Scientists Battle Cancer with the Poliovirus
With cancer putting up such strong fight, scientists are resorting to more unconventional therapies to give them the edge. The Zika virus was recently co-opted to fight deadly brain cancer, and now, scientists are turning their attention to the poliovirus.
The radical approach of using the poliovirus to kill cancer made big headlines in 2014. At that time, a group of researchers from Duke University reported that a lab-engineered hybrid virus was capable of killing cancer cells. The virus is a combination of the poliovirus and the rhinovirus, called PVS-RIPO. But while it showed promising results against cancer cells and was given to a limited number of patients as an experimental therapy, the team didn’t know the precise mechanisms behind how this virus worked.
"We have had a general understanding of how the modified poliovirus works, but not the mechanistic details at this level," said co-senior author and Duke neurosurgery professor Matthias Gromeier. "Knowing the steps that occur to generate an immune response will enable us to rationally decide whether and what other therapies make sense in combination with poliovirus to improve patient survival."
The same team persisted and recently published a follow up study, in which they detailed how the modified poliovirus unleashes its attack against cancer cells.
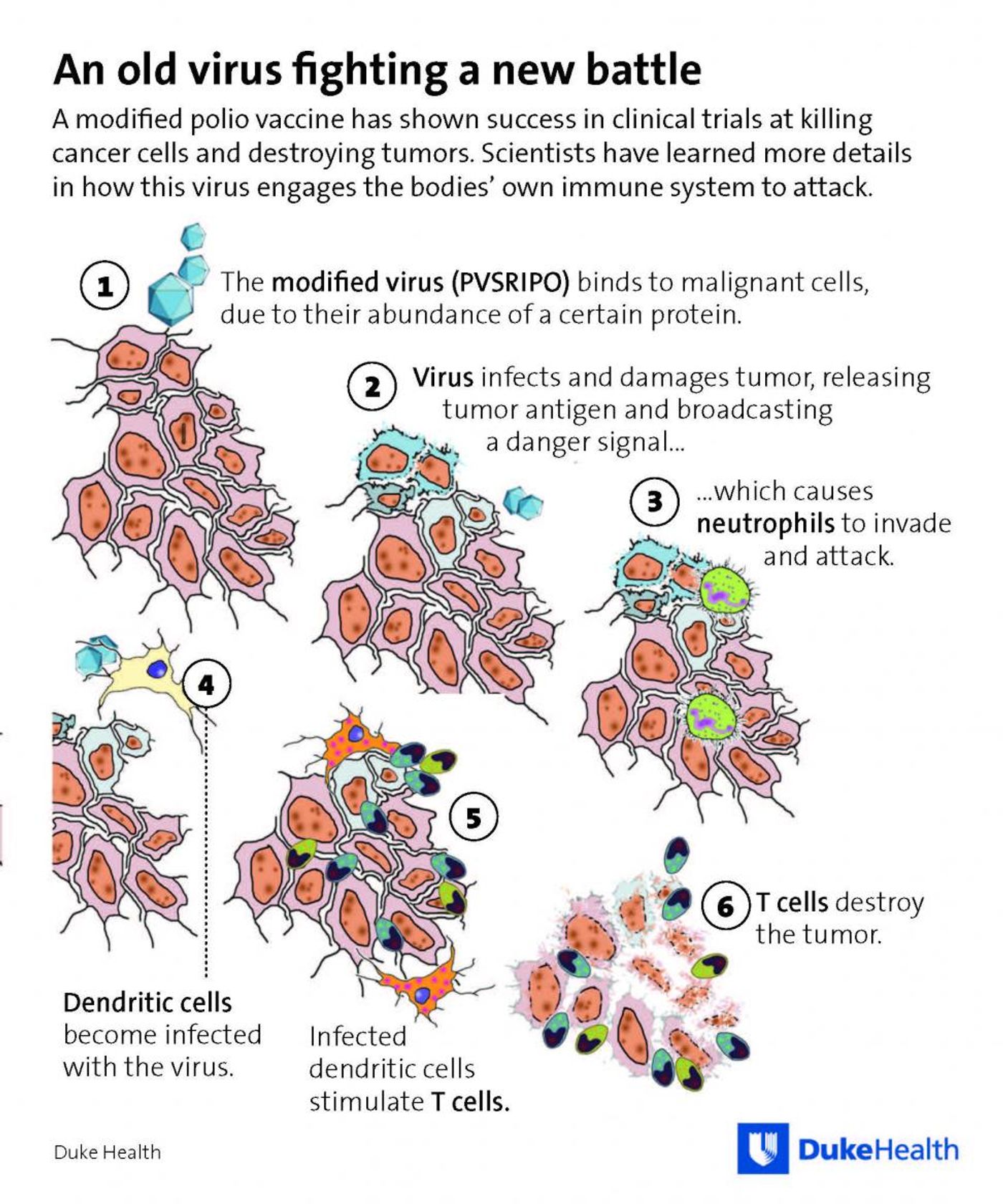
"Not only is poliovirus killing tumor cells, it is also infecting the antigen-presenting cells, which allows them to function in such a way that they can now raise a T-cell response that can recognize and infiltrate a tumor," says Smita Nair, the co-senior author on the study with Grimier. "This is an encouraging finding, because it means the poliovirus stimulates an innate inflammatory response."
