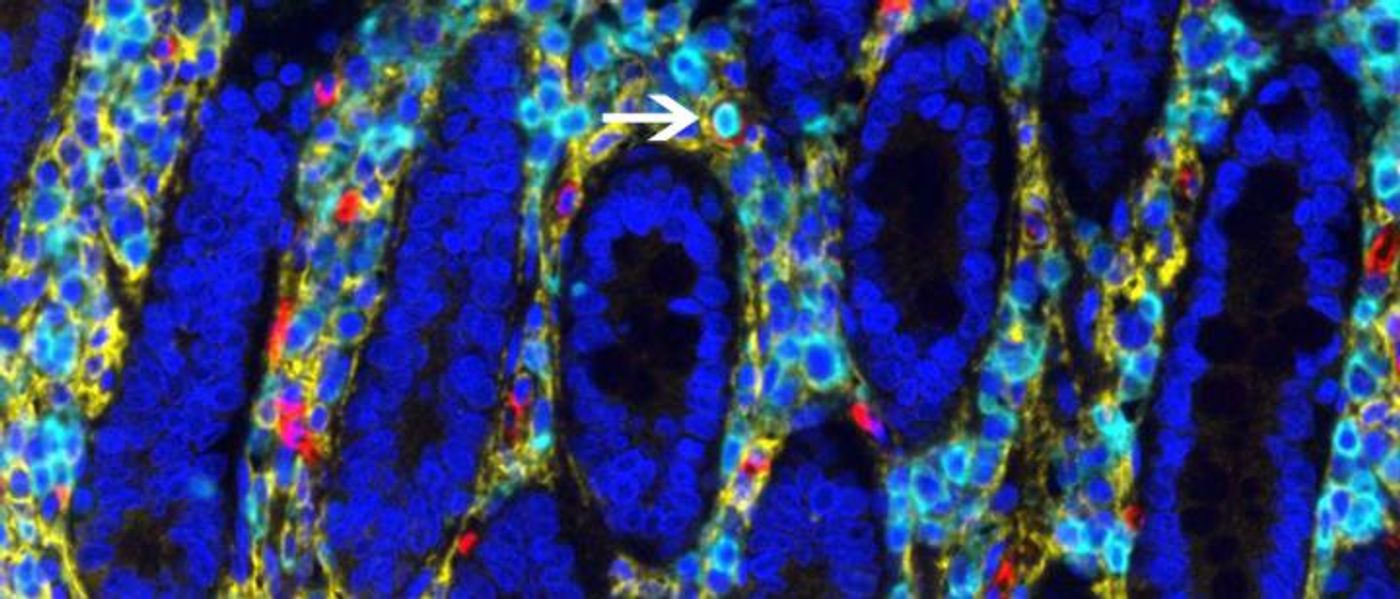
Researchers Surprised to Find a Reservoir of Blood Stem Cells in the Gut
There are a few major types of blood or hematopoietic cells, including red blood cells, which transport oxygen, and white blood cells, which are critical to the immune system. It had been thought that bone marrow was the only source of the many new blood cells that our body has to generate, where important hematopoietic stem cells reside. But new work by scientists at Columbia University Vagelos College of Physicians and Surgeons has found another reservoir of those stem cells: the intestine.
It seems that the human intestine might be providing up to ten percent of circulating blood cells, in a surprise to the researchers. They discovered this intestinal reservoir when researchers found donor blood cells in the blood of intestinal transplant recipients. Researchers led by Megan Sykes, MD, director of the Columbia Center for Translational Immunology, looked for the source of those donor blood cells and found hematopoietic stem cells in the donated intestine.
Intestinal transplants can be extremely critical to patients with intestinal disorders like Crohn’s disease; their intestinal function may fail and transplant becomes the only option. There are, however, high rates of rejection and serious complications from immunosuppressant drugs, and intestinal transplant success is limited.
Scientists have found that after an intestinal transplant, white blood cells in the recipient are mature, and can tolerate the tissues of the recipient. It may be possible to get them to tolerate donor tissues too.
"We are clearly showing that there's immunological cross-talk between the two sets of blood cells that protect the transplant from the patient's immune system and protects the patient from the transplant," said Sykes.
The investigators found that eventually, intestinal hematopoietic stem cells are replaced by a recipient pool. Blood cells made by the donated intestine may also be helpful to the recipient in the interim; patients with more donor blood cells displayed lower rates of organ rejection. This work might open new avenues for improving transplant success.
"It's possible that patients with a high level of donor cells may not require as much immunosuppression as they are currently getting," said Sykes, "and reducing immunosuppression could improve outcomes."
There might be an increase in transplant tolerance if extra donor hematopoietic stem cells are added to transplant organs.
"That could improve the lives of transplant patients dramatically," Sykes said. "Our ultimate goal is to get immune tolerance, which would allow us to remove immunosuppression altogether and have the graft treated as self by the patient. That's really the Holy Grail."
Much more work remains before this work will translate to the clinic, but the researchers are continuing their efforts. They are going to try to increase the amount of hematopoietic stem cells that are transmitted during transplant, which will hopefully raise the levels of circulating donor blood cells, benefiting immune tolerance.
The video above describes the first intestinal transplant performed in Michigan, at Henry Ford Hospital in Detroit, about six years ago.
Sources: AAAS/Eurekalert! via Columbia University Irving Medical Center, Cell Stem Cell