First-of-its-Kind Optical Ultrasound Imaging to Transform Heart Surgery
For the first time, scientists have applied all-optical ultrasound imaging in a “clinically realistic environment,” using a new technology from the University College London and Queen Mary University of London: the optical ultrasound needle. The new technology is expected to revolutionize the way surgeons approach heart and other high-risk surgical procedures.
The new optical ultrasound technology was customized to fit into a needle for use in keyhole procedures. Current technology for these procedures consists of external ultrasound probes that provide images of soft tissues and organs before the procedure.
A “keyhole procedure,” also known as laparoscopic surgery or minimally invasive surgery, is characterized by a procedure using a video camera and multiple small instruments. The surgeon makes small incisions through which to guide the camera and instruments to complete the procedure. Without needing large incisions to physically see inside the body, the camera shows the surgeons what they need to see, boosting recovery times and reducing post-procedure discomfort.
"The optical ultrasound needle is perfect for procedures where there is a small tissue target that is hard to see during keyhole surgery using current methods,” explained co-lead author Dr. Malcolm Finlay. “Missing it could have disastrous consequences.”
Applying the new technology provides several advantages for surgeons and patients:
-
Real-time imaging
-
Able to differentiate between tissues at a remarkable depth
-
Guide high risk moments during surgery
-
Reduce the risk of complications
“The technology has been designed to be completely compatible with MRI and other current methods, so it could also be used during brain or fetal surgery, or with guiding epidural needles,” Finlay added.
Finlay and colleagues took for years to fine-tune the new technology for use in a clinical setting, and they have successfully applied it to a minimally invasive heart surgery in pigs.
“We now hope to replicate this success across a number of other clinical applications where minimally invasive surgical techniques are being used," explained co-lead author Dr. Adrien Desjardins.
How it works
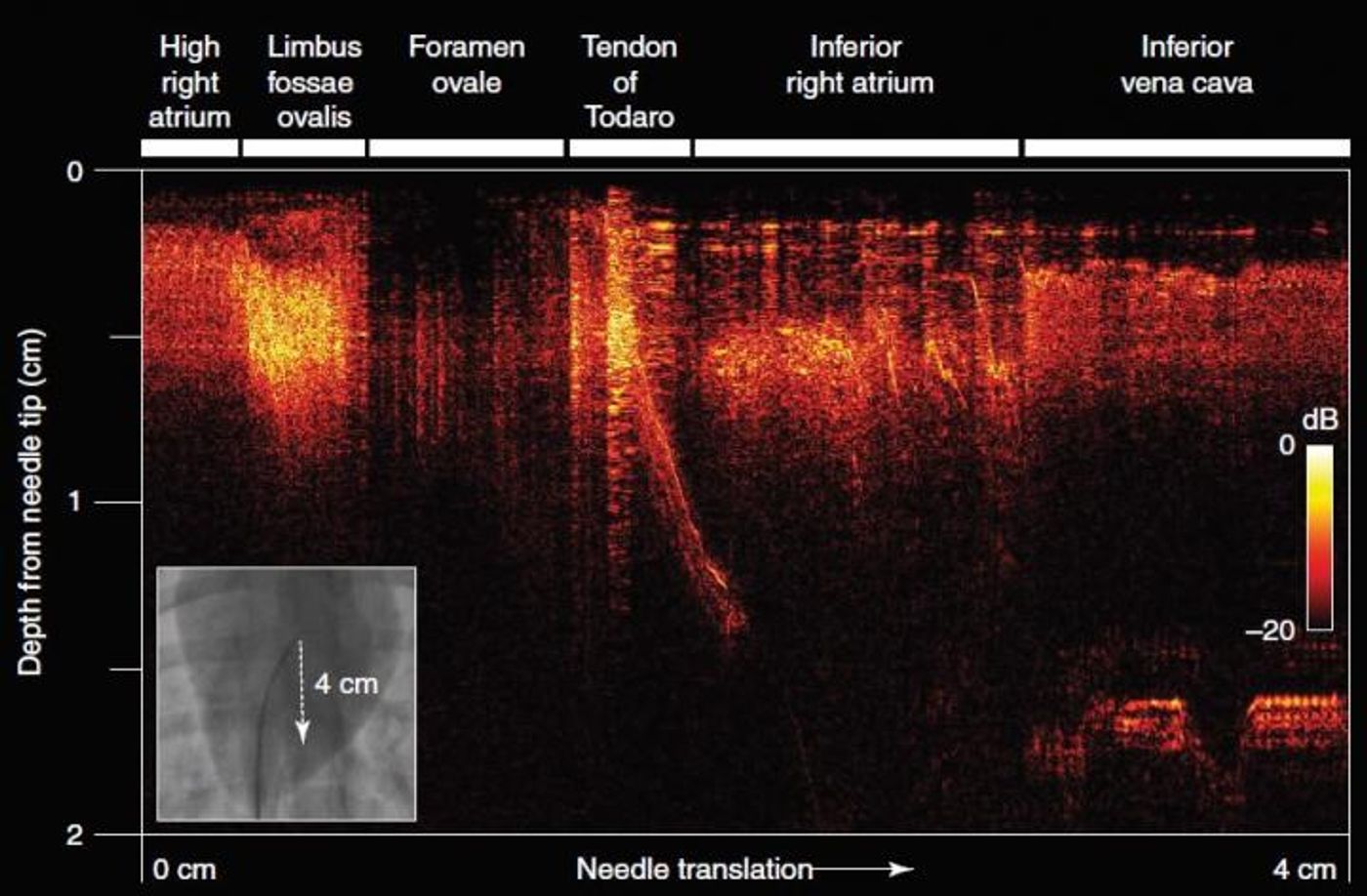
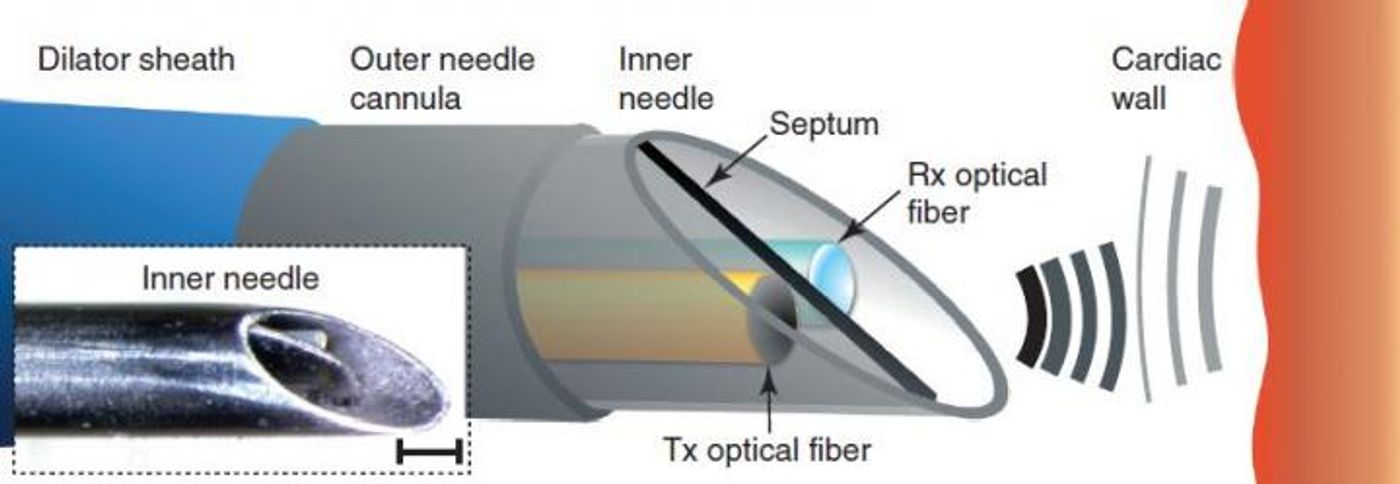
Sheathed within a customized clinical needle, small optical fibers are used to generate a pulse of light followed by ultrasonic pulses. “Reflections” from these pulses provide real-time ultrasound imaging to guide the surgeon’s hand during a procedure, based on ultra-sensitive detection from a second optical fiber.
"The whole process happens extremely quickly, giving an unprecedented real-time view of soft tissue,” explained co-author Dr. Richard Colchester. “It provides doctors with a live image with a resolution of 64 microns, which is the equivalent of only nine red blood cells, and its fantastic sensitivity allows us to readily differentiate soft tissues.”
The present study was published in the journal Light: Science and Applications.
Sources: University of Southern California Department of Surgery, University College London