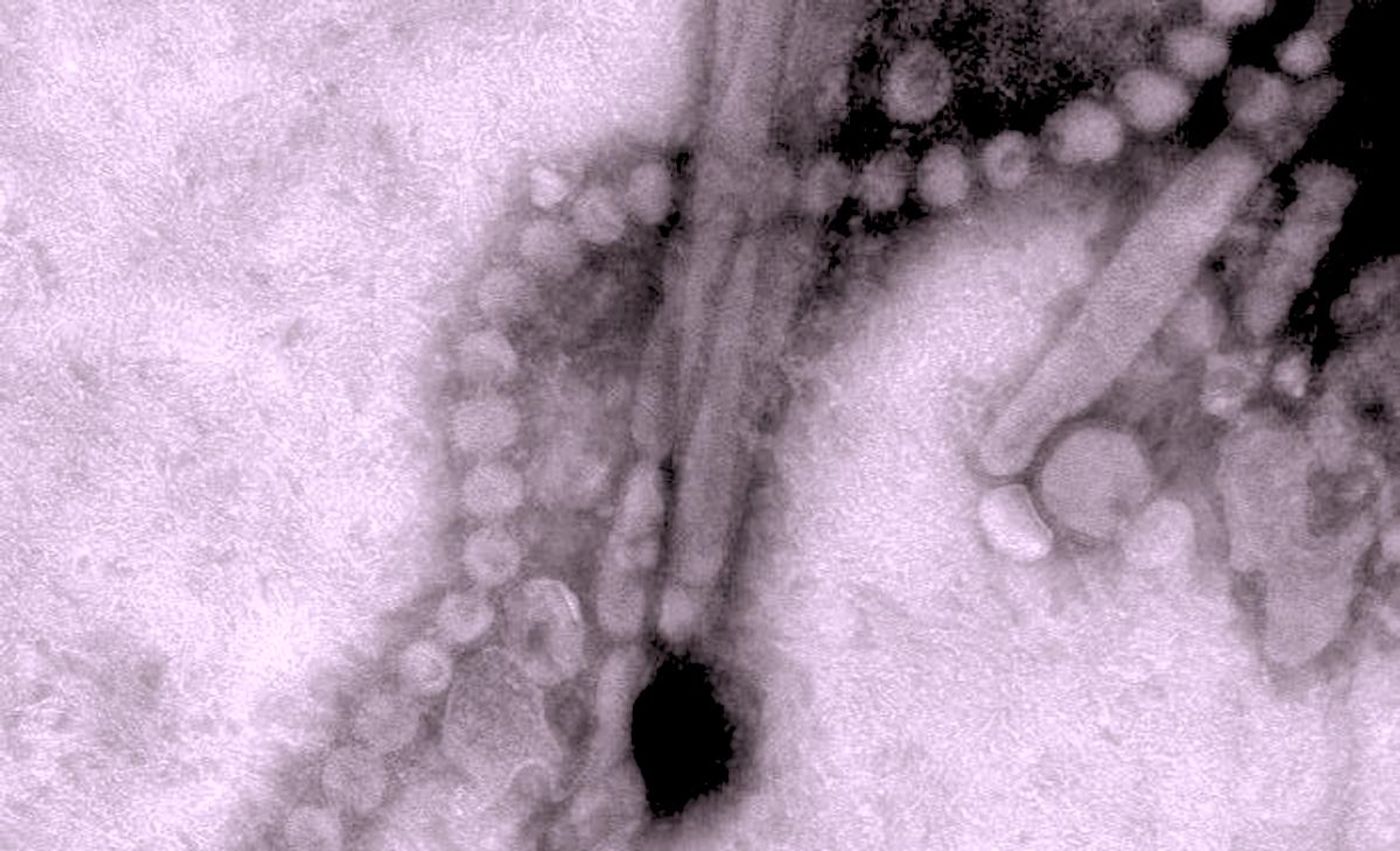
The Immune Response to Infection and Vaccination Depends on Previous Infections
After we are exposed to a pathogen or in the case of vaccines, a portion of a pathogen, our body mounts an immune response, which will be faster-acting in case of a second exposure. Scientists have now found evidence that pre-existing immunity, and whether it came about through natural infection or vaccination, dramatically affects the antibody response to influenza viruses. The work, which was reported in Science Translational Medicine, has suggested that annual flu vaccines are very important to produce the best immune response.
When antibodies are generated in response to an infection, they can be both non-neutralizing, which won't stop an infection, and neutralizing, which will. This work indicated that most antibodies that are initially produced after both flu infections and vaccinations are derived from older white blood cells that produce antibodies, called B cells. The antibodies that were made were more reactive against strains that were in circulation when a person was a child compared to more recently circulating strains. The researchers suggested this means that a person's existing immune memory is very important to how their body first reacts to a viral infection.
"Most interestingly, we found that people who were actively sick with influenza had old antibodies that predominantly targeted parts of the virus that don't change -- but those antibodies specifically targeted non-neutralizing sites," said co-first study author Haley Dugan, a graduate candidate in immunology. "When we tested these same antibodies in mice, they weren't able to protect them from being infected with influenza."
This research can help provide insight into how pre-existing immunity affects the production of antibodies after infection and vaccination. Universal vaccines would have to use parts of the flu virus that stay the same over time, or are conserved, so that antibodies will work against the virus as the rest of it changes year after year.
The scientists also found that flu vaccines tended to boost antibodies against conserved portions of the virus that are also neutralizing. Vaccinations may be drawing on pre-existing immune responses in order to generate more efficient antibodies. People that were vaccinated also tended to produce many antibodies against both new and mutated parts of the virus.
For a vaccine to be effective, it has to trigger a neutralizing immune response against a portion of the pathogen, without causing infection. The memory B cells that are made after the body is exposed to a virus survive for decades and will continue to work against the virus, but not if it mutates too much. Influenza can mutate fast enough to get around the immune memory. Therefore, researchers try to design vaccines to work against parts of the flu virus that are less likely to mutate. The quality of a person's immune response also depends on many things including age.
"For people who have caught the flu, their pre-existing immunity may make them susceptible to infection or increase the severity of their influenza symptoms if their antibodies are targeting 'bad' or non-neutralizing viral sites," noted co-first author and postdoctoral fellow Jenna Guthmiller, Ph.D.
"This study provides a major framework for understanding how pre-existing immunity shapes protective antibody responses to influenza in humans," said lead study author Patrick Wilson, Ph.D., a professor of immunology. "We need more studies to determine whether the targeting of specific neutralizing and non-neutralizing viral sites directly impacts a person's likelihood of becoming ill."
Sources: AAAS/Eurekalert! via University of Chicago Medical Center, Science Translational Medicine