Antibodies are supposed to protect us from infection, right? Right, and this is true under most circumstances. Sometimes, however, antibodies can actually enhance infection through a process called antibody-dependent enhancement.
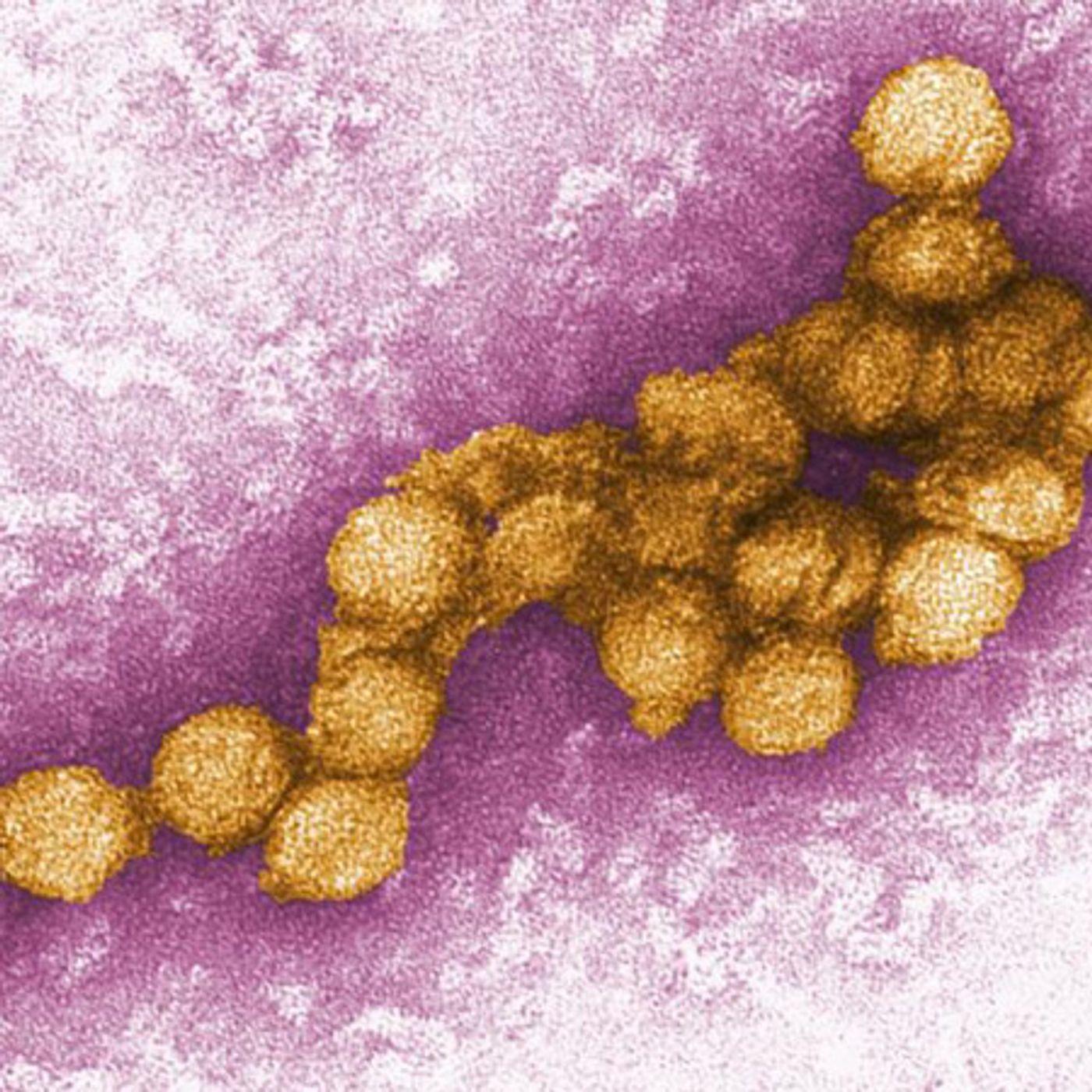
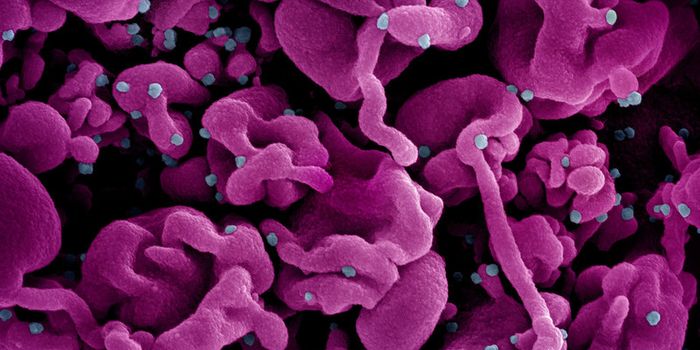
There are a handful of mechanisms by which antibodies can enhance infections by viruses and bacteria, but here I’ll focus mainly on Dengue virus. Dengue virus, a flavivirus that causes Dengue fever, is transmitted by mosquitoes.
