In a Twist, Researchers Suggest Some Alzheimer Plaques are Protective
Scientists have long known that in Alzheimer's disease (AD), there is an abnormal buildup of some proteins in and around cells in the brain, which forms plaques. Tau is one of those proteins, and beta-amyloid is another, which is found in several forms. Some treatments that have been developed for AD have been aimed at those plaques, but so far, they haven't been very successful. Now scientists may have an explanation for that, which might also change how we think of AD.
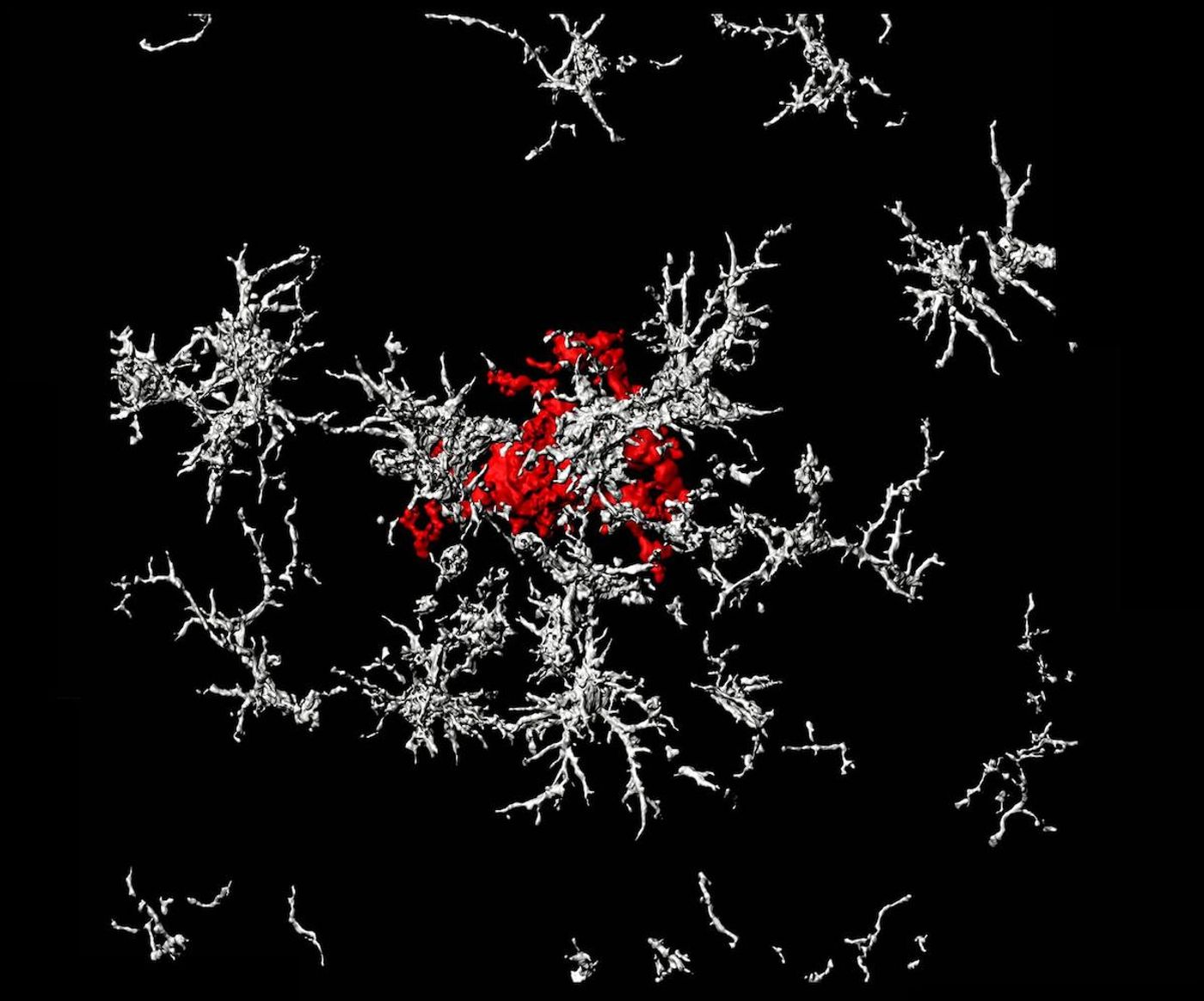
This study, which has been reported in Nature Immunology, suggests that certain brain cells called microglia actually promote the formation of plaques. Microglia act as immune defenders in the brain, and it had been thought that they could consume plaques and inhibit their growth. This work has indicated, however, that microglia encourage dense-core plaques to form, and they are actually protective, so any treatment that targets them for destruction would not be therapeutic and might be harmful.
"We show that dense-core plaques don't form spontaneously. We believe they're built by microglia as a defense mechanism, so they may be best left alone," said Greg Lemke, a professor in the Salk Institute's Molecular Neurobiology Laboratory. "There are various efforts to get the FDA to approve antibodies whose main clinical effect is reducing dense-core plaque formation, but we make the argument that breaking up the plaque may be doing more damage."
It's thought that AD causes memory loss and impairs cognitive function because the accumulation of abnormal proteins creates plaques that disrupt cellular activity, causing brain cells to die. The two most common types of plaque are either 'diffuse,' and loosely organized, or 'dense-core,' which have a tight center surrounded by a halo. Amyloid precursor protein (APP) was thought to play a role in the formation of both types of plaques.
This study upends that view by suggesting microglia form dense-core plaques as they mop up diffuse amyloid-beta fibrils. The researchers found that amyloid plaques send a signal that they should be consumed. Using an animal model, they demonstrated that a receptor called TAM on microglia cells interacts with a protein called Gas6 to consume the plaques.
Further research with live imaging showed that once a microglia cell consumes a diffuse plaque, the amyloid-beta protein that's engulfed is transferred to a compartment that's very acidic. There, the diffuse plaque is transformed into a dense-core plaque. The study authors suggested that this mechanism might be a beneficial one that removes debris from the intercellular environment.
"Our research seems to show that when there are fewer dense-core plaques, there seem to be more detrimental effects," said first study author Youtong Huang. "With more diffuse plaques, there's an abundance of dystrophic neurites, a proxy for neuronal damage. I don't think there's a distinct clinical decision on which form of plaque is more or less detrimental, but through our research, we seem to find that dense-core plaques are a bit more benign."
This work may lead to new approaches in SD, and therapeutics that work better.
"Some people are saying that the relative failure of trials that bust up dense-core plaques refutes the idea that amyloid-beta is a bad thing in the brain," said Lemke. "But we argue that amyloid-beta is still clearly a bad thing; it's just that you've got to ask whether dense-core plaques are a bad thing."
Sources: AAAS/Eurekalert! via Salk Institute, Nature Immunology