Researchers recently
reported that immunotherapy led to remission in 93 percent of patients with advanced leukemia. Though these ‘extraordinary’ results have only been evaluated in the short-term, the technique devised in this study has the potential to improve current and future immunotherapy treatments.
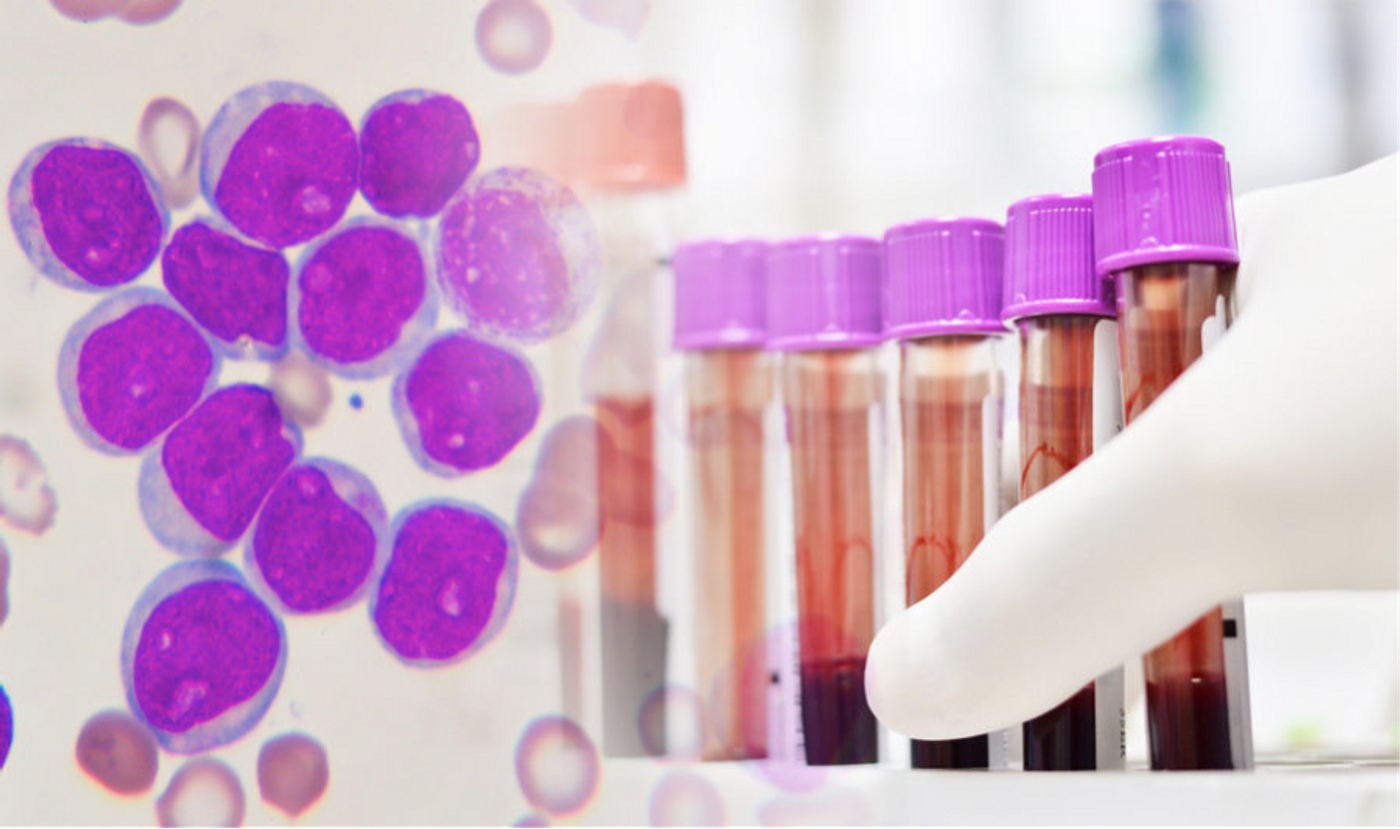
Immunotherapy is a type of cancer treatment that stimulates the body’s natural defenses to kill cancer cells. In some forms of immunotherapy, scientists harvest the patient’s immune T-cells and genetically alter them to carry a synthetic receptor molecule called a CAR (for chimeric antigen receptor). These specialized CAR-T cells are then able to recognize and destroy cancer cells that have a specific marker, known as CD19.
Though this technique has been shown to be powerful against cancer, the factors that determine the efficacy and toxicity of such treatment has been hard to study. To better understand how immunotherapy works and to improve on it, a team of researchers administered a defined mixture of CAR-engineered helper and killer T cells to patients with acute lymphoblastic leukemia (ALL). This is the first immunotherapy trial to use an even composition of the two T-cell types in patients.
Of the 29 leukemia patients who received the CAR-T cell mixture, 27 (93 percent) showed remission, with a total absence of cancer cells in their bone marrow. In addition of the 2 patients who did not experience remission, one patient was given a higher dose of the engineered cells and subsequently achieved remission.
"Patients who come onto the trial have really limited options for treatment. They have refractory, acute leukemia. So the fact that we're getting so many into remission is giving these people a way forward," said study leader Dr. Cameron Turtle.
But as extraordinary as the results appear, it is too early to conclude long-term victories with this treatment. The high percentage of remission was not sustained, as some patients relapsed even after traces of the cancer were seemingly gone. Two patients also relapsed with highly resistant leukemias that were immune to the CAR-T cells.
"This is just the beginning," Turtle said. "It sounds fantastic to say that we get over 90 percent remissions, but there's so much more work to do make sure they're durable remissions, to work out who's going to benefit the most, and extend this work to other diseases."
"In early-phase trials, you're continually learning. You don't expect results like these from early-phase trials. That's why these response rates are so extraordinary," said David Maloney, senior study author.
Additonal source:
Fred Hutchinson Cancer Research Center