Doctors often advise late-stage renal disease patients to stop taking blood pressure medications before they reach the stage where they require dialysis to rid the blood of waste, salt, and water. However, a new study published in
Nephrology Dialysis Transplantation provides evidence for patients to resume taking these medications in order to reduce the risk of heart disease.
Taking blood pressure medicine in late-stage renal disease runs the risk of the patient having dangerously high potassium levels, but scientists in this study say that the medications are less risk after a patient has begun receiving peritoneal dialysis. Renal disease patients, who are at a higher risk of developing cardiovascular disease than health people, could benefit from receiving blood pressure medication, mainly angiotensin-converting enzyme inhibitors (ACEIs) and angiotensin II receptor blockers (ARBs), the new study shows.
From the Los Angeles Biomedical Research Institute at Harbor-UCLA Medical Center, a team of researchers reviewed almost five thousand medical records of American renal disease patients who began peritoneal dialysis between 2007 and 2011. Of the 42 percent who filled prescriptions for either ACEIs or ARBs, the researchers saw an approximately 16 percent lower risk of heart attack, stroke, and death. Pending the success of randomized clinical trials demonstrating a causal relationship, scientists are prepared to recommend that late-stage renal disease patients undergoing peritoneal dialysis receive either ACEIs or ARBs to reduce their risk of heart disease.
“These findings indicate doctors should consider using or re-starting ACEIs and ARBs as first-line blood pressure medications for patients undergoing peritoneal dialysis,” said corresponding author Jenny I. Shen, MD.
The kidneys serve to remove waste and excess salt and water from the blood, and certain conditions like diabetes and high blood pressure can cause the kidneys to lose function. End-stage renal disease occurs after chronic kidney disease has persisted for years, and either regular dialysis or a kidney transplant is required for the patient to survive.
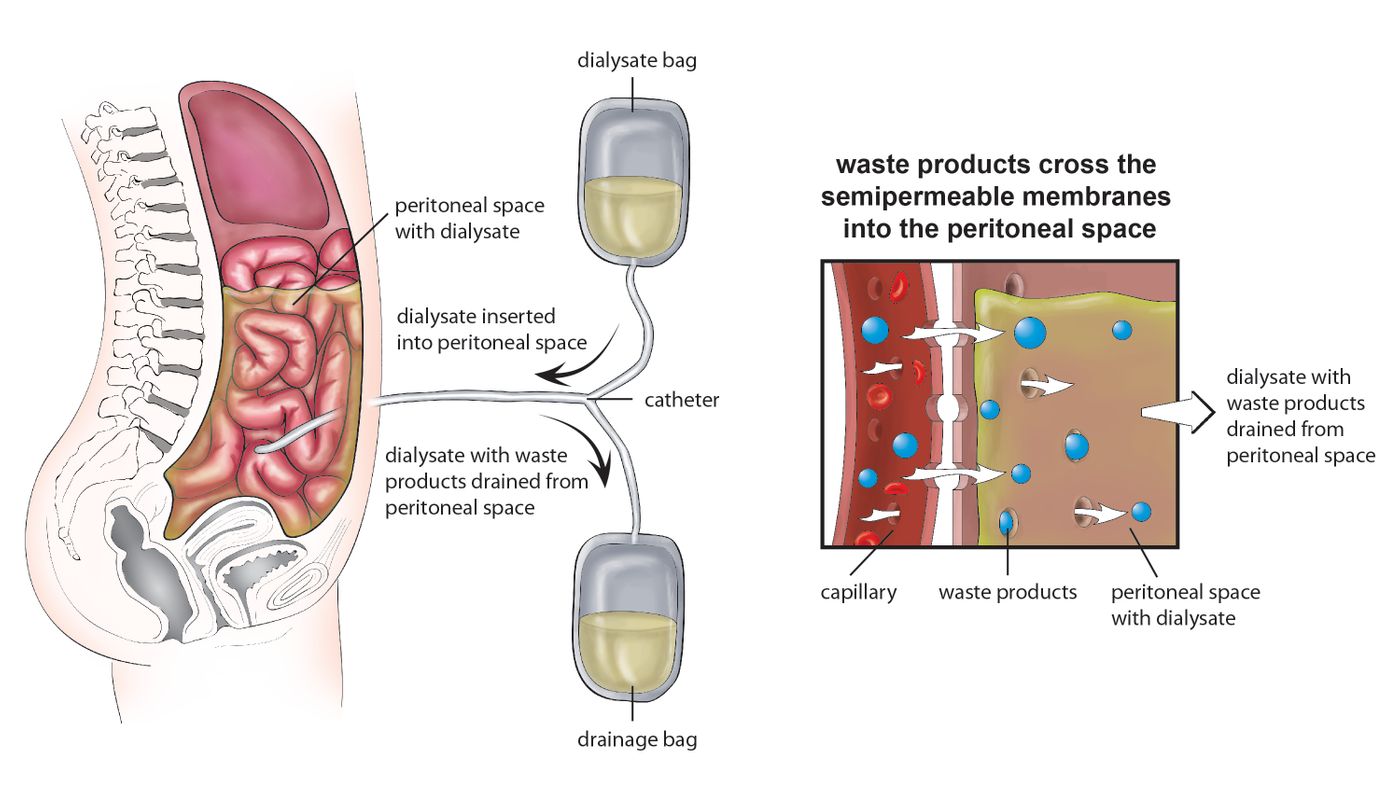
The researchers in this study looked at renal disease patients who received peritoneal dialysis, a type of treatment that cleanses the blood through a surgical placement of a catheter that releases a fluid called dialysate. This fluid is washed in and out of the body in cycles until the blood-filtering process is finished.
ACEIs block the production of a hormone that circulates in the blood, angiotensin II, that is known to cause high blood pressure from constricting the blood vessels. As their name suggests, ARBs also target the function of angiotensin, but in certain cases ARBs might be chosen over ACEIs because they don’t affect the hormone renin like ACEIs do.
After the first year of dialysis, more than 20 percent of late-stage renal disease patients die, and almost half of these deaths are because of cardiovascular disease. Re-introducing blood pressure medications for these patients could reduce the prevalence of cardiovascular-related death. Additionally, for chronic kidney disease patients who have not yet reached the late stage, blood pressure medications are also helpful for slowing the progression of kidney damage as well as decreasing risk of cardiovascular disease.
Sources:
Los Angeles Biomedical Research Institute at Harbor-UCLA Medical Center, National Kidney Foundation,
MedlinePlus,
Circulation,
Baylor University Medical Center Proceedings