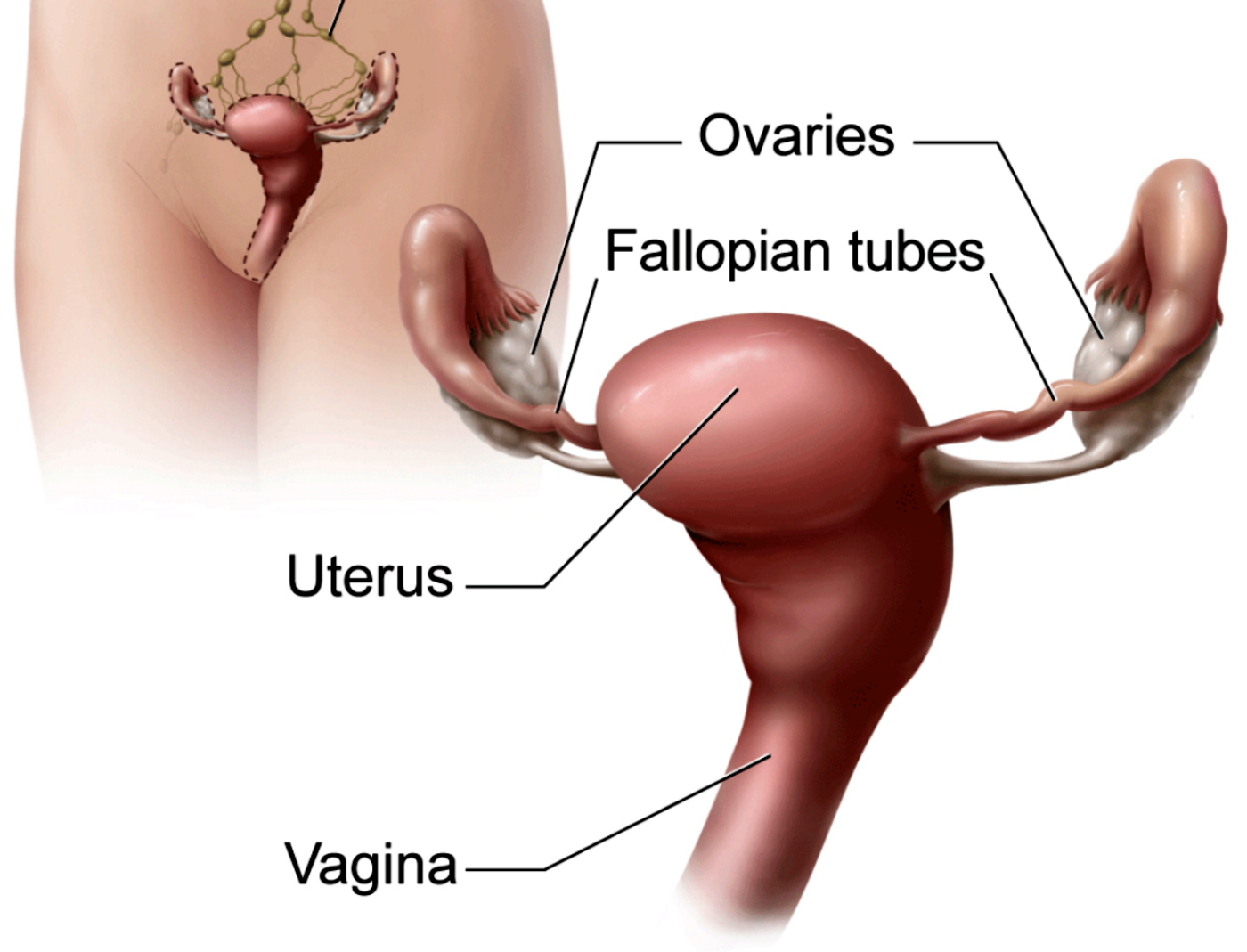
Uterine Cancer Rises, Especially Among Black Women
A recent study from the National Cancer Institute (NCI) found uterine cancer rates among all women rose about 1 percent per year between 2003 and 2015. It’s important to note that this is a hysterectomy-corrected finding, meaning that it took hysterectomy prevalence into account, because women with hysterectomies do not develop this disease. The authors also found that aggressive, nonendometrioid cancers are increasing for all women, and that significant racial disparities exist in uterine cancer rates. Black women are experiencing documented increases in uterine cancer above other groups of women, as well as lower rates of survival.
Rising Uterine Cancer Rates
Relying on population data from NCI’s Surveillance, Epidemiology and End Results (SEER) database, the researchers found uterine cancer rates rose between 2000 and 2015 and, overall, it increased more rapidly among women who were not white. The study also looked at data on endometrioid and nonendometrioid subtypes of uterine cancer. Nonendometrioid cancers are rarer and generally have lower survival rates.
Incidence rates of endometrioid cancers were stable in white women and increased in women of other groups. But rates of the less common, aggressive, nonendometrioid subtypes have been increasing “dramatically” in all groups and especially among black women, who experienced a rate of 25.9 per 100,000 women. The rate for white women was 11.4 per 100,000; for Hispanic women, 10.1; and for Asian/Pacific Islander women, 7.5.
Also, the 5-year survival rate was lower among all women with nonendometrioid subtypes, and black women had the lowest survival rates throughout each of the categories.

Racial Disparities in Cancer
“All of these trends—the rates of uterine cancer among black women exceeding those of white women, the higher incidence rates of nonendometrioid subtypes among black women, and the lower survival rates of black women for all uterine cancer—are very concerning,” Megan Clarke, Ph.D., lead author of the study and postdoctoral fellow in NCI’s Division of Cancer Epidemiology and Genetics, said.
And, these are not isolated findings. As we covered in 2018, a racial imbalance continues to be evident in regard to lower health care quality and higher cancer risk for Blacks, Hispanics and Latinos, along with individuals in poverty. Cancer incidence and mortality are generally highest among non‐Hispanic Blacks, the American Cancer Society (ACS) reported once again in 2019. “Cancer occurrence and outcomes vary considerably between racial and ethnic groups, largely because of inequalities in wealth that lead to differences in risk factor exposures and barriers to high‐quality cancer prevention, early detection and treatment.”
“We need to continue research to further understand these racial differences and disparities, in order to help us better predict risk and work toward prevention,” Dr. Clarke said of her study’s findings.
In 2019, an estimated 61,880 women in the U.S. will be diagnosed with uterine cancer. The ACS predicts that 12,160 deaths from the various forms of uterine cancer will occur this year. It is the fourth most common cancer for women in the U.S. and the sixth most common cause of cancer death for this population.
Sources: National Cancer Institute, American Cancer Society, American Society of Clinical Oncology