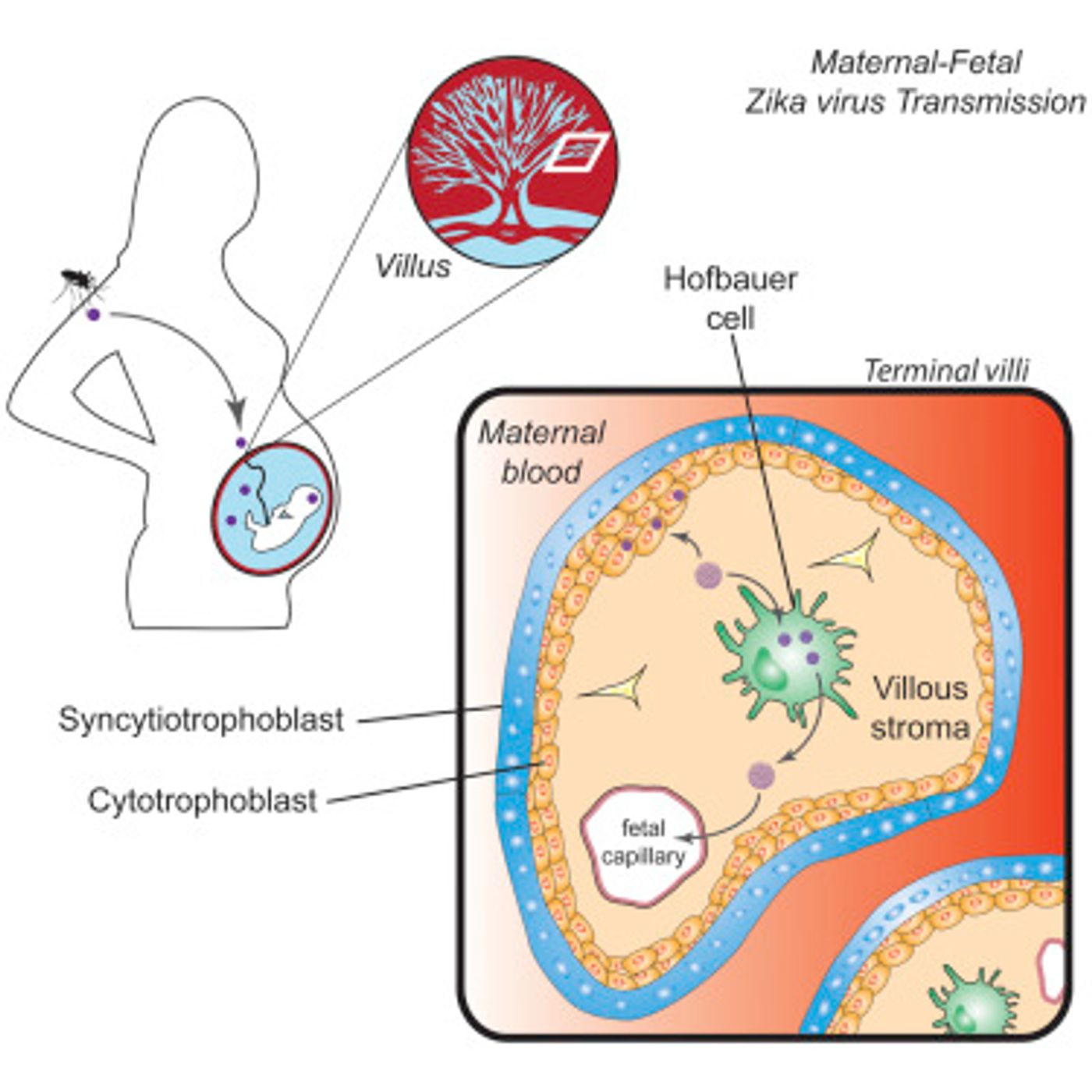
While the current Zika virus outbreak is known to be transmittable from mother to fetus, the exact mechanism of this transfer is unknown. The route may involve multiple cell types through an indirect mode of delivery. A new
study that was published in Cell Host & Microbe provides evidence for the theory that placental immune cells that have direct access to blood vessels of the fetus, called Hofbauer cells, are one of the cell types involved in this process.
"Our study indicates that this cell type may be a target for Zika virus in the placenta and replication in these cells may allow the virus to cross the placental barrier and enter the fetal circulation," said Rana Chakraborty, a pediatric infectious disease specialist at Emory University and one of the authors of the study.
"One group has recently discovered viral antigen in Hofbauer cells collected from placental tissue of a fetus that unfortunately died as a result of Zika virus infection," added senior author and Assistant Professor of Pediatrics at the Emory, Mehul Suthar.
In this work, the scientists looked at full-term placental tissue samples, donated by five women who had delivered by Caesarean section, to find cell types that could be vulnerable to infection from Zika virus. They infected the tissue with a strain of Zika virus that is currently spreading in Puerto Rico. Hofbauer cells are macrophages of the placenta that come from the mesenchymal stem cells of a developing fetus. Zika virus infection was found there in the Hofbauer cells. It was also revealed to a lesser extent in cells located in the middle layer of the placental barrier, called cytotrophoblasts. The team found that while the virus infects Hofbauer cells right away, the cytotrophoblasts only become infected after a couple of days.
