An Autoimmune Link to Heart Disease is ID'ed
It’s vital for our immune system to protect us from pathogenic invaders, and immune cells must constantly be on the lookout. But the immune system also has to be careful and extensively regulated so that it does not start to attack cells of the self. Auto-immune diseases can be devastating. Type 1 diabetes, for examples, can occur when the immune system destroys insulin-producing cells in the pancreas. Researchers have now identified an autoimmune component of cardiovascular disease, the world’s leading cause of death.
Cardiovascular disease tends to be fatal when a heart attack or stroke occurs. Blood clots caused by artherosclerosis often trigger these events. Artherosclerosis is a chronic disease in which cell debris, fats and other materials generate plaques in the walls of blood vessels, causing inflammation. Thrombosis is when a blood clot happens inside of a blood vessel.
Reporting in Nature, scientists have now identified a molecule that can act as an autoantigen and play a role in artherosclerosis development.
"We know that atherosclerosis includes an immunological component and that the innate and adaptive immune systems are both involved in the origin and progression of this disease,” said study leader Dr. Almudena Ramiro of the CNIC.
The researchers found that a molecule called ALDH4A1, a mitochondrial protein, is involved in artherosclerosis, and triggers an immune response.
"ALDH4A1 is recognized by the protective antibodies produced during atherosclerosis, making it a possible therapeutic target or diagnostic marker for this disease," Ramiro said.
In this study, the researchers used a mouse model that lacks a receptor for low-density lipoprotein (LDL), which transports so-called ‘bad’ cholesterol, and gave them a diet high in fats. The scientists assessed the antibody response in these animals to see if autoantibodies were being generated.
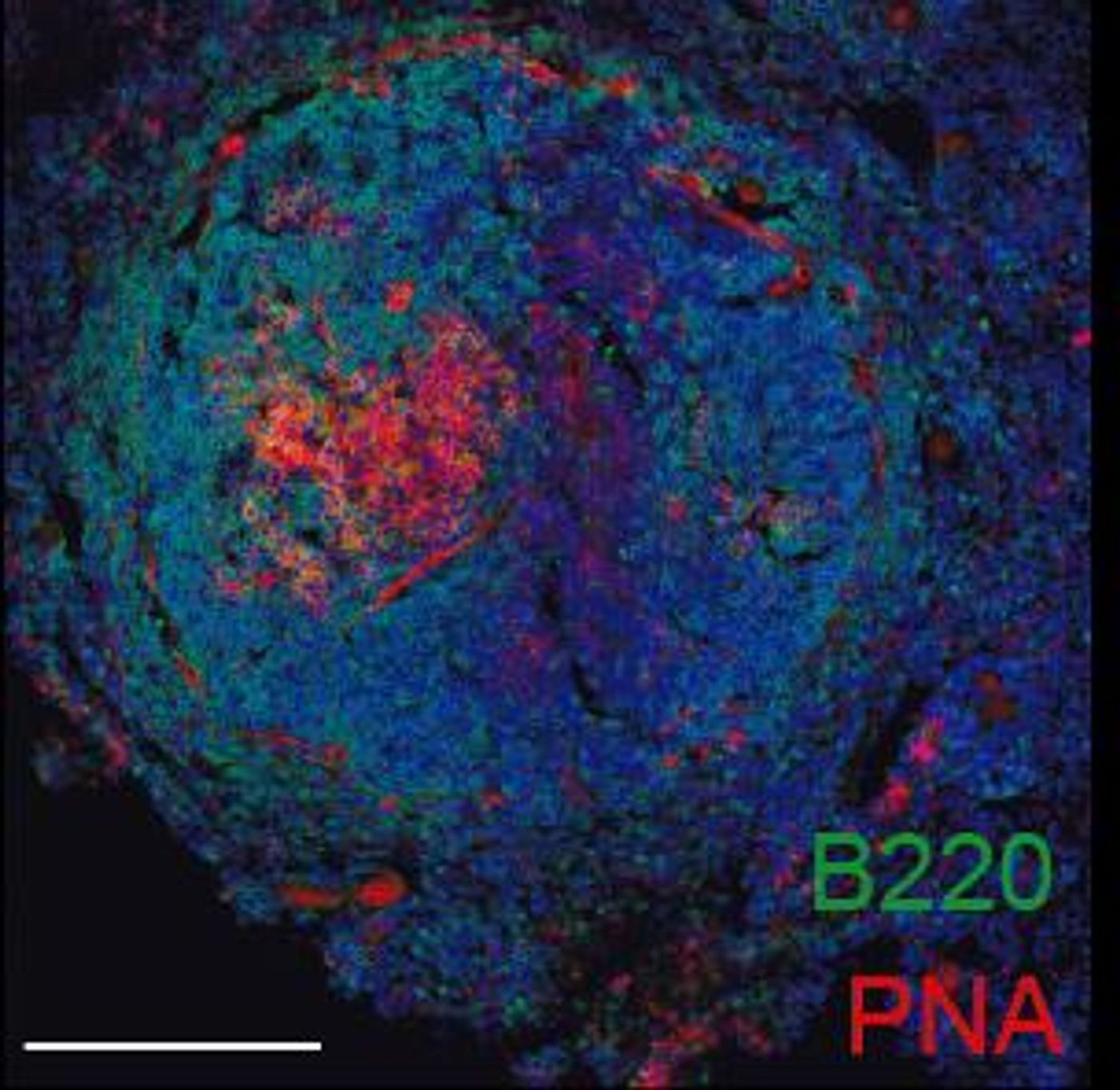
"We found that atherosclerosis is associated with the generation of specific antibodies in the germinal centers, where B cells diversify their antibodies and differentiate into high-affinity memory B cells and plasma cells," revealed first study author Cristina Lorenzo.
The researchers wanted to characterize the antibodies that were generated, so they isolated B cells and sequenced the antibody genes they contained.
"Analysis of the sequences of more than 1700 antibody genes showed that mice with atherosclerosis produced a distinct antibody repertoire. The production of these antibodies allowed us to study their targets (their antigen specificity) and their functional properties," explained study co-author Hedda Wardemann of the German Cancer Research Center (DKFZ) in Heidelberg.
The researchers examined the antibodies linked to artherosclerosis and found that one, A12, could identify plaques in the mouse model (which is prone to artherosclerosis) as well as humans with artherosclerosis in their carotid arteries.
"Proteomics analysis showed that A12 specifically recognized a mitochondrial protein called aldehyde dehydrogenase 4 family, member A1 (ALDH4A1), identifying this protein as an autoantigen in the context of atherosclerosis," explained Lorenzo.
Artherosclerosis can develop over a period of years without showing any symptoms for years. If there were markers of the disorder, we may be able to prevent fatal heart conditions.
"The study shows that ALDH4A1 accumulates in plaques and that its plasma concentration is elevated in the atherosclerosis-prone mice and in human patients with carotid atherosclerosis, establishing ALDH4A1 as a possible biomarker of the disease," noted Ramiro.
When the atherosclerotic mice were infused with A12 antibodies, plaque formation was delayed. Levels of free cholesterol and LDL in circulation were also lowered.
"These results broaden our knowledge of the humoral response during atherosclerosis and highlight the potential of ALDH4A1 as a new biomarker and of A12 as a therapeutic agent for this disease," added Ramiro.
Sources: AAAS/Eurekalert! via Centro Nacional de Investigaciones Cardiovasculares (CNIC), Nature