Bowel Cancer May be Tied to Prolonged Antibiotic Use
The onset of colon cancer may be tied to antibiotic use, reported scientists.
The importance of the microbiome has only being fully realized and appreciated in the recent years. And nowhere does the microbiome play a more important role than in the gut, influencing a variety of cancers, including colorectal or colon cancer.
Following these insights into the role of gut microbes, scientists wondered whether antibiotics – medicines designed to kill bacteria – can also affect our health outcomes. Indeed, several studies hinted at a link between antibiotic exposure and alterations in cancer risks. Some have blamed antibiotics for gastrointestinal conditions including irritable bowel syndrome (IBS) and celiac disease.
To study the connection between antibiotics and cancer, the researchers analyzed data that were collected from over 121,000 women between 30 and 55 in 1976 as part of a Nurses Health Study registry. But for the current study, researchers used data on a subset of these women, 16,642, who were at least 60 years old in 2004. This subset of women provided crucial information regarding antibiotic usage in their past. They provided detailed accounts of their health status, dietary habits, and other lifestyle factors.
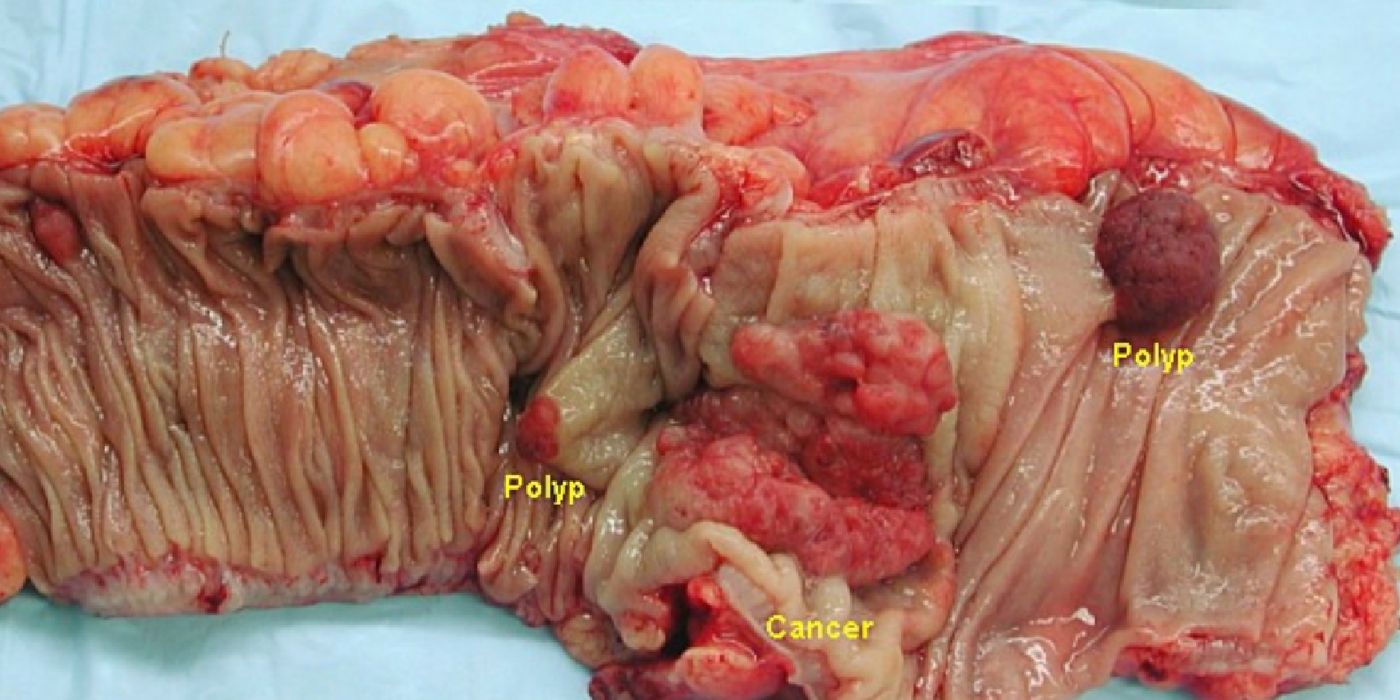
The team found that women who took antibiotics for 2 months in their 20s and 30s had a 36 percent increase in colon cancer risks. And just taking antibiotics for 15 days still increased chance of getting colon lesions verses for women who didn’t take antibiotics. Colon lesions, otherwise known as polyps or adenomas, have the potential to turn into colorectal cancer.
“This suggests that alterations in the naturally occurring bacteria that live in one’s intestines caused by antibiotics might predispose individuals to colorectal cancer,” said lead researcher Dr. Andrew Chan.
Colorectal cancer, also known as colon cancer or bowel cancer, is the third most commonly diagnosed cancer type in the world. Without proper removal, polyps can cause symptoms such as abdomen pain, rectal bleeding, weakness, and fatigue. According to their report, the incidence of colorectal cancer is “expected to increase by 60% to more than 2.2 million new cases and 1.1 million deaths by 2030.”
Chan hypothesizes that prolonged use of antibiotics could significantly disrupt the microbial diversity in the gut, which could promote the growth of polyps. However, he cautions against disrupting any antibiotic regimen without the supervision of doctors. Furthermore, Chan admits that the study does not provide a causal relationship between antibiotics and colon cancer; rather the results suggest a link between these two factors. “More research needs to be done to understand the interaction between alterations in one’s gut bacteria and future risk of colorectal cancer,” he added.
Additional sources: MNT