Genes Have an Influence on our Response to Infection
When an infectious illness sickens multiple people, they often respond in different ways; there can be differences in symptoms that people exhibit, or a range of severities, or sometimes some infected people don’t get sick at all. New research has suggested that small variations in our genetics are to blame for the varied responses. The work, reported in Nature Communications, shows that infections cause changes in gene expression levels, but those changes are different in different people. Genes alter the response to the illness. The video below outlines the work.
"We wanted to understand how genetic differences between individuals affect this cellular response to infection," said one senior author, Dr. Johannes Schumacher of the University of Bonn.
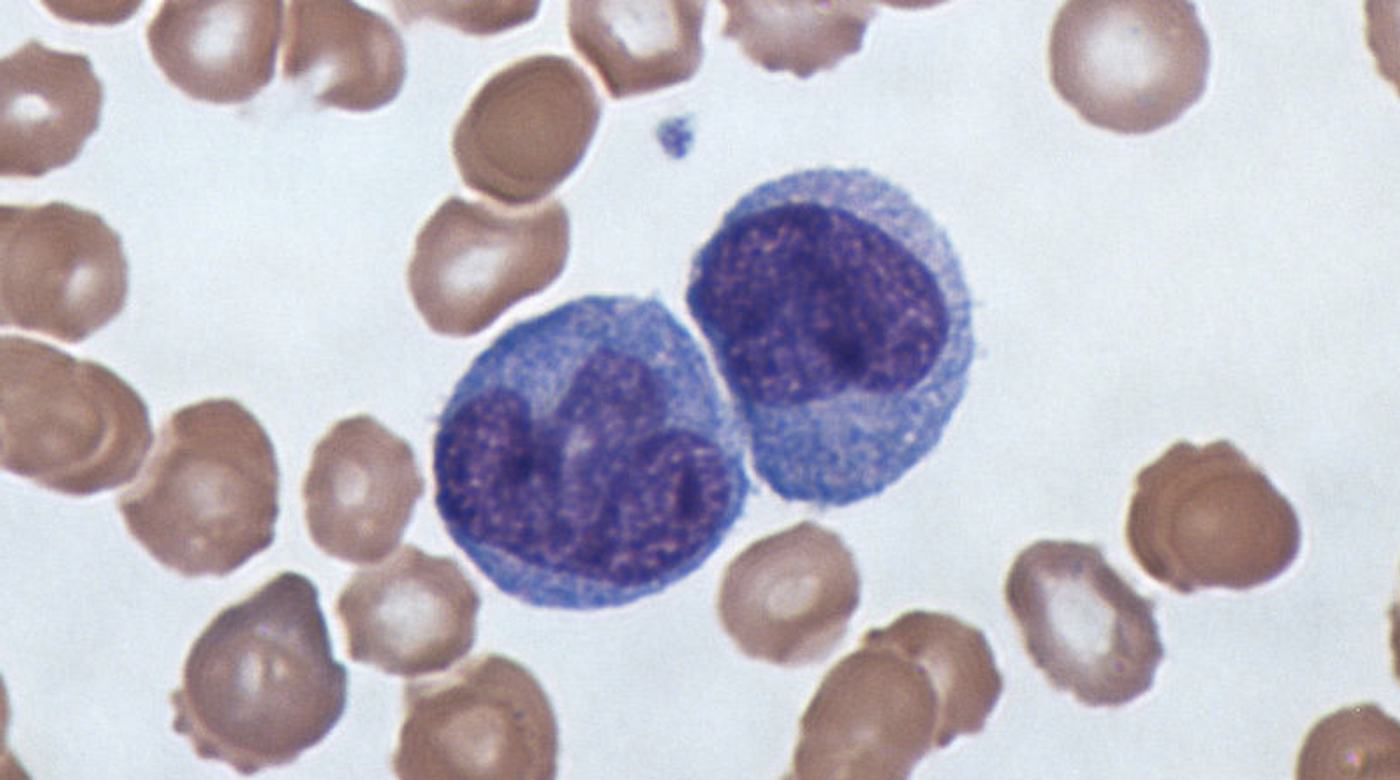
"Our defense mechanisms against microbial pathogens rely on white blood cells that are specialized to detect infection. Upon encounter of microbes, these cells trigger cellular defense programs via activating and repressing the expression of hundreds of genes," explained Dr. Veit Hornung of the Ludwig-Maxmilians-Universität in Munich and another senior author of the study. The researchers used donated monocytes from 134 volunteers for this research.
The immune system not only fights infectious disease; through inflammation and autoimmunity, it can also play a role in many other diseases. Small differences in genes the investigators identified were affecting the immune system and its response to infection.
"These genes include many of the well-known genes of the human immune system, demonstrating that genetic variation has an important role in how the human immune system works," said lead author Dr. Sarah Kim-Hellmuth of the New York Genome Center, Columbia University. "While earlier studies have mapped some of these effects, this study is particularly comprehensive, with three stimuli and two time points analyzed."
Some of the genetic variants identified in the study had links to celiac disease, others were associated with cholesterol level. The variants had different effects on gene regulation depending on a cell’s infectious state.
Because gene expression patterns were analyzed at the population level, researchers were able to show how innate immune responses differed widely among individuals that were exposed to myriad pathogens on multiple occasions. The study suggested that genetics underpins the many differences in immune response among the members of a population. It also showed that the immune system influences genetic association with disease. The work provides some insight into how genetic elements impact the response to environmental stimuli, as well as the dynamics of immune response.
"This supports a paradigm where genetic disease risk is sometimes driven not by genetic variants causing constant cellular dysregulation, but by causing a failure to respond properly to environmental conditions such as infection," said co-senior author Dr. Tuuli Lappalainen of the New York Genome Center and Columbia University.
”It's been known for a long time that most diseases have both genetic and environmental risk factors. But it's actually more complicated than that because genes and environment interact. As demonstrated in our study, a genetic risk factor may manifest only in certain environments," explained Dr. Lappalainen. "We are still in early stages of understanding the interplay of genetics and environment, but our results indicate that this is a key component of human biology and disease. The molecular approach that we took in our study can be a particularly powerful way for researchers to delve deeper into this question."
Sources: Science Daily via New York Genome Center, Nature Communications