What's the secret to clear arteries in old age?
UNC Chapel Hill lead researcher Jonathan Schisler, PhD, lost both of his grandfathers to heart disease, and now he is dedicated to studying the condition as well as to identifying new treatments and prevention methods. In his newest study, he and other researchers identify a potential genetic basis for coronary artery disease (CAD), the leading cause of heart attacks and death in the United States.
Plaque buildup occurs naturally with aging, but some people appear to be better than others at keeping their arteries clear as they get older. The new UNC study, published in the American Journal of Pathology, identifies the CXCL5 protein, and genetic variants near the CXCL5 gene, as potential markers of healthy coronary arteries.
The CXCL5 protein is part of the CXC family of chemokines, signaling proteins released by cells to send messages. CXCL5 is found in the blood, produced and released by platelets. In 2010, CXCL5 was paradoxically found to both hinder host defense in the lungs in response to an E. coli infection and recruit neutrophils during inflammation.
In the present study, where Schisler and other researchers analyzed more than 143 patients’ blood samples and heart scans, CXCL5 proved to be higher in quantity in older adults (more than 65 years of age) who had relatively clear coronary arteries.
“The more CXCL5 you have, the healthier your coronary arteries are,” Schisler explained. How does CXCL5 improve the health of the arteries? Research shows that it can minimize plaque buildup by “changing the composition of fat and cholesterol deposits in the arteries.”
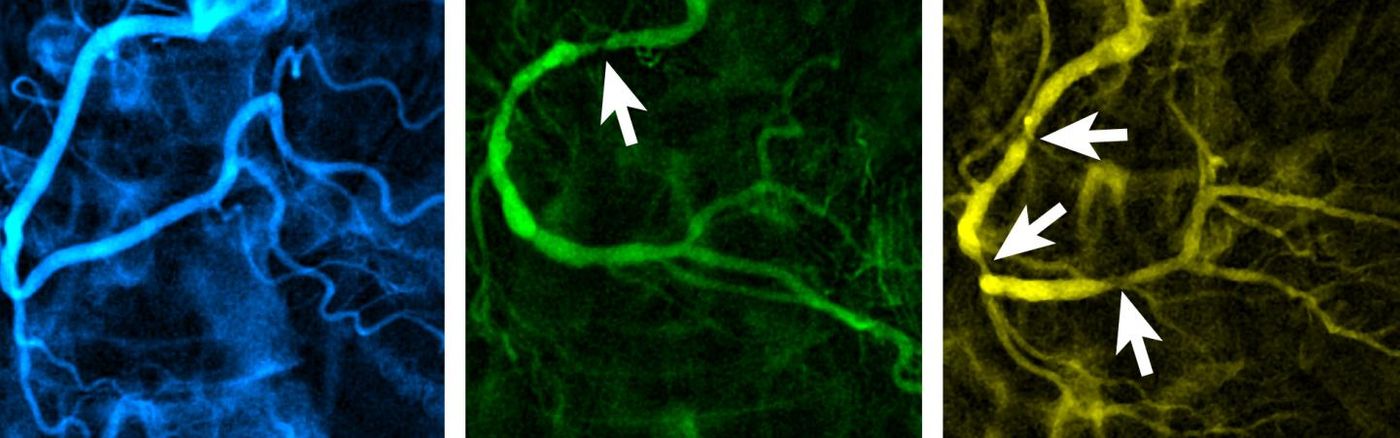
"Patients with no obstructed blood flow in the coronary arteries had higher levels of CXCL5 (blue) compared to patients with moderate levels (green) or lower levels (yellow) of CXCL5, who had increased severity of coronary obstructions (indicated by the arrows)." Credit: Schisler lab, UNC School of Medicine
The results suggestive that CXCL5 was both protective against CAD and a possible therapeutic ingredient to treat CAD. In patients with dwindling levels of CXCL5, researchers more often saw “increased severity of coronary obstructions.” However, Schisler stresses the importance of conducting more studies to confirm their findings, particularly studies that also includes test results from healthy patients for comparison.
Going forward, Schisler and his team are considering the wide variety of applications that are possible now knowing what they know about CXCL5. They could develop drugs that reduce plaque buildup by imitating the actions of CXCL5. They could stimulate the body directly and increase its natural production of the protein. Or, they could use CXCL5 as a biomarker for CAD to improve diagnostics.
"Although our goal was not to discover biomarkers that may have diagnostic or prognostic applications, it's possible and worth exploring,” Schisler said. Needless to say, the possibilities of applying CXCL5 to reducing the burden of CAD are near endless and definitely needed.
Sources: Immunity, Critical Reviews in Oral Biology and Medicine, University of North Carolina Health Care