Brain Activity Predicts Who Will and Who Won't Survive Cardiac Arrest
Mapping and measuring the interaction between very specific parts of the brain while a cardiac arrest survivor is comatose could help scientists predict which patients will survive, which won’t, and which will live the rest of their lives with debilitating neurological problems.
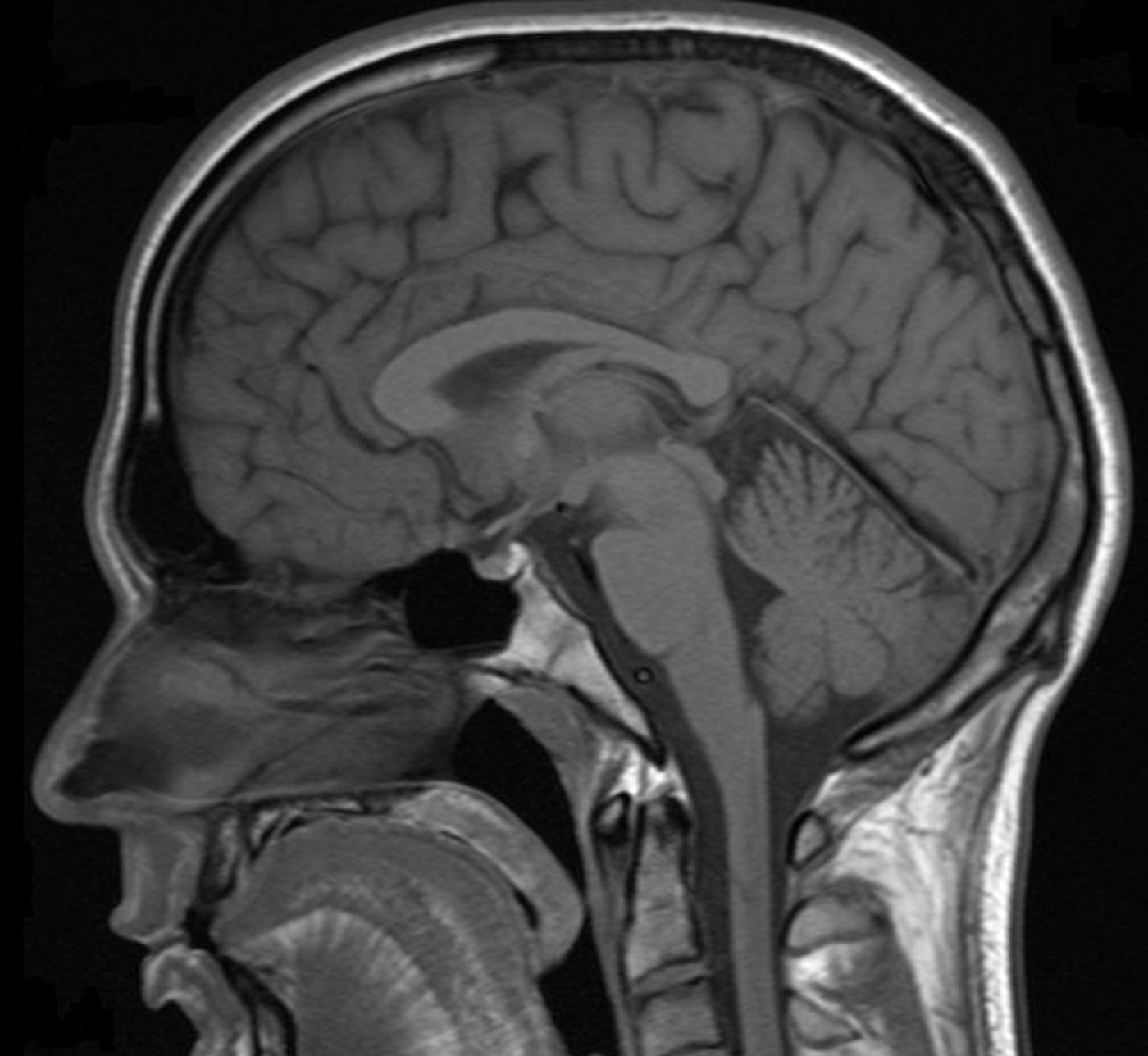
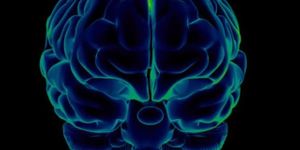
From Johns Hopkins University, scientists used the quantitative brain mapping capabilities of functional MRIs to measure and record changes in tissue structure, blood flow, and functional activation with remarkable precision and accuracy.
With this data, says senior author Robert Stevens, MD, researchers could “see where brain network disruption is occurring, and determine how these changes relate to the likelihood of recovery from brain damage.”
The present study focused on patients recovering following a cardiac arrest, but the new brain mapping protocol could also predict reliable “long-term recovery trajectories” for people recovering from heart attack, stroke, brain hemorrhage, or trauma.
Unlike a heart attack, where a disruption in blood flow blocks oxygenated blood from reaching the heart, cardiac arrest is a sudden loss of a heartbeat that can lead to death in minutes.
Stevens notes several factors that influence the chance of survival and the amount of brain damage a person will incur, including how quickly and how well a person in cardiac arrest receives resuscitation and how well body temperature is regulated to avoid fever. Existing technologies to predict recovery following cardiac arrest are few and far between.
Stevens and others conducted their study with 46 patients in a coma following cardiac arrest, all with an average age of 49. Between one and two weeks after each patient’s cardiac arrest, researchers assessed their brain’s functional activation. They focused on four networks in the brain involved in using energy to focus attention, being at rest, initiating tasks, rewards and inhibition, and determining the importance of stimuli.
Researchers continued with a follow-up one year after the cardiac arrests to assess overall survival. Compared to the others, eleven of the original 46 had favorable outcomes, with little to no neurological disability and higher connectivity with the brain region associated with being at rest as well as so-called anti-correlation between other networks, which means that while one is active the other is not.
"These findings highlight a potential realm of precision medicine using brain network biomarkers that are discriminative and predictive of outcomes," explained lead author Haris Sair, MD. "In the future, connectivity biomarkers may help guide new therapies for targeted treatment to improve brain function."
The present study was published in the journal Radiology.
Source: Johns Hopkins Medicine