People with type 2 diabetes are more than twice as likely as people without diabetes to develop coronary artery disease. With the prevalence of type 2 diabetes on the rise in the United States, health professionals can expect rates of coronary artery disease to rise as well. Researchers from the Royal Melbourne Hospital in Australia are on the move to address this problem.
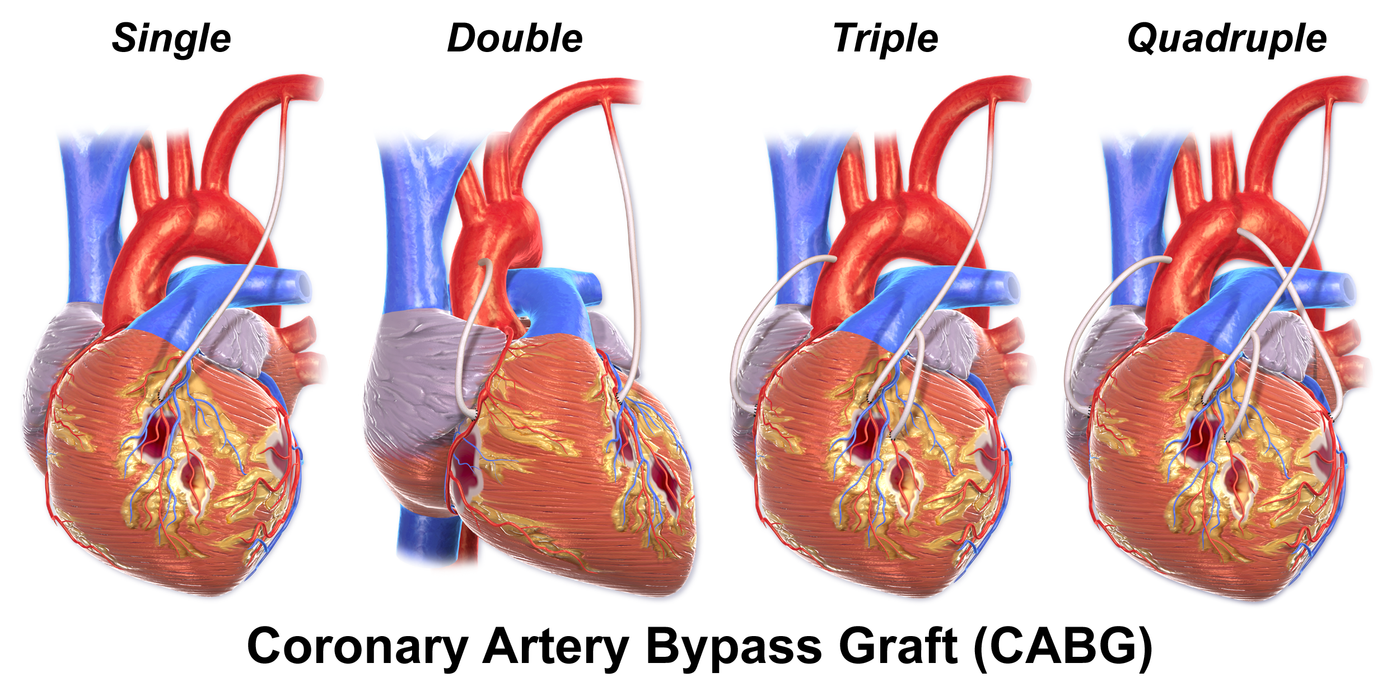
While doctors estimate that less than five percent of all American patients going under the knife for coronary artery bypass grafting (CABG) surgery receive multiple arterial grafts as opposed to multiple venous grafts, researchers in a new study published in
The Annals of Thoracic Surgery suggests that an artery-only approach will help CABG surgery patients live longer, especially when they also have diabetes.
A CABG surgical technique called total arterial revascularization (TAR) uses only arteries to redirect blood flow to the heart. CABG surgery is one of the most common major procedures performed in the U.S., with practically 400,000 completed annually. This procedure has been performed for more than half a century, and James Tatoulis, MD, FRACS from the Royal Melbourne Hospital in Australia confirms that "TAR/CABG is definitely within each cardiothoracic surgeon's ability and should be part of their repertoire.” CABG works by restoring normal blood flow by redirecting it around blood vessels with blockages due to plaque buildup.
Tatoulis and the rest of the research team from Australia studied the long-term outcomes of TAR/CABG surgery versus a conventional approach through thousands of cardiac surgical cases from the Australian and New Zealand Society of Cardiothoracic Surgeons Database. Out of more than 34,000 patients who received their first CABG surgery between 2001 and 2012, around 4,000 were diabetics. Half underwent conventional CABG, and half underwent TAR/CABG.
After comparing the end results from each of the two groups, Tatoulis and the other researchers saw a “significant magnitude of the difference” between the long-term survival of patients receiving TAR/CABG versus the conventional surgery, with the former surviving much longer than the latter.
Since more people are living and more people are living longer when their surgeons use arteries as opposed to veins as the blood vessel of choice for the bypass, Tatoulis believes “the superiority of TAR/CABG will assume progressive importance” in the near future.
“For every 100 diabetic patients undergoing CABG surgery, four more will be alive at ten years when arteries are used for the bypasses rather than just one arterial graft together with veins,” Tatoulis said.
Sources:
Elsevier,
Centers for Disease Control and Prevention,
American Heart Association