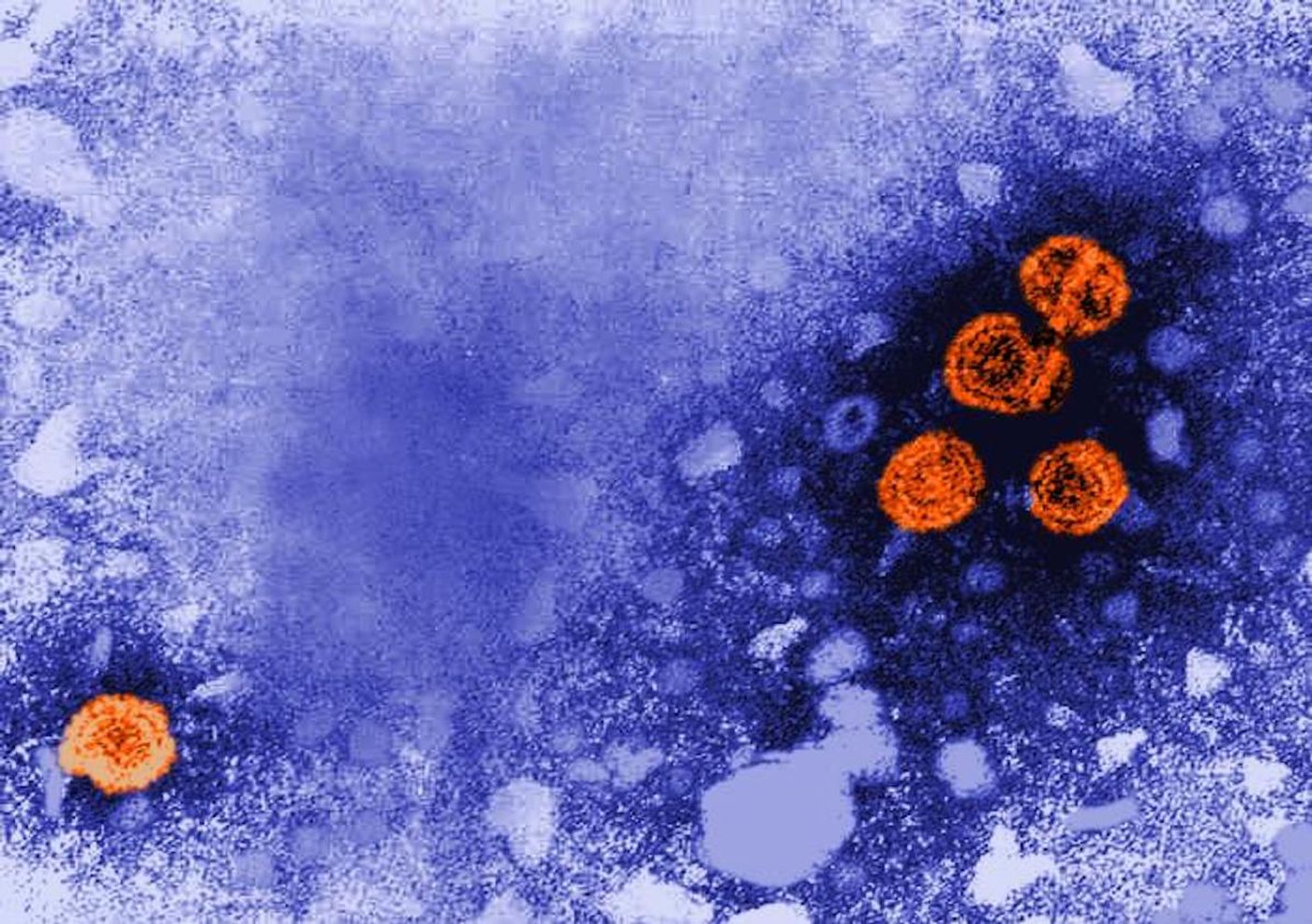
Viral Infection Can Have a Lasting Impact on Cells
When a virus infects a cell, it usually takes over the cell's machinery to start churning out viral particles, which are thought to be released when the infected cell bursts. That leads to the infection of more cells, starting the process over. But viruses don't always kill every cell they infect; some viruses can get into cells and lurk there for a long time, maintaining the infection or waiting for an opportune time to proliferate, while others may coexist with the cell. Researchers have now learned more about cells that are infected by viruses but don't die. Some of these cells appear to undergo long-term changes in gene expression, which may be related to liver cancer susceptibility in hepatitis C patients.
It's been thought that viruses that can cause chronic infection, like hepatitis B and C, remain in infected cells. But a new study in the the Journal of Experimental Medicine has suggested that these viruses can disappear from those cells, and may go on to infect new ones. The cells also seem to get rid of the virus on their own as well, without using immunological help.
“Liver cells seem to have their own mechanism for removing a virus from within,” said co-first study author Dr. Peter Reuther. The study suggested that chronic infection by these viruses is aided by the continuous infection of new cells.
This work used a mouse model of hepatitis C infection in which the mice are infected with something like human hepatitis, called lymphocytic choriomeningitis virus (LCMV), which also attacks the liver.
However, while the liver cells seem to be able to eject the virus, the cells don't get away unscathed. The researchers found that the gene activity in these infected and subsequently uninfected cells changes; gene expression levels are different from what's seen in cells of the same type that were not infected. Genes that are involved in cell metabolism and division seem to be particularly affected.
This work may help explain symptoms that linger or cause other problems, such as the increased risk of liver cancer in hepatitis C patients.
“We see significant parallels with other studies of cured hepatitis C patients. Their formerly infected liver cells show changes in the genetic material that influence genetic programs,” noted co-first study author Dr. Katrin Martin.
The researchers don't yet know how long the genetic shifts after viral infection persist. Additional work is also planned to look for changes in the genetics of cells in other organs after a temporary viral infection. The scientists also want to know how the cells are removing the virus that infects them.
“Two questions arise from a medical perspective,” noted team leader Professor Daniel Pinschewer of the University of Basel. “How can these viruses be prevented from spreading from cell to cell in a chronic infection and thus affecting a large number of cells? And is it possible to reverse the changes in the genetic profile and prevent subsequent damage?” The answers to these questions may have implications for other diseases including long COVID and asthma, he added.
Sources: University of Basel, Journal of Experimental Medicine