Regenerative Heart Muscle Cell Boosts Healing
Some organisms have strong regenerative abilities, but humans are not among them. However, recent exploration of a regenerative cell type may offer a new solution, according to scientists from the University of Southern California.
Mononuclear diploid cardiomyocytes (MNDCMs) are known for their regenerative abilities in the heart muscle but are only present in zebrafish, a common model organism, and newborn mice, humans, and other mammals. There are only low levels of MNDCMs in adult mammals, limiting the cells’ regenerative abilities. However, a recent study in mice suggested that there might be something that could be done to increase levels of MNDCM.
USC researchers saw “a surprising amount of variation” in MNDCM levels among different strains of mice during their studies. Of all heart muscle cells, some strains of mice showed ten percent of MNDCMs. The same mice were better able to recover after damage was done to the heart. Could there be similar variation in humans?
"[This finding] suggests that not all individuals are destined to permanent heart muscle loss after a heart attack, but rather some can naturally recover both heart muscle mass and function,” explained first author Michaela Patterson, PhD. “If we can identify the genes that make some individuals better at it than others, then perhaps we can stimulate regeneration across the board."
Patterson and the rest of the research team did just that, during a genome-wide association study (GWAS). They identified a gene called Tnni3k (cardiac troponin I-interacting kinase) to be involved in the variation they observed in the mice study. Inhibiting Tnni3k activity boosted the level of MNDCMs and, subsequently, the ability of the mice to regenerate heart cells. Enhancing Tnni3k activity had the opposite effect.
Tnni3k was also described in a 2013 study as interacting with a protein called cardiac troponin I to impact contraction of cardiac myofilaments, which play a role in the heart’s pumping of oxygenated blood to tissues all over the body.
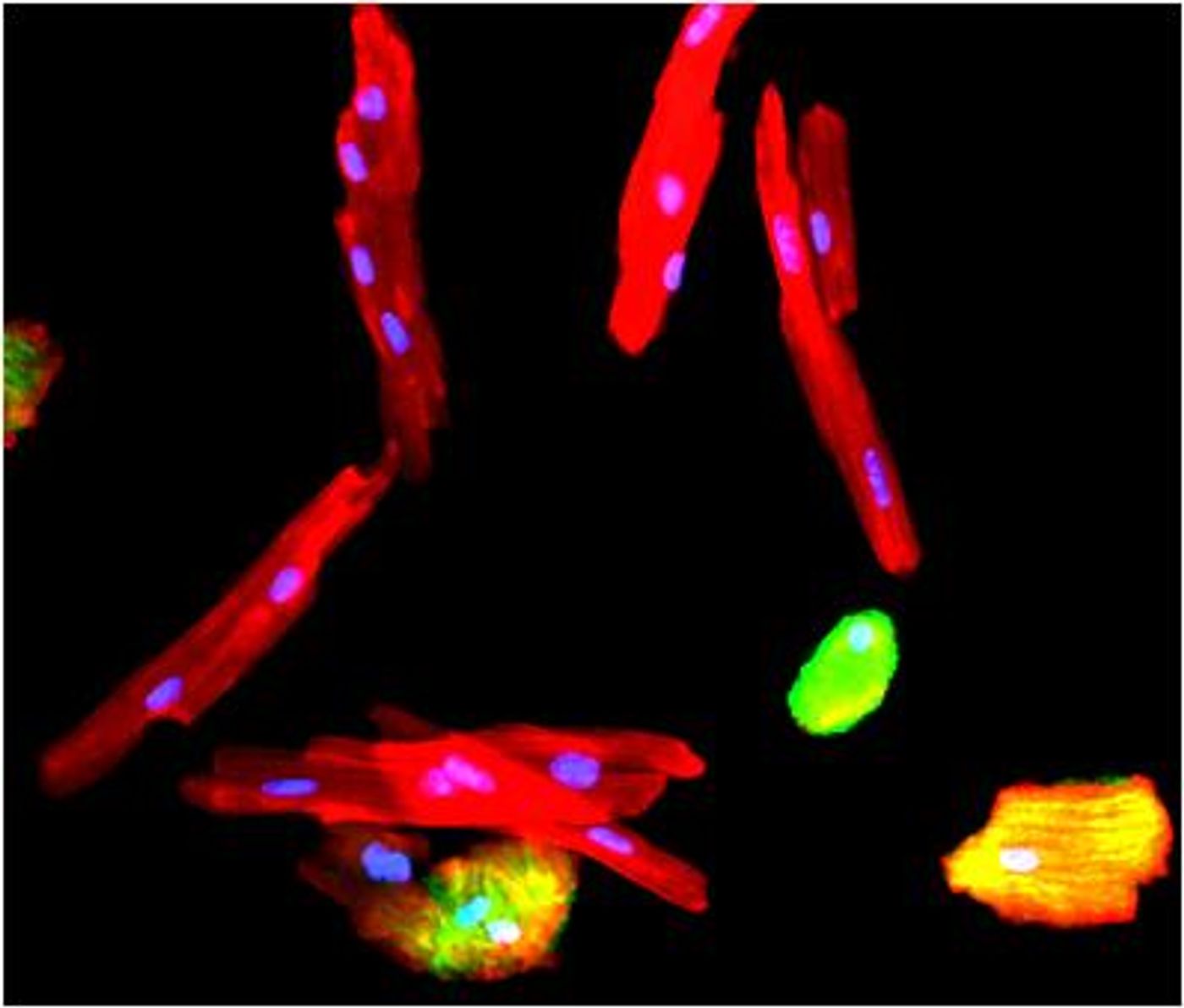
Heart muscle cells (red) with nuclei (blue). On the far right is a regenerative cell, which only has one nucleus. Credit: Michaela Patterson/USC
"The activity of this gene, Tnni3k, can be modulated by small molecules, which could be developed into prescription drugs in the future," explained senior author Henry Sucov, PhD. "These small molecules could change the composition of the heart over time to contain more of these regenerative cells.” More regenerative cells, less initial damage done to the heart for people on the verge of heart failure.
The present study was published in the journal Nature Genetics.
Sources: Journal of Biomechanics, Brazilian Journal of Medical and Biological Research, University of Southern California - Health Sciences