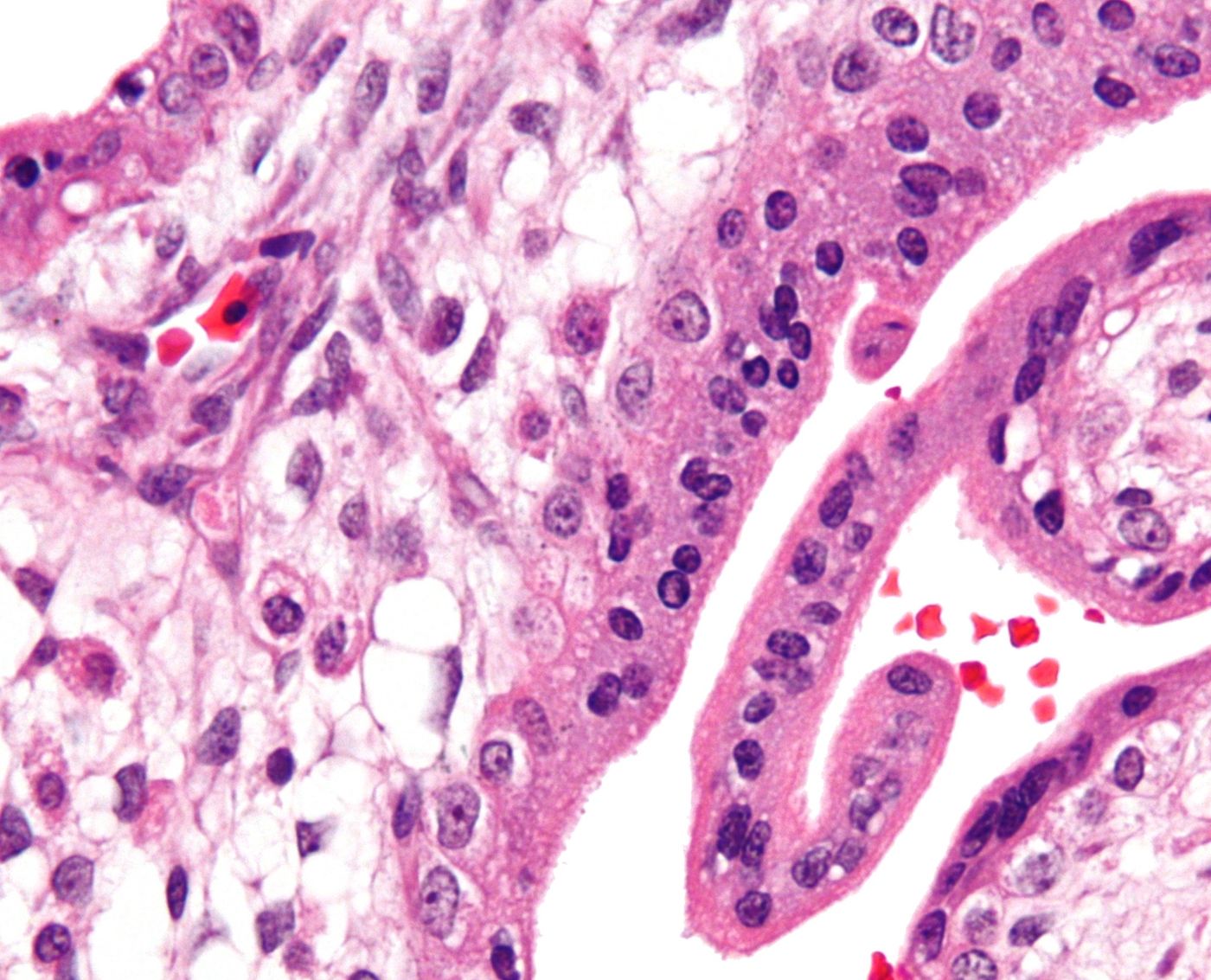
This work indicates that cytotrophoblasts are more permissive for Zika virus infection than the outer layer of the placenta, called the syncytiotrophoblast layer, previously shown to be impervious to Zika infection. The hypothesis is then that if the virus can cross the syncytiotrophoblast, the virus then has access to cells where it can penetrate and replicate.
One intriguing finding from the study was that the placental cells there were varying levels of viral replication over time in the five different samples. "A concept that is emerging is how host genetics or other non-viral factors, including nutrition and microbiota, influence your immune response," Suthar said. "What our study suggests is not everyone is predisposed to having the virus replicate in the placenta, but the full meaning of this needs to be explored further."
Hofbauer cells were identified more than a 100 years ago and yet there is very little information known about them. Overall, the Zika epidemic has certainly highlighted the dearth of facts we have about the human placenta and indicates that it’s an area ripe for more research.
Sources:
Cell Host & Microbe,
AAAS