Measuring Pulse Transit Time as a Replacement for the Inflatable Cuff
Many people deal with one disease or another every day of their life. Most require checking on things like blood sugar for diabetes or blood pressure for hypertension. The development of easy to use tools to monitor these symptoms has been of keen interest to both doctor and patient.
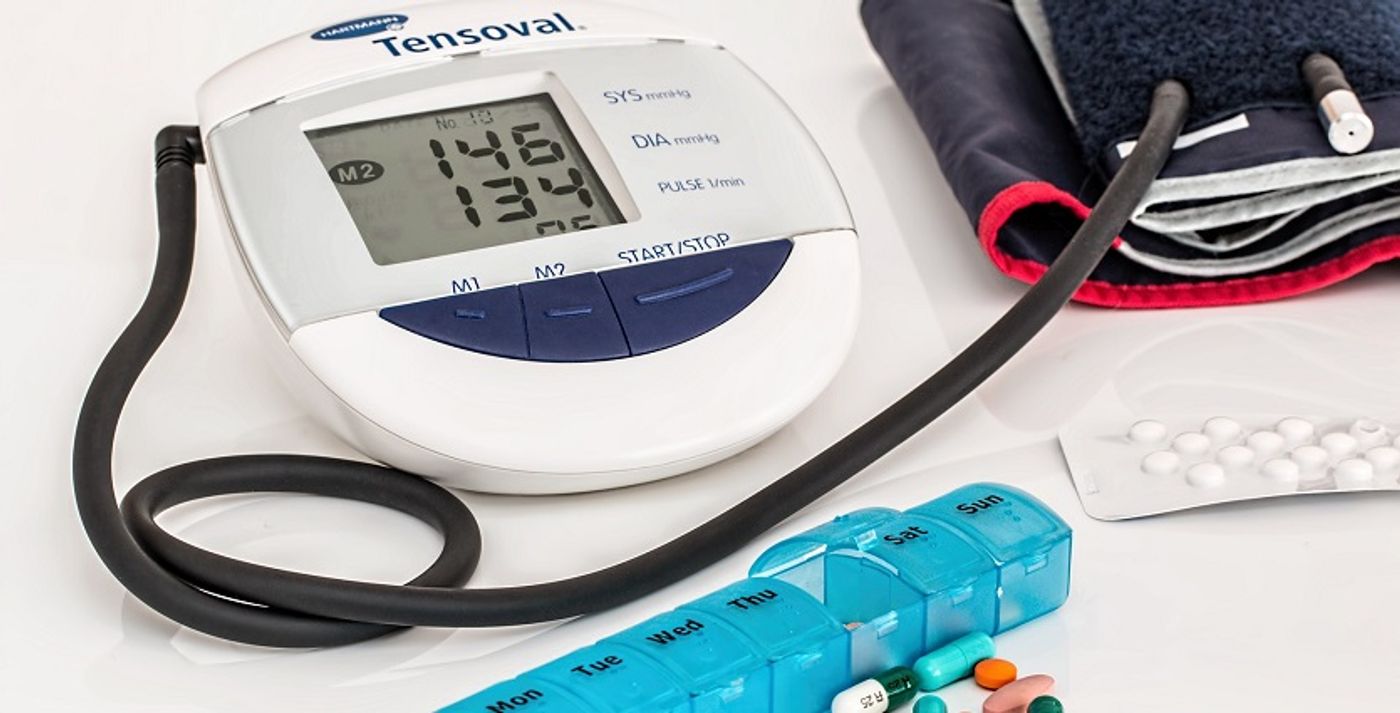
For diabetes, small portable testing tools have been available for years. For hypertension patients and blood pressure monitoring, not so much. The old inflatable cuff is still the go-to method for its simplicity, but you can’t be carrying one around all the time. Conducting the test on yourself may also result in biased results (who doesn’t want perfect blood pressure, even if it’s a little fib). A tool is needed to give hypertension patients an easy and portable way to check their blood pressure.
A study out of the University of Rochester intended to investigate if pulse transit time (PTT) could replace the inflatable cuff method. Pulse transit time is a measure of the time delay between ECG waves from two parts of the body, which can then determine blood pressure. While this method still requires special machinery, further development could very well lead to an easy to use portable blood pressure monitor.
The team gathered a group of 31 patients and retrieved conventional pulse time transit readings and manual cuff readings from all of them. They used two different setups for the pulse time transit measurements, with monitors at the ear and finger for one, and ear and toe for the other. The manual cuff measurements were also performed by an actual doctor, rather than a machine. Finally, they used various methods to alter blood pressure to ensure accurate results across multiple settings.
The team found that the toe-ear setup was the closest to the manual cuff in its readings. They had some concerns about the data from some of the altered blood pressure readings. Combined with some other odd readings of various blood pressure characteristics, these concerns led the team to conclude pulse transit time methods may not be useful in the real world use. Many of the studies supporting this method used a limited amount and type of patient, where this relatively larger group gave more realistic results.
The study concludes, “In conclusion, finger PAT and cPTTs detected via the PPG waveform peaks may not generally correlate well with BP in a person. Toe PAT may be a superior marker of changes in systolic BP in particular but perhaps not good enough. Innovations are needed in order to achieve cuff-less BP measurement via PTT.”
Sources: Nature Scientific Reports, IEEE Sensors