Human Malaria Trial Creates More Questions
Malaria is a major health problem in many parts of the world; nearly half a million people die from malaria, and another 220 million are infected every year. Mosquitoes spread the disease through their bites, infecting humans with a pathogenic parasite called Plasmodium falciparum that has a complex life cycle. Scientists have now studied people who were infected with malaria, which might not cause any symptoms in some people, but could be life-threatening in others. The research found that there was a wide range of immune responses in infected individuals. The work, which was reported in eLife, has generated new questions about malaria.
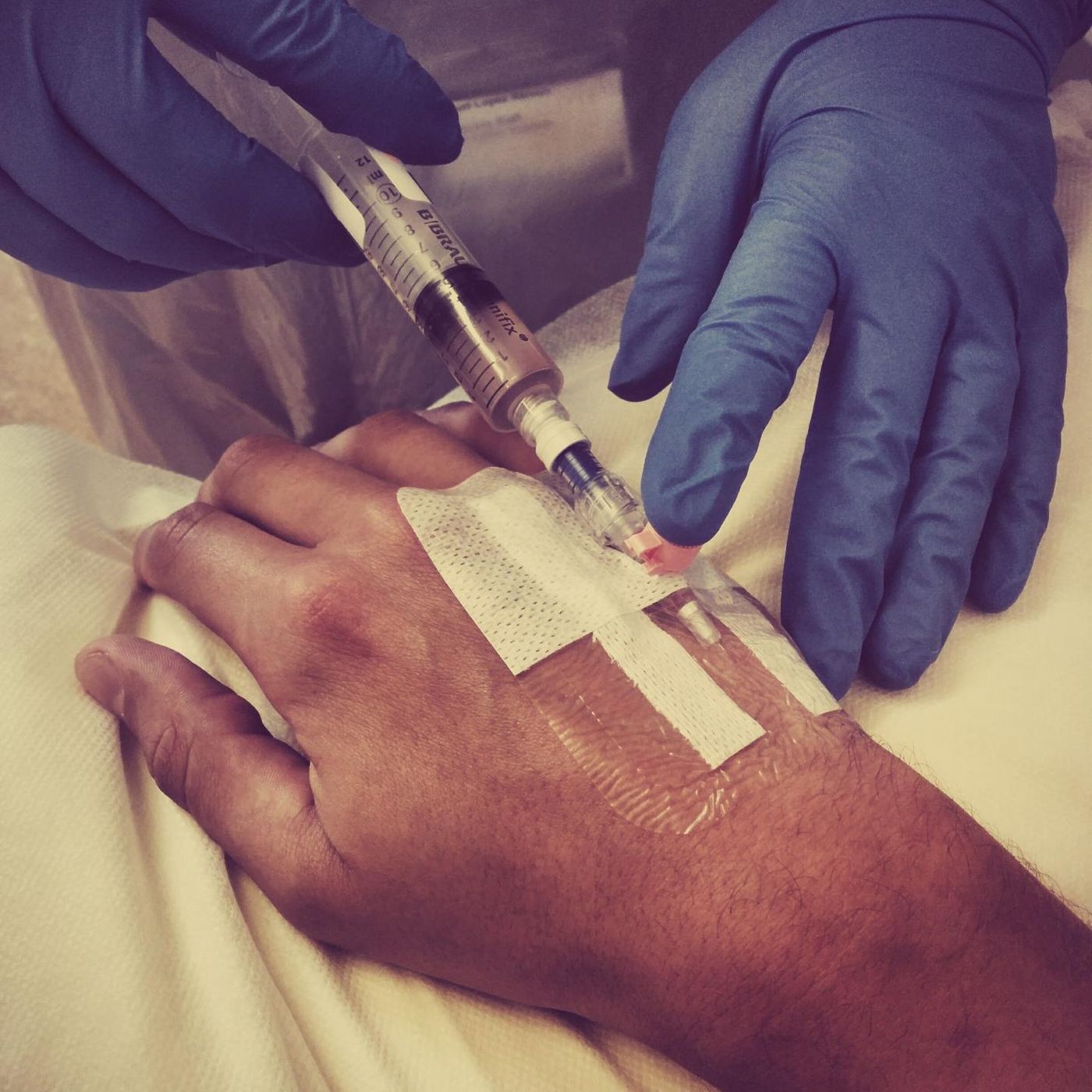
In this study, fourteen people were deliberately infected with malaria parasites. Since there are treatments for the disease, these individuals volunteered, and the scientists monitored the volunteers' responses to the parasite over ten days, after which time the group was treated with antimalarial drugs, the deliberate infection was considered ethical. The researchers cured the study volunteers of their infections before they could develop severe symptoms.
In about half of the study participants, the immune system was rapidly alerted to the parasites, and the host initiated signals to mount a response against the parasite. These people also started to show symptoms of malaria, like fever and headache. In the rest of the study participants, however, there were no symptoms, and there was either no sign of immune system activation, or the host actually began to dampen immune responses.
"It looks like most of the variation in malaria is due to intrinsic differences between people in how they respond to infection," suggested one co-leader of the study, Dr. Phil Spence, Sir Henry Dale Fellow at the Institute of Infection and Immunology Research at the University of Edinburgh. "We need to do further work to tease out the underlying factors responsible for immune variation, such as investigating human genetics and prior experience of other infections."
The scientists also wanted to know if there were variables in the growth rate of the parasite or its virulence factors that influenced the severity of an infection. They found that there were significant differences in the growth rate of the parasite in different volunteers, but that was not connected to the severity of infection or its outcome. For example, a volunteer might carry a low level of parasites and show a strong immune reaction, while another had a high level of parasites but not have any symptoms.
There also did not appear to be any meaningful differences in the virulence factors (some of which include group A var genes) in the parasites.
"The biggest surprise from our study was that there was no variation in expression of the parasite virulence factors," noted study co-leader Professor Alex Rowe, Personal Chair of Molecular Medicine at the Institute of Infection and Immunology Research at the University of Edinburgh. "Current theory, based on data from infected patients in malarious countries, suggested that parasites expressing group A var genes would rapidly come to dominate as the infection progressed, but this was not seen in our volunteers.
"There are many possible reasons for this: maybe a parasite collected more recently from a field site would give a different result, or maybe longer infection times are needed so the host immune response can influence these changes."
The research shows how important it can be to study health outcomes and disease in people, and not only rely on animal models.
Sources: AAAS/Eurekalert! via University of Edinburgh, eLife