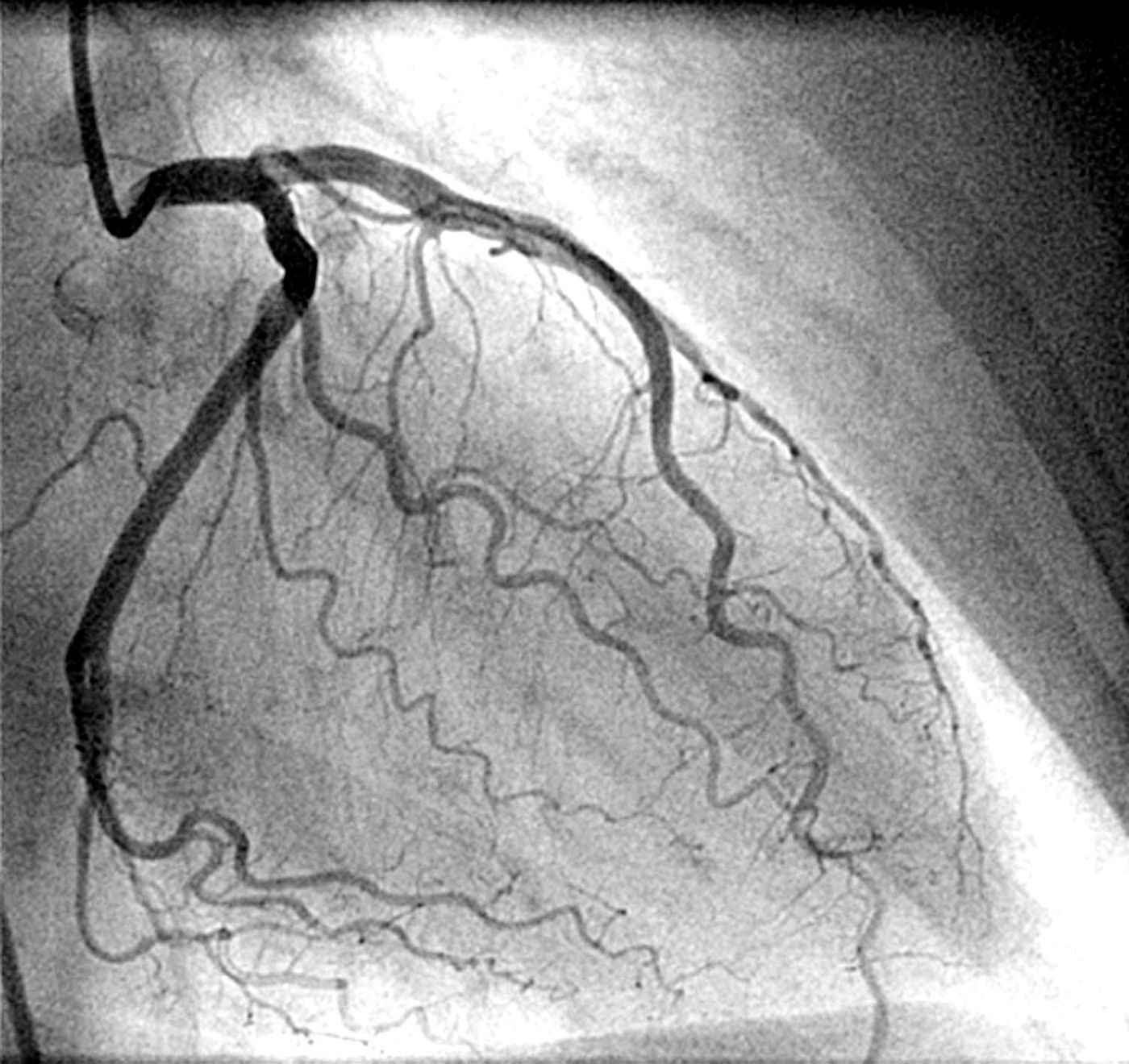
Predicting Heart Attacks with New, Noninvasive Imaging
Predicting a heart attack or other major adverse cardiac event (MACE) is possible with a pair of techniques that paint a picture for doctors by illustrating the status of a blockage in the blood vessels. These invasive procedures can cause side effects that may be unnecessary, though, according to new findings that suggest a noninvasive alternative is just as effective.
The key to determining whether a blockage is severe enough to warrant medical intervention to ward off MACEs is a factor called “hemodynamic significance.” This is a measure of how badly the blockage is preventing oxygenated blood from traversing the blood vessel to gain access to heart tissue in desperate need for oxygen.
If a blockage is declared hemodynamically significant, the next step is to treat the blockage with bypass surgery or stent placement, procedures which are both designed to improve blood flow to prevent MACEs like heart attack, stroke, and cardiac arrest.
But there is an problem that arises during the procedures completed to draw an accurate image of what the blockage looks like and what it is doing to inhibit blood flow: invasive coronary angiography (ICA), which demonstrates the nature of the blockage, and stress tests with single photon emission tomography (SPECT) myocardial imaging, which illustrate the amount of blood still able to cross the blockage into the tissue.
What is the issue with ICA and SPECT? First, ICA requires a catheter to be inserted into a blood vessel in the groin, which is then guided through the vessel up to the heart. The catheterization process can cause vascular problems, often at the site of initial injection. "In rare cases, it can cause strokes or heart attacks,” explained study author João A.C. Lima, M.D. “These risks are not trivial."
ICA and SPECT also end up costing the patient a lot of money due to longer, necessary hospital stays. The solution? A test that is noninvasive and combines ICA and SPECT, killing two birds with one stone.
After a comparison between the invasive and noninvasive combined approach to determining hemodynamic significance, the noninvasive approach proved to be just as successful at predicting MACEs as the traditional approach. Experts compared the two approaches in a study of nearly 400 patients referred for ICA.
"The key finding of our study is that both techniques are equally effective in identifying which patients are going to have trouble down the road," Lima said. "The noninvasive option should be a preferred or at least strongly considered option by cardiologists and radiologists managing these patients because it is safer and less expensive, and patients like it better."
Lima’s study was recently published in the journal Radiology.