Heart CT Scans for Personalized Blood Pressure Therapeutics
A decade-long study of nearly four thousand participants, conducted by scientists at Johns Hopkins University, provides a foundation for doctors with patients who are in the “gray zone” for blood pressure treatment.
"Our study, along with others, positions cardiac risk and coronary artery calcium as helpful ways to determine if a given patient would either benefit from more intensive blood pressure control or do just fine with a more traditional blood pressure target,” explainedJ. William McEvoy, M.B.B.Ch., M.H.S. from Johns Hopkins University School of Medicine.
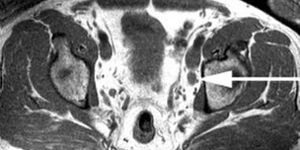
Cardiac CT scans used in this study can detect the amount of calcium in a patient’s coronary arteries. The higher the calcium levels in a patient’s arteries, the more they would likely benefit from aggressive blood pressure treatment. On the other hand, if a CT scan indicates a patient does not have high calcium in the coronary arteries, intense treatment is likely not necessary, and doctors can spare a patient from that experience.
Other heart disease risk factors must be considered as well, though. "If a health care provider wants to target blood pressure in a patient with traditional heart disease risk factors and above-normal blood pressure, he or she can look at coronary artery calcium to help with tiebreaker-like decisions," McEvoy explained.
McEvoy and his team enrolled 3,733 participants from the Multi-Ethnic Study of Atherosclerosis (MESA). Each individual had systolic blood pressure between 120 and 179mmHg. The male-female ratio was nearly 50:50, and the participants had an average age of 65 years.
At the beginning of the 10-year study, researchers measured blood pressure and participants underwent the cardiac CT scan to determine their coronary artery calcium scores. Once a year until the study was completed, researchers contacted each participant or a family member to take note of heart disease diagnoses, hospitalizations or deaths. At the end of the study, there were 642 total heart disease events among the 3,733 patients.
Upon analysis of the results, researchers calculated each participant’s heart disease risk via the “Atherosclerotic Cardiovascular Disease Risk Algorithm” which factors in components like race, age, sex, cholesterol, and family history. Participants were then divided into three groups based on the outcome of their coronary artery calcium from the CT scan. Researchers examined the number of heart disease-related events among the participants in each category.
They found that participants in the group with zero levels of coronary artery calcium but a high calculated risk of heart disease at the onset of the study actually had a low event rate after the ten-year study, while participants with a coronary artery calcium level greater than 100 and an initially low predicted rate of heart disease risk ended up with a high event rate. Participants with high systolic blood pressure had high event rates regardless of coronary artery calcium score
"It may be that if patients are in that blood pressure treatment gray zone with a high risk score but their coronary artery calcium score is zero, then they don't need to be treated aggressively to 120 millimeters of mercury and can be treated to 140 instead," McEvoy said. "But if patients have a high calcium score and are in the gray zone, then it would make sense to go with 120 as a treatment goal."
Almost one-third of the American adult population has prehypertension, and this study could help doctors and patients discern the most appropriate treatment pathway according to an individual’s specific needs and risk factors.
McEvoy’s study was recently published in the journal Circulation.
Source: Johns Hopkins Medicine