Cooling Injured Brain Cells Can Aid Recovery
According to the Centers for Disease Control and Prevention, in 2014 there were around 2.87 million incidences of traumatic brain injury-related emergency room visits, caused in part by car accidents, sports injuries, assaults, and falls. There is no approved treatment for these injuries, which can have serious long-term consequences and may reduce the lifespan of some people. Scientists have been studying how hypothermia or cooling might help treat these injuries. Researchers at the University of Wisconsin (UW)-Madison have looked at the impacts of this treatment at the cellular level, and their findings have been reported in PLOS ONE.
"There are currently no effective medical treatments for concussions and other types of traumatic brain injuries. We're very excited about our findings because they could potentially pave the way for treatments we can offer patients," said the study leader Christian Franck, the UW-Madison associate professor of mechanical engineering.
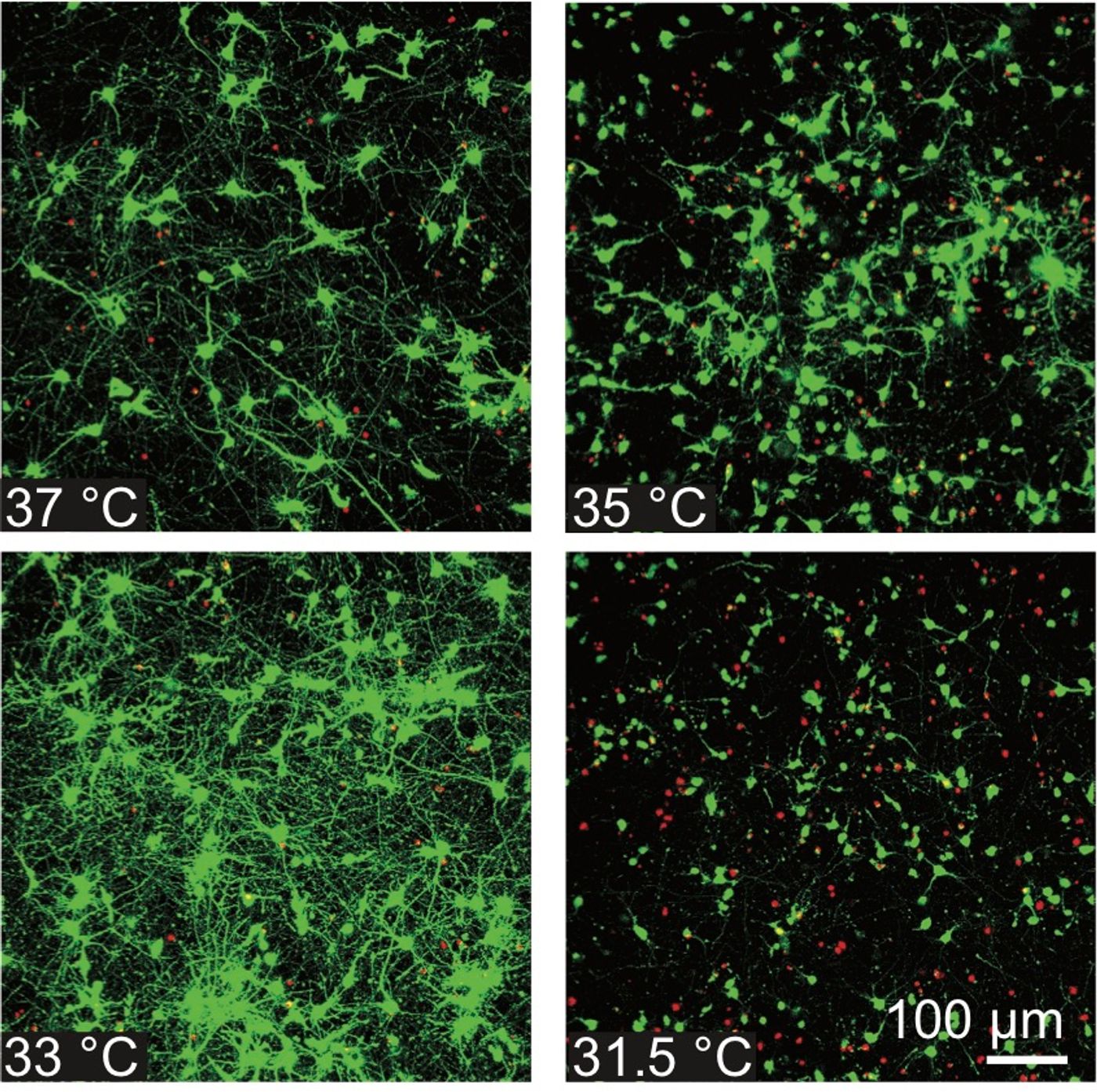
In this work, the researchers grew neurons in culture and exposed them to a mechanical stimulus that was meant to mimic the cell damage that would result from a concussion. They then cooled the cells to one of four temperatures. They determined that the treatment had to be fine-tuned. "We found that, for this treatment to be successful, there's a sweet spot," said Franck. "You can't cool too little; you can't cool too much, and you can't wait too long following an injury to start treatment."
After finding the right levels, there was an impressive effect. "I was amazed at how well the cooling worked," Franck said. "We actually went back and repeated the experiments multiple times because I didn't believe it at first."
The biggest benefit was seen at 33 degrees Celsius, when applied 24 and 48 hours after the injury. When cells were cooled to 31 degrees Celsius, however, there was a detrimental impact. The treatment also had to be delivered within four hours of the injury, and had to last for at least six hours to have the best outcome. Even 30 minutes of cooling was beneficial though, noted Franck.
If the researchers stayed within the parameters they set for the best outcome, they were able to keep the cells functioning normally even though they'd been injured; the damaging pathways that come on after an injury to the cell were kept off. These deleterious pathways can lead to neurodegeneration and in patients, negative health effects. "These pathways are like flipping on a bad molecular switch in your brain," explained Franck.
But after the cooling, the pathways stayed off even if the cells were brought back to a normal temperature.
"The biggest surprise was that the molecular switches actually stayed off -- permanently -- through the duration of the lab experiment," Franck said. "That was huge."
There will be more to learn before this becomes a commonly applied treatment in the clinic. Lowering the temperature of the entire body can have negative consequences, so the cooling must also be limited to the brain.
"We hope our paper will spawn renewed motivation and interest in solving the technical challenges for getting this type of treatment to patients in the future," Franck said. "For a long time, the scientific literature was inconclusive on whether this would be a successful treatment. What we showed in our study was that, yes, as far as the cell biology is concerned, this is effective. And so now it's really worth thinking about how we might implement this in practice."
Sources: AAAS/Eurekalert! via University of Wisconsin-Madison, PLOS ONE