How a Cancer-Causing Virus Hides in Plain Sight
It’s estimated that nine out of ten people are infected with the Epstein-Barr virus (EBV). The virus stays dormant for most of the time, but in some cases, it rears its ugly self to cause lymphoma in immunocompromised people. How does the virus manage to conceal itself so well within our bodies only to strike when we’re most vulnerable? Scientists think it’s the virus’ ability to masquerade within our immune cells.
Since its discovery in the 1960s, the Epstein-Barr virus has proven to be increasingly more complex. Also called human herpesvirus 4 (HHV-4), EBV is one of eight viruses in the herpes family. It’s infamous for causing “the kissing disease,” otherwise known as mono (short for mononucleosis), in teenagers.
But even more threatening than causing swollen lymph glands and fevers, EBV was the first virus shown to cause cancer directly. In particular, EBV infection is linked to two types of lymphomas (Burkitt’s and Hodgkin’s), stomach cancer, and some types of head and neck cancer (nasopharyngeal carcinoma).
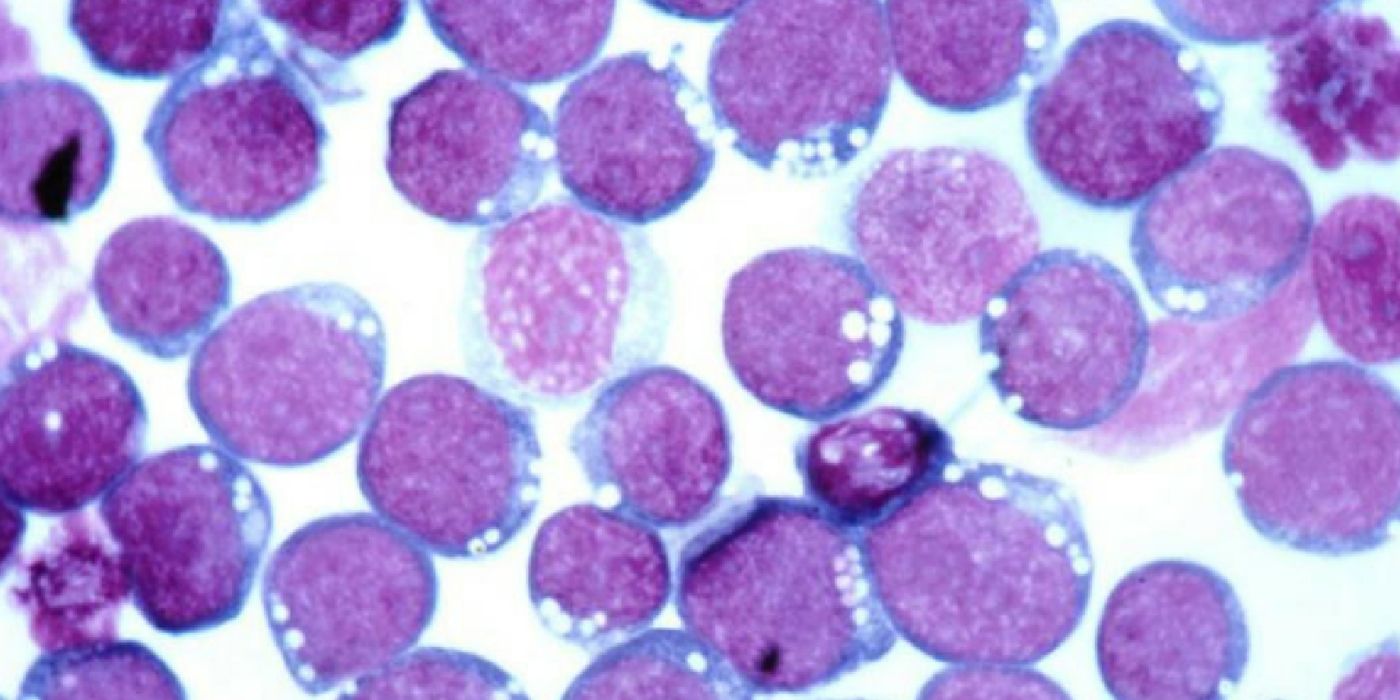
EBV typically persists in a type of immune cells called B cells - these are white blood cells that respond to infection. And from within, the virus manages to boost B cell division while simultaneously stalling cell death.
"The virus actually taps into the B cell's normal protection against apoptosis," said Micah Luftig, an associate professor of molecular genetics and microbiology at Duke University, and the study's senior investigator.
By this mechanism, EBV manages to immortalize the B cells, and thereby furthering its own survival. Specifically, as the infection progresses, EBV will blend in with memory B cells, a B-cell subtype that circulate throughout the body, ready to respond to attacks by known pathogens.
"All of this is about establishing latency," Luftig said. This is how EBV hides in plain sight. The team used a technique called BH3 profiling to “query mitochondrial regulation of apoptosis,” which allowed them to glimpse the mechanism behind B-cell immortalization by the virus. Key to the story is a protein called EBNA3A (Epstein-Barr Nuclear Antigen 3A), which plays an crucial role in the B cell’s abilities to resist apoptosis.
Ultimately, Luftig hopes this line of research could lead to new treatment options and benefit immunocompromised people who are at much higher risk of developing cancer from the Epstein-Barr virus.
Additional source: Duke University via EurekAlert!