High Blood Pressure May Raise Brain Damage Risk
New research has suggested that people that have higher than normal blood pressure before they reach age 50 are more likely to have brain damage when they get older. An assessment of data from 37,041 people in the UK Biobank, which includes MRI and health information, revealed that diastolic blood pressure (the bottom number in blood pressure readings) is connected to brain damage later in life, even when the diastolic blood pressure is within what is considered a normal range. The findings have been reported in the European Heart Journal.
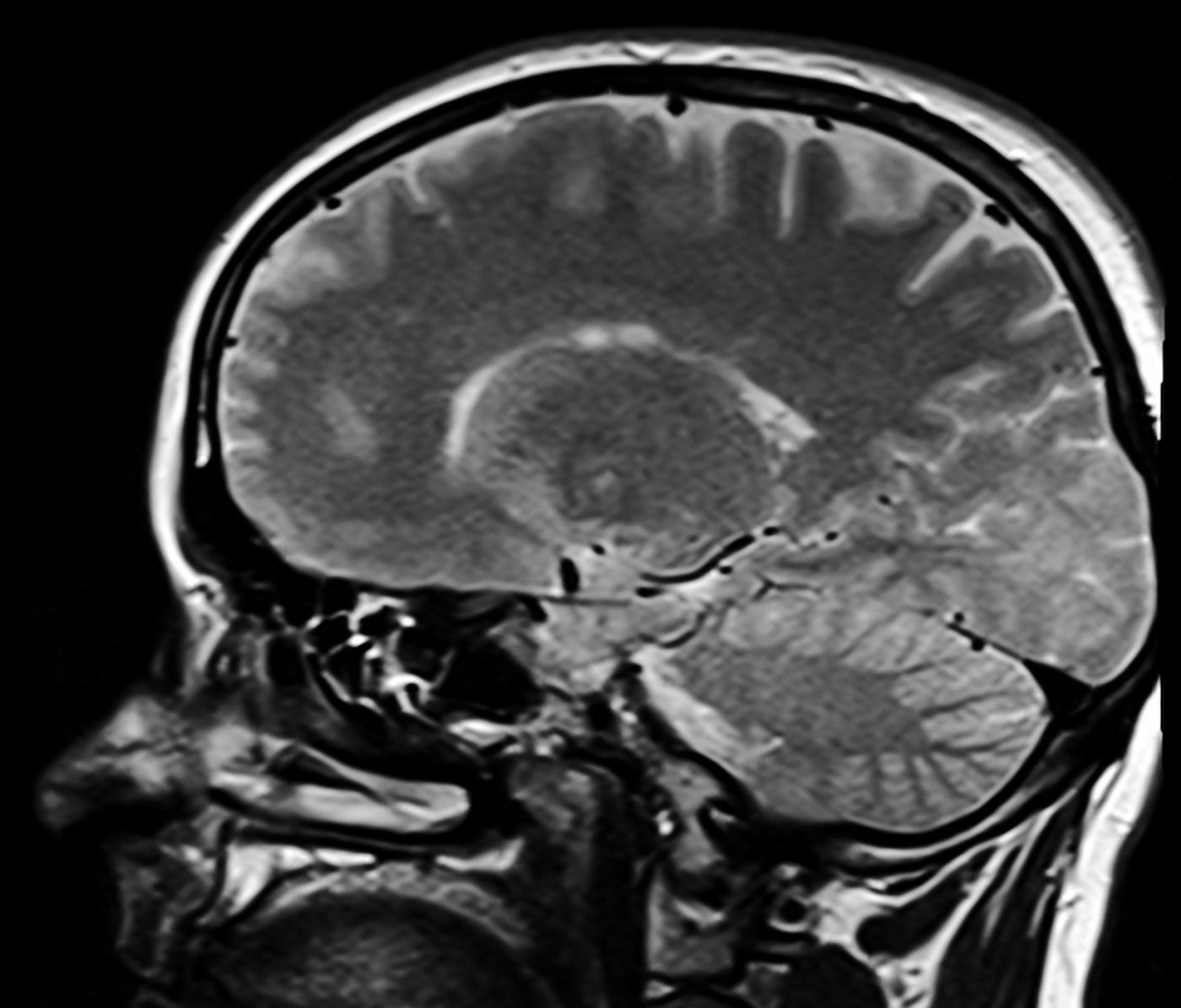
In this study, the researchers looked for bright regions on MRIs, which are thought to indicate brain damage called "white matter hyperintensities" (WMH). The blood vessels in these areas suffer damage due to age and blood pressure.
"Not all people develop these changes as they age, but they are present in more than 50 percent of patients over the age of 65 and most people over the age of 80 even without high blood pressure, but it is more likely to develop with higher blood pressure and more likely to become severe," said first study author Dr. Karolina Wartolowska, a clinical research fellow at the Centre for Prevention of Stroke and Dementia at the University of Oxford, UK.
The researchers took into account risk factors like diabetes and age in their investigation.
"To compare the volume of white matter hyperintensities between people and to adjust the analysis for the fact that people's brains vary slightly in size, we divided the volume of WMH by the total volume of white matter in the brain. In that way, we could analyze the WMH load, which is the proportion of the WMH volume to the total volume of white matter," Wartolowska explained.
Higher levels of WMH were also linked to systolic blood pressure, but the association was stronger for diastolic blood pressure. Any increase in blood pressure, even when it's below the threshold for therapeutic intervention, is connected to an increase in WMH, an association that was even more significant when people were taking high blood pressure medication.
"We made two important findings. Firstly, the study showed that diastolic blood pressure in people in their 40s and 50s is associated with more extensive brain damage years later. This means that it is not just the systolic blood pressure, the first, higher number, but the diastolic blood pressure, the second, lower number, that is important to prevent brain tissue damage," said Wartolowska.
"The second important finding is that any increase in blood pressure beyond the normal range is associated with a higher amount of white matter hyperintensities. This suggests that even slightly elevated blood pressure before it meets the criteria for treating hypertension has a damaging effect on brain tissue."
Researchers still aren't exactly sure how WMH develops. It's been suggested that chronically elevated blood pressure slowly stresses the vessels, causing leaks in the linings; when these leaks get bigger, WMH happens. Another possibility is that diastolic blood pressure could lead to a stiffening of larger blood vessels, raising blood pressure pulses in the brain. That could cause high blood pressure during every beat, a rapid change in blood pressure, and a reduction in blood flow between beats, leading to WMH.
More work will be needed to understand how WMH forms, and exactly how it's connected to blood pressure.
Sources: AAAS/Eurekalert! via European Society of Cardiology, European Heart Journal