Robotic surgery sounds like the stuff of science fiction, but reality is quickly catching up. In particular, a system called the TransOral Robotic Surgery (TORS) was able to help oropharyngeal cancer patients recover from tumor surgery without any incisions.
Head and neck squamous cell carcinoma (HNSCC) is the sixth common cancer worldwide. These include cancers of the tongue, tonsils, soft palate and pharynx. Each year there are nearly 650,000 new cases and 350,000 deaths.
Conventional surgery techniques for these cancers can often lead to significant pain and disfigurement. By contrast,
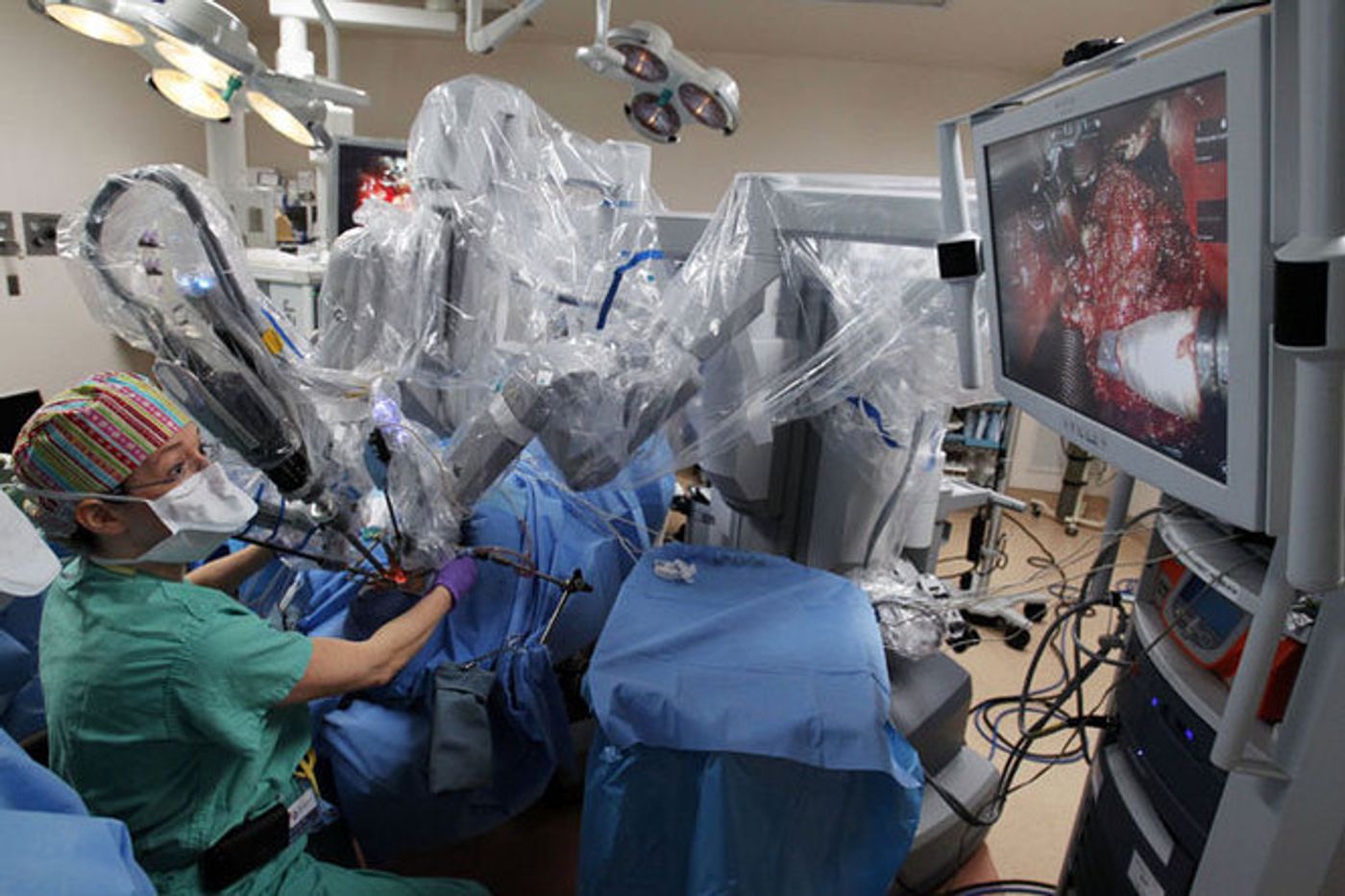
TORS, part of the da Vinci Surgical system proved to be much less invasive. The robotic system purportedly allows surgeons to get to the tumor via the mouth – no open incision on the face necessary.
By eliminating open wounds for the patients, doctors at the Henry Ford hospital found that patients recovered much quicker, some within mere days after surgery. "Within our study, patients treated with robotic surgery had excellent results and survival, irrespective of their p16 status,” said Tamer Ghanem, director of Head and Neck Oncology and Reconstructive Surgery Division in the Department of Otolaryngology-Head & Neck Surgery at Henry Ford Hospital, and the study’s lead author.
P16 is a protein marker of the human papilloma virus (HPV). The presence of the HPV type 16 virus is linked to oropharyngeal cancer. This status also appears to influence how well or how poorly a patient responds to treatment
"For non-surgical patients, several studies have shown that p16 positive throat cancers, or HPV- related throat cancers, have better survival and less recurrence than p16 negative throat cancers," said Ghanem.
In their study, the team analyzed a total of 53 patients with oropharyngeal cancer patients. Of this, 81 percent had HPV16+ oropharyngeal cancer.
Despite the p16 status, the study showed that the TORS robotic surgery was directly correlated with high survival and low cancer recurrence. In addition, the outcome appears to also improve when TORS was used in conjunction with chemotherapy or radiation therapy. Furthermore, the success of the surgery enabled lower doses of radiation, which benefited patients by reducing unwanted side effects.
Additional sources:
Henry Ford Health System,
Mayo clinic