Image: Centers for Disease Control
In many cases, antibody-dependent enhancement (ADE) occurs when sub-neutralizing concentrations of antibody attach to a virus. The Fc portion of these antibodies can then bind to the Fc receptors on immune cells, usually macrophages. This process allows the virus to enter the macrophage and establish a productive infection. Great for the virus, not great for the host.
With respect to Dengue virus, Dr. Scott Halstead first observed the effects of ADE in the 1960s. He realized that if a person was infected with Dengue a second time, that infection was much more serious than the first, causing Dengue hemorrhagic fever or Dengue shock syndrome.
This is when Halstead proposed the idea of "antibody-dependent enhancement of infection." After the initial infection, the body establishes a population of memory B cells that makes Dengue-specific antibodies. The problem is that there are four different strains of Dengue virus. If a person is later infected by a different strain, the antibodies made by the memory B cells will not effectively neutralize the virus, resulting in ADE. Unfortunately, ADE can also occur in children who received Dengue antibodies in utero.
Image: Shutterstock
ADE doesn’t just help viruses get into host cells, it also wreaks havoc on the body’s immune response. During the initial infection, the virus interacts with the dengue virus receptor on host cells, inducing pathogen recognition-receptor signaling. This signaling pathway induces the production of type I interferon, a proinflammatory and antiviral cytokine.
During the secondary infection, however, the virus-antibody complex signals the host cell to downregulate pathogen recognition-receptor signaling and produce IL-10. IL-10 induces SOCS signaling (suppressor of cytokine signalling), which dampens the immune response to the virus.
ADE doesn’t just occur with viral infections, there’s evidence that it occurs with bacteria too! Streptococcus pneumoniae causes pneumonia, and the body’s antibody response actually helps these bacteria attach to host cells. S. pneumoniae cells are covered by a capsule, and host IgA1 antibodies recognize and bind to capsular polysaccharides. When this happens, S. pneumoniae releases IgA1 protease, which cleaves the antibody into its Fab and Fc components. The positively charged Fab portion remains attached to the bacterium, disrupting the negatively charged capsule. This exposes ChoP (phosphorylcholine) on the surface of the bacterium. Finally, ChoP binds to its specific receptor on host cells, thereby enhancing infection.
Unfortunately, ADE and Dengue are making headlines because of their connection with Zika virus - there’s evidence that Dengue antibodies can enhance Zika virus infection. A study published earlier this year demonstrated that anti-flavivirus antibodies promote ADE of Zika virus infection in immunocompromised mice.
The researchers, from Washington University in St. Louis, injected the immunocompromised mice with plasma from people exposed to different flaviviruses (Dengue and West Nile). Only 21% of the mice that received plasma with Dengue antibodies survived for 1 week after being infected with Zika, but 93% of the control mice survived. The mice that received Dengue antibodies also experienced more serious symptoms with Zika infection, suggesting that ADE occurred.
With Dengue and Zika vaccines in the works, researchers must consider how ADE factors into the equation. It’s possible that a Dengue vaccine could make a Zika infection worse, or a Zika vaccine could make Dengue infection worse.
Sources: TRENDS in Immunology, Science, The Scientist, PLOS Blogs, The Lancet, Nature Education, Nature
-
MAY 07, 2024Is It Anti-RNP or Anti-Sm/RNP?
- See More
-
APR 30, 2024Immuno-Oncology Virtual Event Series 2024
-
MAY 07, 20243rd International Biosecurity Virtual Symposium
-
JUN 06, 2024The Future of Scientific Conferencing
- See More