England's Cancer Screening for Trans and Non-binary People Has Major Gaps
In July 2017, The National Health Service (NHS) and Public Health England published a guidebook called “NHS population screening: information for transgender and non-binary people.” The NHS is tasked with providing free, universal public health services -- England, Scotland, Wales and Northern Ireland all have their own branch of the NHS, and the term can also describe the services as a group. The booklet is intended to inform transgender people and non-binary people about the types of health screenings they will automatically be assigned in England. Based on its guidance, many people will miss being screened for health issues they are biologically more prone to get.
Transgender people are individuals who identify as a sex different from the one they were assigned at birth. Nonbinary people do not identify as either primarily male or female within the common gender binary system. The NHS reported in 2017 that in the past five years, the number of children referred to gender identity clinics in Great Britain quadrupled. Also in 2017, the number of people identifying as LGBTQ in the UK rose above 1 million for the first time.
Within the NHS’s 24-page pamphlet on screenings for transgender and non-binary people, several regulations have gained attention in the media. For example, transgender men (who were identified as female at birth) will not be offered routine cervical and breast cancer screenings. Unless their uterus and cervix have been removed, which is currently the case for only a minority of this population, this group is still at risk for cervical cancer. Each year, about 900 women in Britain die of cervical cancer.
In contrast, while the Center of Excellence for Transgender Health of the University of California recognizes, “Pelvic exams to obtain pap smears may be challenging for transgender patients,” it advises transgender men be screened with the same guidelines as non-transgender women.
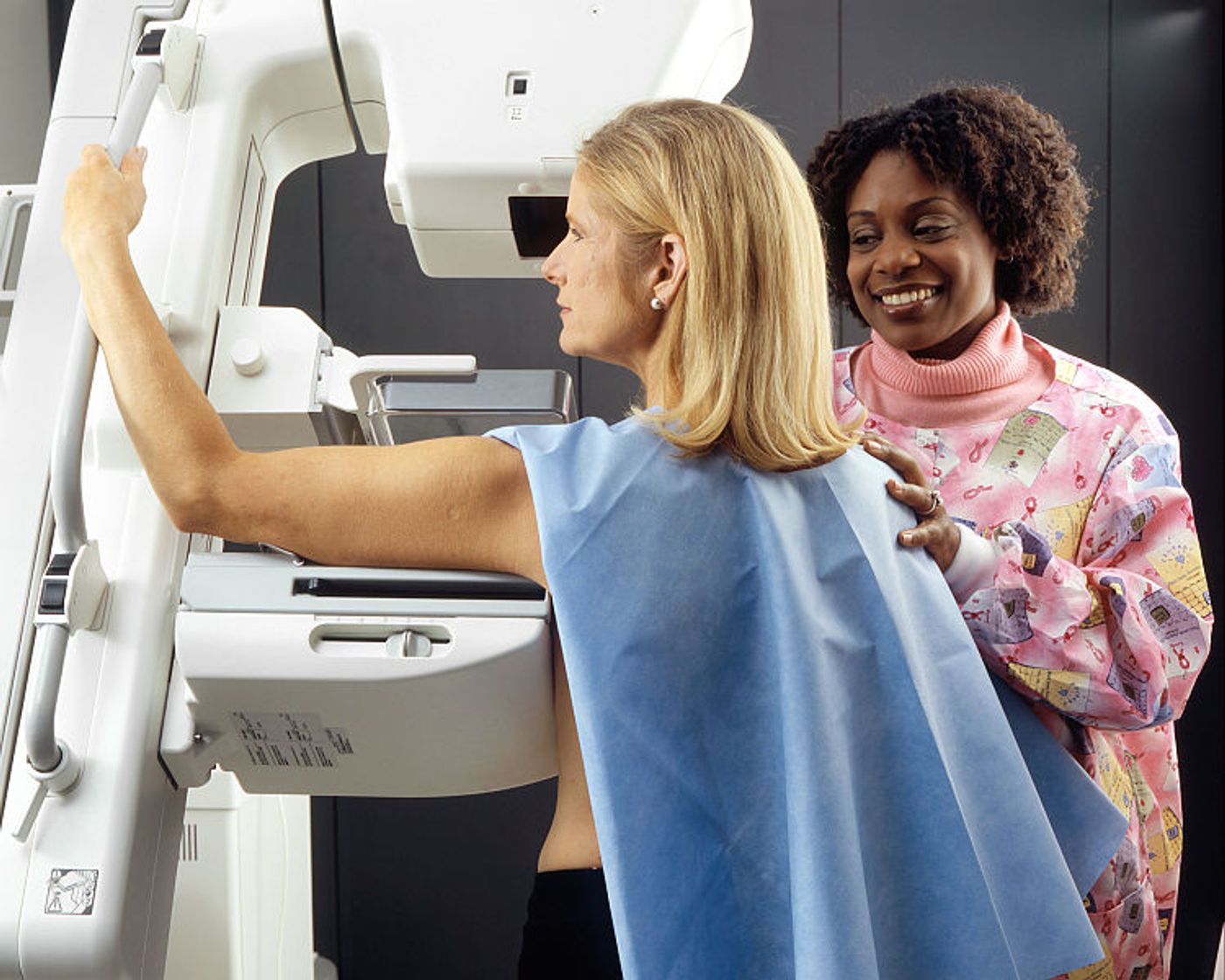
“If you are a trans man aged 50 to 70 who is registered with a GP as male, you won’t be invited for breast screening,” the NHS document states. NHS breast cancer screening is believed to save 1,300 lives annually, according to the Daily Mail. Transgender women registered as female will be invited for breast cancer screenings. This is generally recommended for trans women who have grown breast tissue.
Also, men within the UK are generally screened for abdominal 
The screening invitations are computer-generated based on the patient’s age and registered sex. Essentially, people who register with their doctor under their newer-identified sex will not be screened for diseases they are at higher risk for because of their sex-at-birth. This system places them at greater risk of missing out on the often life-saving benefits of early identification of serious health problems. In order to be automatically signed up for testing aligned with risks associated with their birth sex, they would have to formally register under their birth sex.
Transgender women registered as women will be invited to have cervical screenings, though they do not possess cervixes. Transgender men registered as men will also be invited for AAA screenings, though they do not biologically have an increased risk for this health issue.
“Following engagement with the LGBT community, we produced a guide to help trans people understand what screening is available in England,” Director of Screening Anne Mackie says. The NHS advises more information is available for transgender, gender fluid (having an unfixed or fluid gender) and non-binary individuals at www.nhs.uk/trans-health.