacteria in our daily environment, infections are all but rare. Some infections are hardly noticeable and the body can handle the clearing of the culprit easily, but other infections can cause serious harm and even result in death if not able to be treated. Luckily, modern day medicine has been developed to address a wide variety of infections originating from a multitude of sources; however, multi-drug resistant organisms have emerged causing a substantial crisis in public health globally. These organisms which may have been initially responsive to treatment modalities have evolved and become resistant to the same treatment they once responded to. Today, it is more common than ever before for people to go to the doctor for nearly any ailment, which has led to antibiotics being prescribed constantly. This abundant use of antibiotics has resulted in selective pressure of highly resistant strains which are able to persist and continue to infect humans and animals. According to the Center for Disease Control and Prevention based out of Atlanta, Georgia, there are two million infections and 23,000 deaths from infections annually in the United States alone. This is clearly a problem, and is particularly true in hospital settings where patients who may have immune-compromised situations in the first place are exposed to other potentially-infected patients, bacteria, and microbes. Once infected, patients are typically given broad-spectrum antibiotics while clinicians attempt to isolate and identify the source of infection and testing to determine what antibiotics the infection will respond to is conducted. This process is time consuming, taking days while the infection continues to progress hourly. Furthermore, development of new antibiotics to combat the newly resistant strains of bacteria typically takes a decade or better.
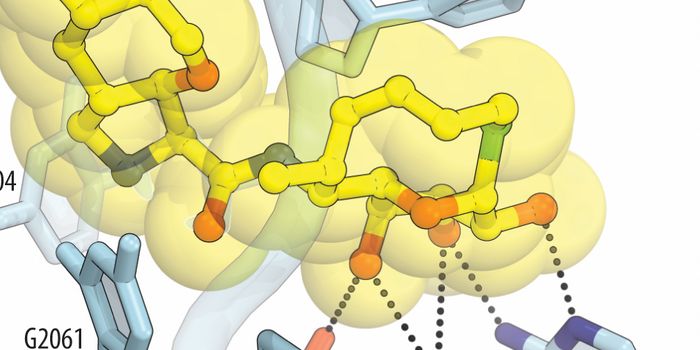
Scientists at the National Institutes of Health’s National Center for Advancing Translational Sciences and Clinical Center and National Institute for Allergy and Infectious Diseases have come together to develop a new approach to combat resistant bacteria. They have developed a novel high throughput screening platform to identify drugs and combinations of drugs that could be used to target multi-drug resistant microbes in a more rapid and robust manner than previously available. This platform involves the screening of thousands of known, already approved drugs which could be repurposed for combating infections is found to be effective. This repurposing allows for the drugs identified as effective to be moved much more quickly into clinical use. A researcher from the National Center for Advancing Translational Sciences, Wei Zheng, PhD, and his colleagues from the collaborating institutions tested this platform by screening 4,000 already approved compounds and were able to identify 25 “hit” compounds which could abrogate the growth of two drug resistant strains of the bacteria Klebsiella pneumonia known to be fatal. Additionally, these researchers found that combinations of approved drugs also proved to be an effective strategy to combat antibiotic resistant bacteria. Dr. Zheng was quoted as saying “The results are very promising, and we think that the test can eventually help repurpose approved drugs and other compounds and find clinically relevant drug combinations that can be approved for use in different ways that we have never used before. We are hoping this approach will lead to approvable, effective ways to combat dangerous infections by drug resistant bacteria”. This screening represents a breakthrough in drug discovery for the antimicrobial world, and will hopefully contribute greatly to progress in the field.
Additional Resources: The Center for Disease Control, Wikipedia, Pixabay, Youtube
-
APR 30, 2024Immuno-Oncology Virtual Event Series 2024
-
MAY 07, 20243rd International Biosecurity Virtual Symposium
-
SEP 03, 2024Microbiology Week Virtual Event Series 2024
- See More