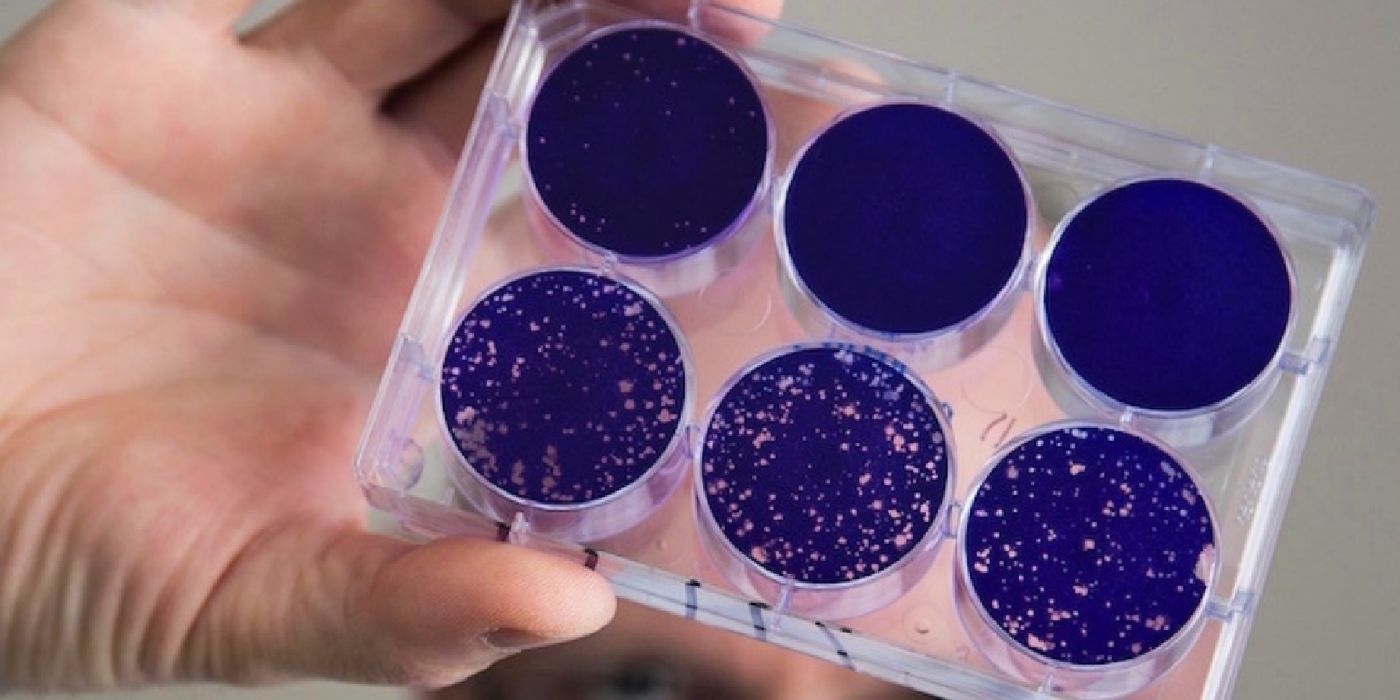
The results were observed in human melanoma and breast cancer cell lines, and subsequently validated in mouse models. The team believes the same mechanism of attack could apply to several other cancer types that express the CD155 marker.
"Because PVSRIPO naturally targets and destroys cancer cells from most common cancer types (pancreas, prostate, lung, colon, and many others), it can be directed against these cancers as well," says Gromeier. "To establish this in the clinic, we plan future clinical trials in patients with cancers other than brain tumors."
PVS-RIPO earned the FDA’s “breakthrough therapy” designation last year, based on early success in clinical trials. If promising results continue, the treatment could be on the shortlist to receive approval.
Additional sources: Duke University, MNT