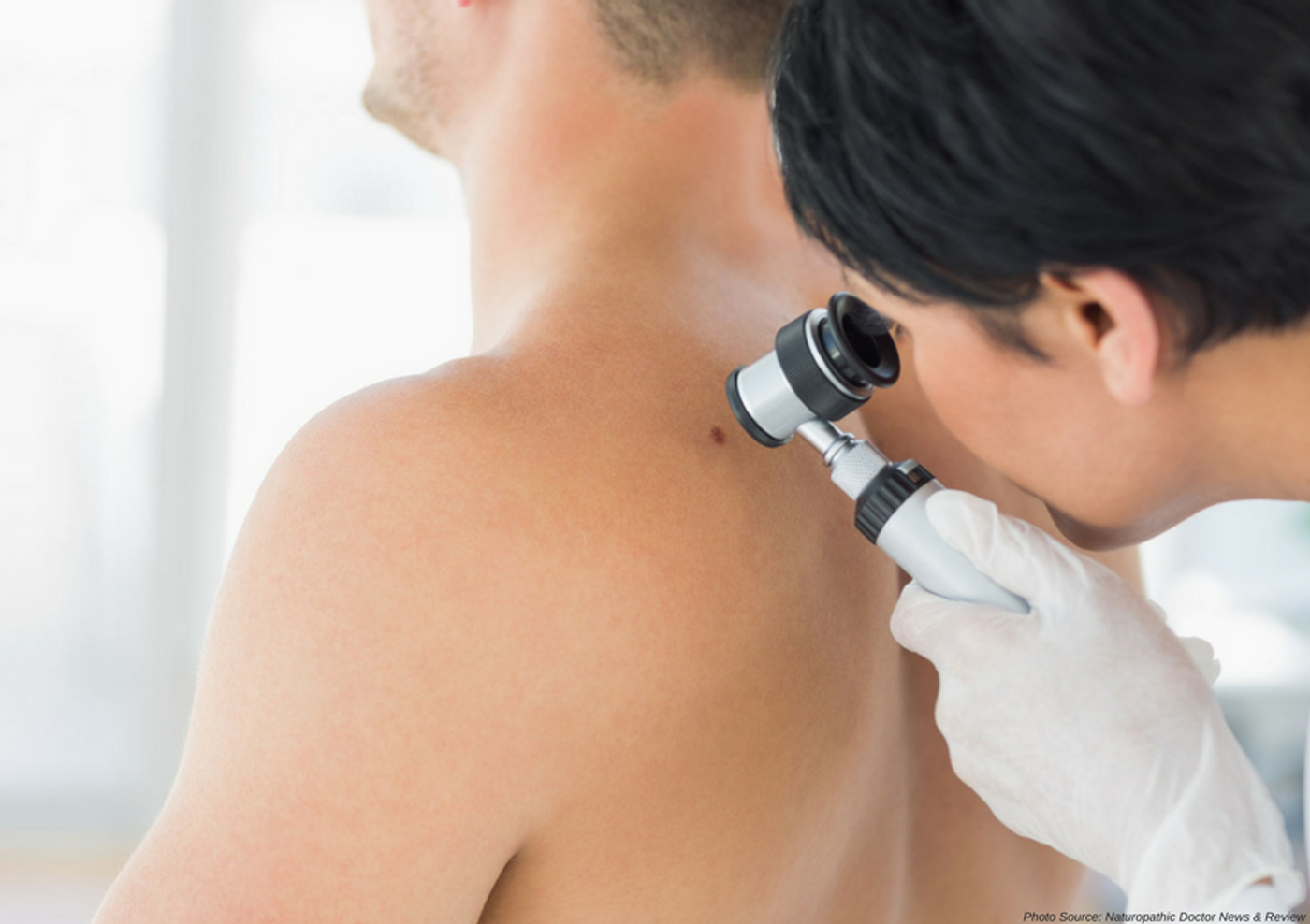
Artificial Mole Tattoo for Early Cancer Detection
Tattoos for medical purposes? You bet.
In the past few years, researchers have explored the use of biologically sensitive ink to be indicators of medical issues like dehydration for athletes, blood glucose increases in diabetes, body temperature for infections, and epilepsy detection for medicine delivery. Some of the intent of this research is to further expand the idea of “wearables” and blend that with biotechnology. Still, for many others, the true goal with this biotechnology is to positively affect patients and proactively address health concerns.
The most recent revelation, published in Science and Translational Medicine in late April 2018, is a biomedical tattoo, that will detect certain cancer types through the use of implanted engineered cells designed to darken, like an a mole, under certain conditions. According to the researchers, the idea for this biomedical tattoo came from concerns about the 14 million new cases of cancer per year across the globe. Scientists and providers know that early detection of cancer during the asymptomatic period can be immensely critical to the prognosis and subsequent successful treatment of patients in eradicating their disease. Many cancers, if not caught early, are more resistant and challenging to treat. The group found the commonality of long term hypercalcemia in cancers of the breast, colon, prostate, lung, gastrointestinal, and in hematological malignancies. Calcium (Ca2+ is required by all cells in the body and contributes to normal structure and function, signal transduction, cell proliferation, apoptosis, adhesion, differentiation, and motility. It has also been discovered to have a role in messaging for cancer, contributing to cancer growth. Additionally, long term hypercalcemia is a result in cancer because tumor cells, primary, metastases, and immune cells secrete humoral factors causing a disruption in Ca2+ balance in the body. The group hypothesized a novel way to assess long term levels of Ca2+ in the blood whereby hypercalcemia levels consistent with cancer presence would be detected.
The researchers utilized the calcium sensing receptor (CaSR) which is naturally functions with high sensitivity to levels of Ca2+ in the blood. Increased Ca2+ concentration activate CaSR to inhibit the secretion of parathyroid hormone. CaSR is capable of detecting mild to moderate blood hypercalcemia, as defined by the study as 5.6 to 10mg/dL, which often goes unnoticed in the patient during very early stages of cancer growth. The biomedical tattoo, made up of engineered cells to express CaSR, have a rewired signaling pathway for CaSR activation. Upon CaSR activation, the redesigned signaling cascade leads to expression of tyrosinase which produces melanin. The design was intended to detect the accumulation of melanin as a pigmented mark, or tattoo, that would signal the long-term presence of blood hypercalcemia. The body’s normal Ca2+ homeostasis mechanisms would not be affected because the feedback pathways between blood Ca2+ and PTH secretion respond within minutes of an increase or decrease in Ca2+ concentration.
The group validated their theories using in vitro cultures with hypercalcemic solutions followed by in vivo mice models using wild-type mice with both asymptomatic hypercalcemic carcinomas and normocalcemic adenocarcinoma. Their theory proved true; blood concentration profiles confirmed correlation between presence of pigmented marks and long-term mild to moderate hypercalcemia from the asymptomatic hypercalcemic mice. In addition, the group explored the ability to visualize the biomedical tattoo in ex vivo porcine skin more closely aligned with human skin than that of murine mammals.
The use of a biomedical tattoo is an incredibly interesting theory that warrants additional investigation and exploration for early detection of cancer.
Sources: Science and Translational Medicine, Nature, Harvard Gazette, Journal of Thoracic Disease, Sub-cellular Biochemistry Journal,