Smell Cells Are Especially Good at Fighting the Flu
All over the body, epithelial cells line organs and vessels, forming protective barriers. But some pathogens like the influenza virus have gained the ability to infect epithelial cells. Researchers investigating influenza have studied epithelial cells that line the lungs, because the flu infects those and uses them to generate more copies of the virus. These viral particles cause the cell to burst, releasing the new viral particles so they go on to infect more cells. However, the virus also passes by cells in the upper respiratory tract on their way to the lungs, exposing them probably to the same levels of influenza as lung epithelial cells. However, the cells in these upper airways are far less likely to die from being infected by the flu. Now researchers know more about why; the findings have been published in Cell Reports.
"So you're standing on the bus, somebody sneezes, and you breathe something in," said Nicholas Heaton, an assistant professor of molecular genetics and microbiology in the Duke School of Medicine. "But where does that virus go? It's certainly not somehow sneaking all the way down to the bottom of your lungs before it encounters a cell. It's hitting somewhere in your nose."
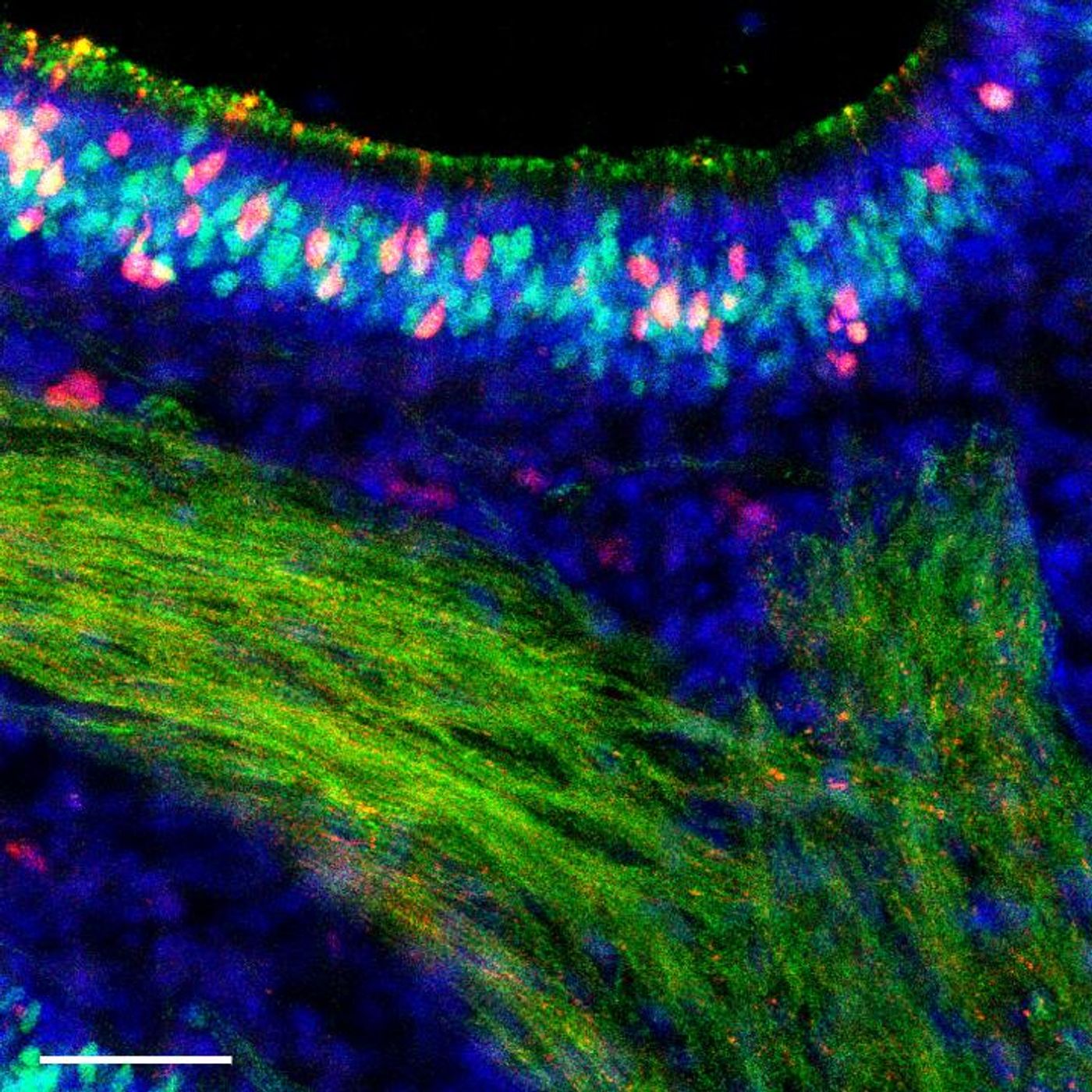
Researchers led by Heaton and Ashley Moseman of Duke immunology have now shown that the cells that line the nose and detect smells, called olfactory sensory neurons, are able to mount a very strong immune defense. The work shows that the immune response can be varied among different cells, noted Heaton.
"There's this whole group of cells that get infected but do something different," he said. "So we felt like we should be studying those cells."
These front-line cells also have a direct connection to the central nervous system, including the brain, so it’s especially important for the body to prevent flu infections from getting a foothold there. Some flu strains are known to affect the brain.
In this work, Heaton’s team looked at how cells in the sinuses and upper respiratory tract responded to exposure to the virus. They saw that while olfactory cells became infected, they fought off the pathogen before being killed by it.
When they sequenced the RNA in the cells to look at the active genes, they saw that the olfactory cells activated a group of genes that are known to help fight off invaders, but the cells turned them on more (either higher or faster, the team does not know which yet), compared to other cells.
Learn more about the sense of smell, or olfaction, from the videos.
"They upregulate genes that shut down viral replication," explained study author Rebekah Dumm, Ph.D. This is the same group of antiviral genes activated by the epithelial cells, "but the higher level to which they are induced was striking," Dumm said. "It's surprising because most of these genes were discovered and best described in the respiratory cells."
"Olfactory neurons have the ability to fight this virus off a little better than other cells," Heaton said. "We think that might be a brain-protective mechanism." Heaton added that there may be a straightforward explanation for why all cells don’t respond like the olfactory cells. It may be, for example, that a strong immune response would be a bad thing in lung cells.
Heaton’s team is going to continue to investigate the differences among cells’ immune responses. "You're a person who's been exposed to all kinds of stuff, you have your own particular exposure history that gives you different antibodies, different cell memory phenotypes, probably also different epithelial phenotypes, and we'd like to know what that means in terms of how you respond to secondary infections or these types of things."
Sources: AAAS/Eurekalert! via Duke University, Cell Reports