Early Detection of Low Blood Sugar Made Possible with Heart Rate Monitor
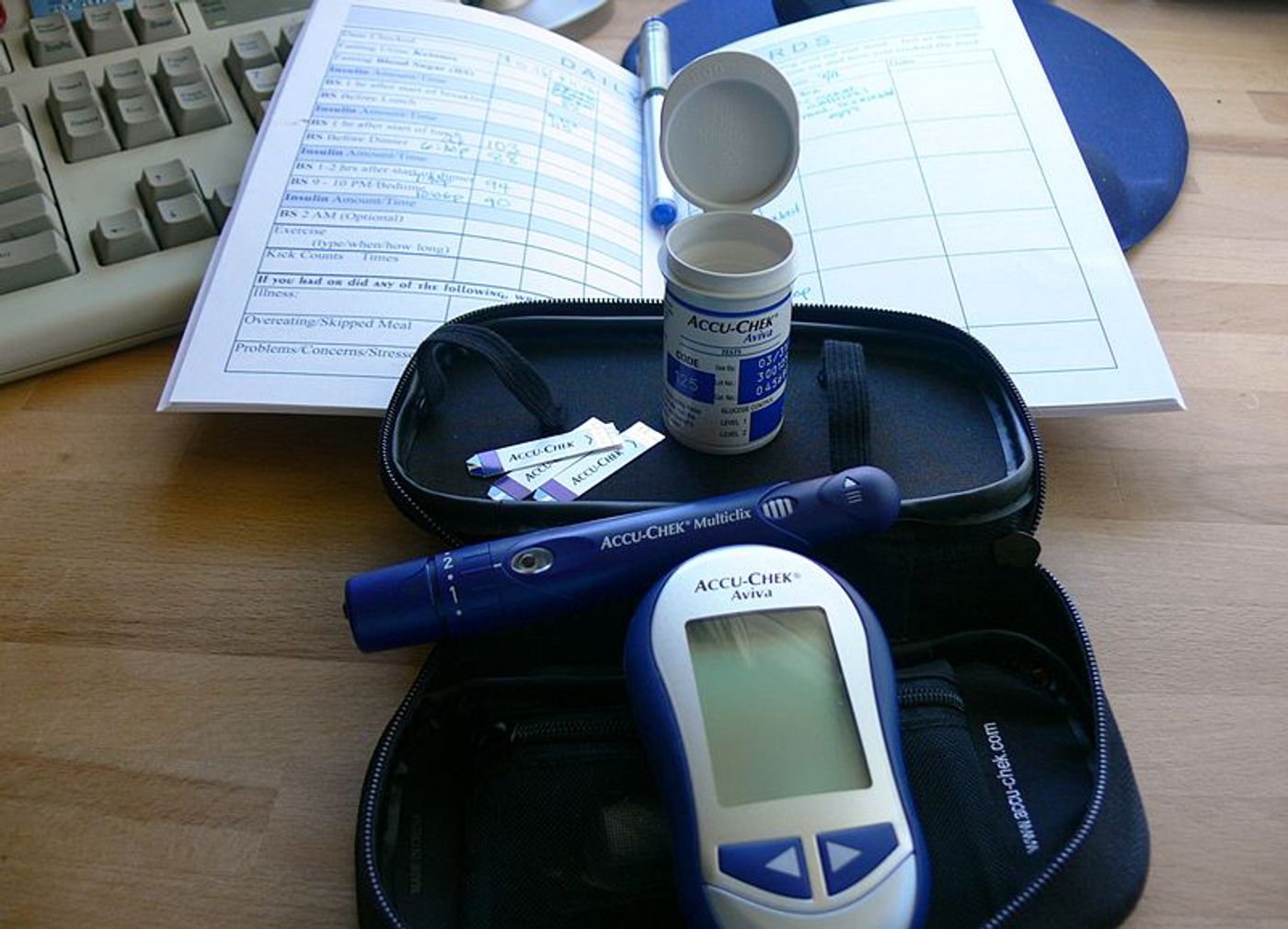
For people with type 1 diabetes, being unaware of a hypoglycemic (low blood sugar) event could be very dangerous. To help people detect these type of events, researchers have adopted a commercially-available heart rate biosensor.
Type 1 diabetes is an autoimmune disease where the immune system mistakenly attacks the insulin-producing cells of the pancreas, called beta cells. People with this condition have to self-administer injections of insulin to make up for this loss. Hypoglycemia can lead to seizures, loss of consciousness, and death. And many people with type 1 diabetes do not experience the same warning signs as other people. This impaired awareness of hypoglycemia prevents people from recognizing the state of their blood sugar and can lead to dangerous events.
Some people with impaired hypoglycemia awareness use glucose sensors, but these devices often produce delayed results, skewing the accuracy of glucose measurements. Because of this, scientists found reason for an additional monitor technology.
At the beginning of a hypoglycemic event, the sympathetic nervous system, also known as the “fight or flight response” is activated, which results in increased heart rate, blood pressure, breathing rate, and pupil size. On the other hand, the parasympathetic nervous system, which mostly performs the opposite actions, is suppressed. The new device works on an algorithm designed to detect “beat-to-beat variation” in heartbeats that occurs during hypoglycemia.
Researchers used a commercially-available heart rate and single-lead electrocardiogram (ECG) biosensor, the HealthPatch made by VitalConnect. They tested this biosensor in 27 men and women with type 1 diabetes and self-reported issues with impaired hypoglycemia awareness.
During the study, each participant wore the HealthPatch on their chest along with a continuous glucose meter. They also recorded low blood sugar levels verified by traditional fingerstick measurements. The data collected by the sensor was wirelessly transmitted to a mobile device, where the researchers’ algorithm went to work.
Using the data, researchers evaluated 39 hypoglycemic events and compared them to the results from glucose meters and fingerstick measurements. The algorithm successfully detected hypoglycemic heart rate variability at the start of hypoglycemia in 72 percent of cases. Going forward, researchers plan to improve the accuracy and precision of the algorithm to account for the hypoglycemic events it did not detect. Ideally, the technology would also be able to “translate the data into an audiovisual hypoglycemia alert “that can be sent to a mobile device
"Timely detection of impending hypoglycemia is critical to avoid severe, potentially life-threatening hypoglycemia," explained principal investigator, Marleen Olde Bekkink, MD, PhD. "Our proof-of-principle study found that measuring heart rate variability using a wearable device in an outpatient setting seems promising for alerting to upcoming hypoglycemia."
Sources: American Diabetes Association, PubMed Health, The Endocrine Society