How Patients Surviving Advanced Heart Failure Defy the Odds
Ten years ago, a diagnosis of “advanced heart failure” was essentially a death sentence, aside from the patient miraculously receiving a heart transplant in time, which would have been highly unlikely with upwards of four thousand people in the United States on the waiting list on any given day.
However, a new procedure that has been developed and altered over the past decade has somewhat altered the dim outlook for heart failure patients. Implantation of a left ventricular assist device (LVAD) changed the way experts saw advanced heart failure. Only 15-20 percent of recipients reaped the benefits, but for this minority of advanced heart failure patients, an LVAD “unburdens the damaged heart and promotes recovery.”
Now scientists from the University of Utah are trying to figure out the difference between the 20 percent and the rest of the heart failure patient population. What makes those who respond unique? Unveiling the details behind these distinct differences of patients who have “defied the odds” could help doctors in identifying the best candidates for cardiac recovery therapies.
"Based on everything a doctor would traditionally measure, these patients look equally sick," said co-senior author Stavros Drakos, MD, PhD. "But what we're seeing is that there are differences between them at the biological level, and we can use that information to predict who has a chance to recover."
Drakos and his team examined heart biopsies taken at the time of LVAD implantation asking the question: For the patients who respond to treatment, what makes them equipped to do so?
"Most therapies are based on knowing what goes wrong in disease," Drakos said. "There's also a lot to be gained from understanding what goes right."
Ten heart biopsies were taken from LVAD patients who showed signs of recovery three months after the procedure, and 16 were taken from patients who did not recover. In comparison between the two types of biopsies, researchers quickly saw a difference in an anatomical structure in the heart called the transverse system (t-system).
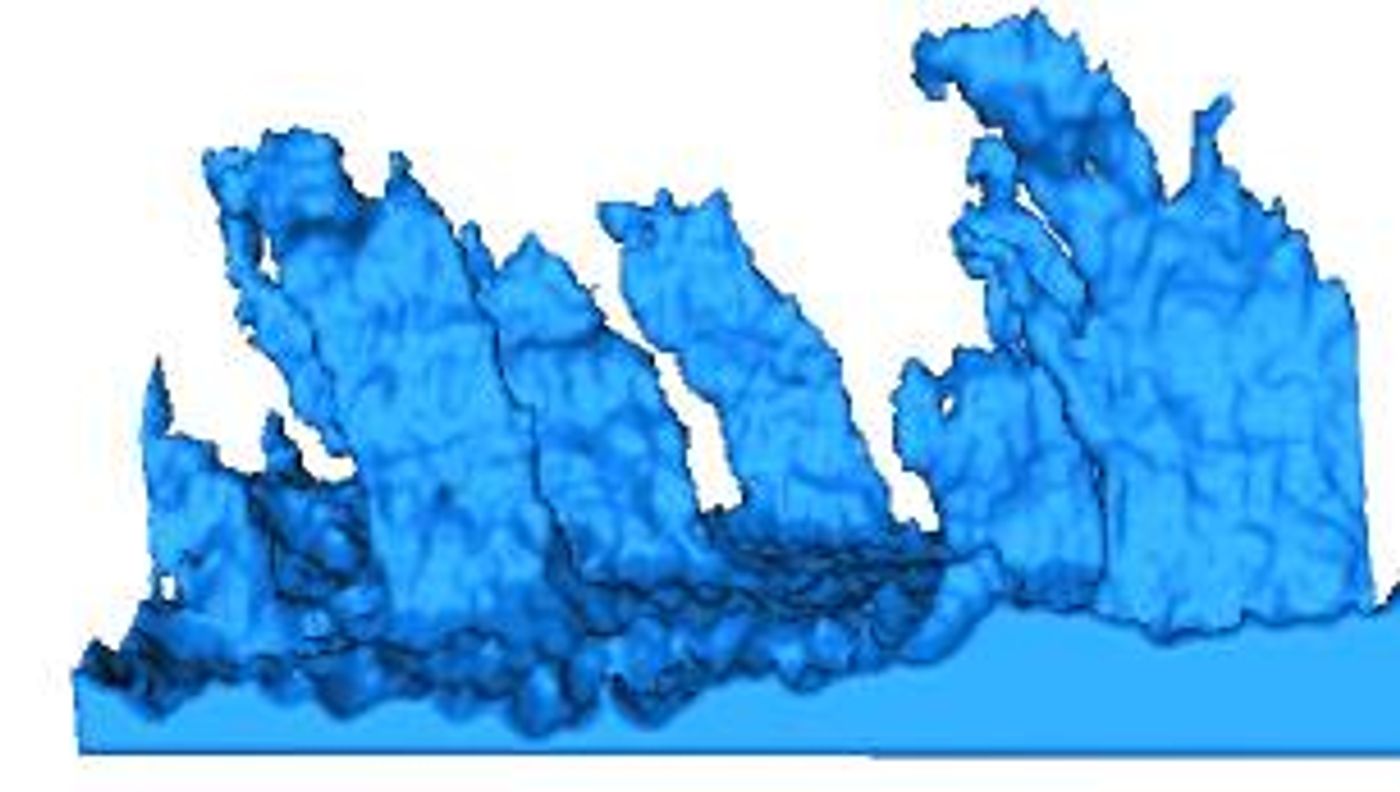
Image: Sheet-like remodeling of the transverse tubular system in human heart failure. Credit: Frank Sachse
In individuals who did not respond to treatment, the t-system, which normally extends thin, rounded fingers into heart fibers, instead “looked like squashed, flattened sheets.” This was an unexpected finding, one which scientists observed via advanced three-dimensional imaging. Co-senior author Frank Sachse, PhD, said he had never seen anything like it.
In contrast, the t-system in the ten patients who did respond to treatment was “relatively intact,” so much so that researchers began to make connections between an individual’s ability to recover based on the state of each transverse system.
"We're seeing that a patient's anatomy can help predict if that person has a high or low chance of recovery at the time of LVAD implantation," said first author Thomas Seidel, MD, PhD. "Our vision is that we can one day use this information to identify those patients that finally will not need a heart transplant, but may instead be weaned from the LVAD to go back to a normal life."
The present study was published in the journal Circulation.
Sources: University of Utah Health Sciences, Clinical Examinations in Cardiology, SynCardia Systems, LLC