HAX-1 is an anti-cell death protein that could protect cardiac cells during traumatic cardiovascular events like heart attack and heart failure. In a study published this week in
Proceedings in the National Academy of Sciences (PNAS), scientists from the
University of Cincinnati (UC) explored the mechanism behind harnessing this protective behavior into a way to keep cardiac cell damage to a minimum after a damaging event.
After observing HAX-1 levels decreasing and cell death levels increasing after heart attacks in mice, UC researchers thought there might be away to reverse this behavior to prevent cell death.
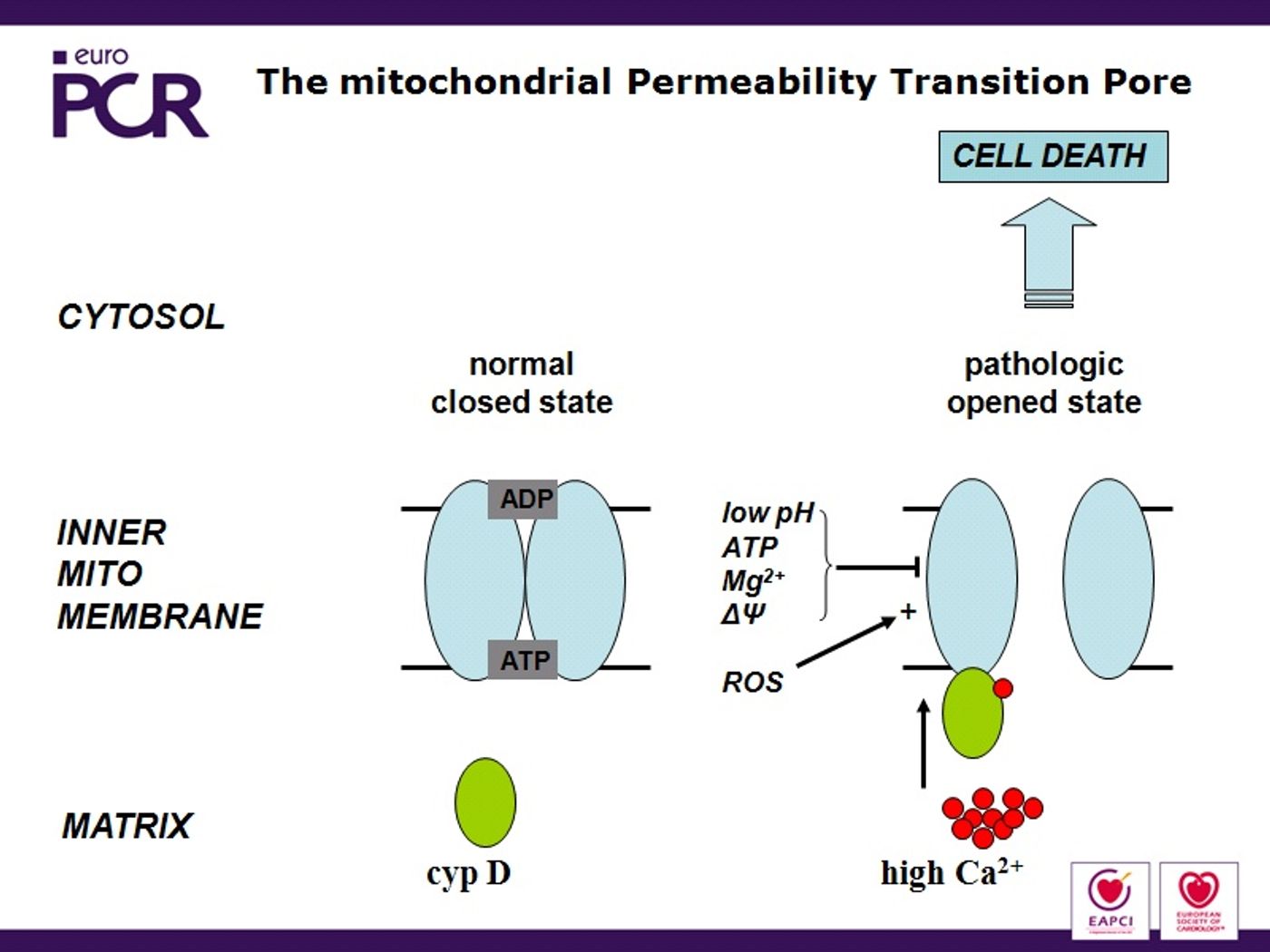
During oxidative stress, the mitochondrial permeability transition pore (MPTP) opens and results in ATP depletion and cell death (
Journal of Molecular and Cellular Cardiology). HAX-1 manages this activity on a regular basis to maintain the integrity of the heart tissues. Theoretically, HAX-1 could be manipulated to do damage control during heart attacks and heart failure by inhibiting energy loss and necrotic cell death from the MPTP.
“Basically, what we have found is that this protein is inhibiting cell death through a pathway that is known to cause death,” UC’s Dr. Chi Keung Lam explained.
According to
Circulation, cardiac tissue can resist damage from oxygen depletion for about 15 minutes, but over time cell death will increase without access to oxygen, leading to a “spectrum of reperfusion-associated pathologies,” also known as reperfusion injury. Increasing levels of HAX-1 during events of oxygen depletion, like heart attacks, could lessen the long-term impact of reperfusion injury.
ATP depletion and cell death from an opening of the MPTP occurs in more than just heart disease. Cell damage from some cases of cancer, stroke, and liver disease are connected to the MPTP. HAX-1 and similar proteins in other organs have the potential to prevent damage during traumatic events in patients suffering from these diseases.
Check out the following UC San Francisco video from a previous study involving stem cells in mice for treating heart attack patients.