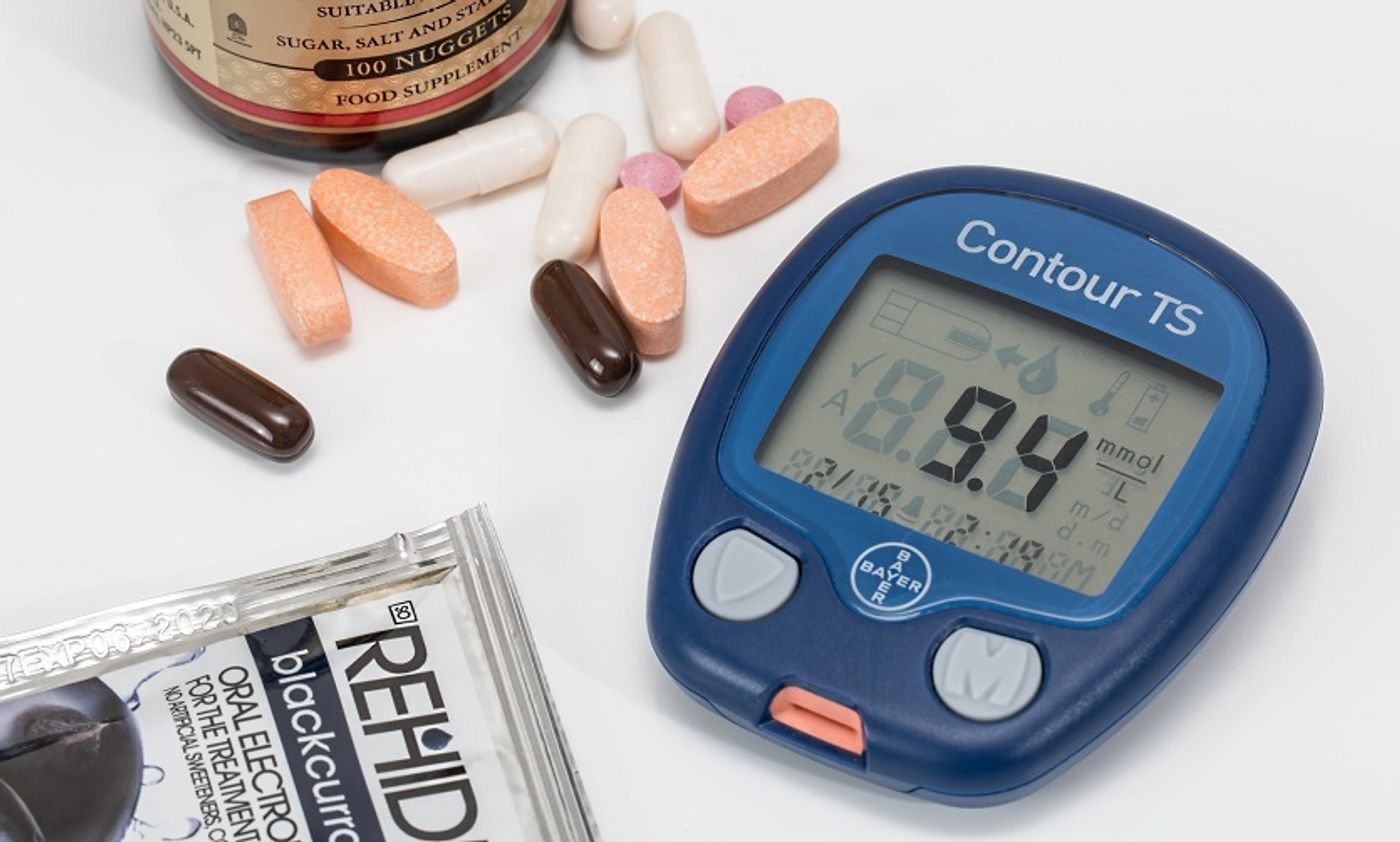
Does Impaired Glucose Tolerance Increase Heart Damage After a Stroke?
Diabetes is a looming threat to the world’s healthcare systems. Diagnoses of its precursors, impaired glucose tolerance, and impaired fasting glucose are also rising. Cardiovascular risk is closely tied to diabetes, but its ties to its precursor states are still unknown.
Across the world, diabetes has been a rising threat for years. While diabetes itself is manageable, it is often followed by cardiovascular disease. The research linking these two health issues can be traced back for decades, but diabetes doesn’t just happen overnight.
Impaired glucose tolerance (IGT) is when a person’s blood sugar levels remain elevated over long periods, but diabetes can not technically be diagnosed. As you might have pieced together, impaired glucose tolerance is often followed up by diabetes. Research focusing on impaired glucose tolerance has only recently gained traction, with many previous studies only looking at it peripherally to diabetes. Focused studies are required to reveal if a real cardiovascular risk for patients with impaired glucose tolerance exists.
That is where a team from the Almazov National Medical Research Center in Russia came in. In a new study, they looked at if IGT increases the damage done to the heart after a stroke. They also looked into how two diabetes drugs, metformin and liraglutide, each with a different method of controlling blood glucose levels, might protect the heart from this damage.
The study centered around a rat model, where they tested four groups. Group one would represent a diabetes control, group two would represent IGT alone, with groups three and four being IGT treated with either metformin or liraglutide. After eight weeks, both the IGT and IGT + metformin groups began outpacing the diabetes group in weight gain, a normal effect of high blood glucose. The IGT + liraglutide group’s weight gain began to slow, consistent with liraglutide’s appetite-suppressing effects. Finally, the blood glucose levels of the groups treated with metformin and liraglutide were lower than the IGT and diabetes groups.
The team then looked at the left ventricular heart pressure, a measurement of heart health, during ischemia in all four groups. Both untreated groups had reductions in pressures compared to healthy rats during a stroke. The metformin group saw a slower rise but eventually came to the same pressure. The liraglutide-treated group did surprisingly well by comparison, with left ventricular pressure comparable to healthy rats. Finally, infarction size (the size of dead tissue after ischemia/stroke) in IGT and diabetes groups was much larger than in healthy rats. Both metformin and liraglutide reduced this infarct area down to healthy rat levels.
One of the biggest takeaways from this study was the similarities between IGT and diabetes groups. Both groups had similar issues handling ischemia compared to healthy rats. The team notes this could point to impaired glucose tolerance as a blanket cause of cardiovascular issues for diabetes and IGT, although a high-fat diet control had similar detriments. As far as the cardioprotective effects of metformin and liraglutide, both managed to reduce infarct size. Liraglutide pulls out ahead, though, by controlling the left ventricle pressure during ischemia.
The study concludes, “Both MET and LIRA have cardioprotective effect that is independent on their influence on glucose metabolism. Cardioprotective property of LIRA includes both improvement of hemodynamic parameters and infarct-limiting action, whereas use of MET only decreases myocardial damage volume.
Sources: Nature Scientific Reports, HCPLive