Nanoparticles provide momentum for better diagnostic imaging
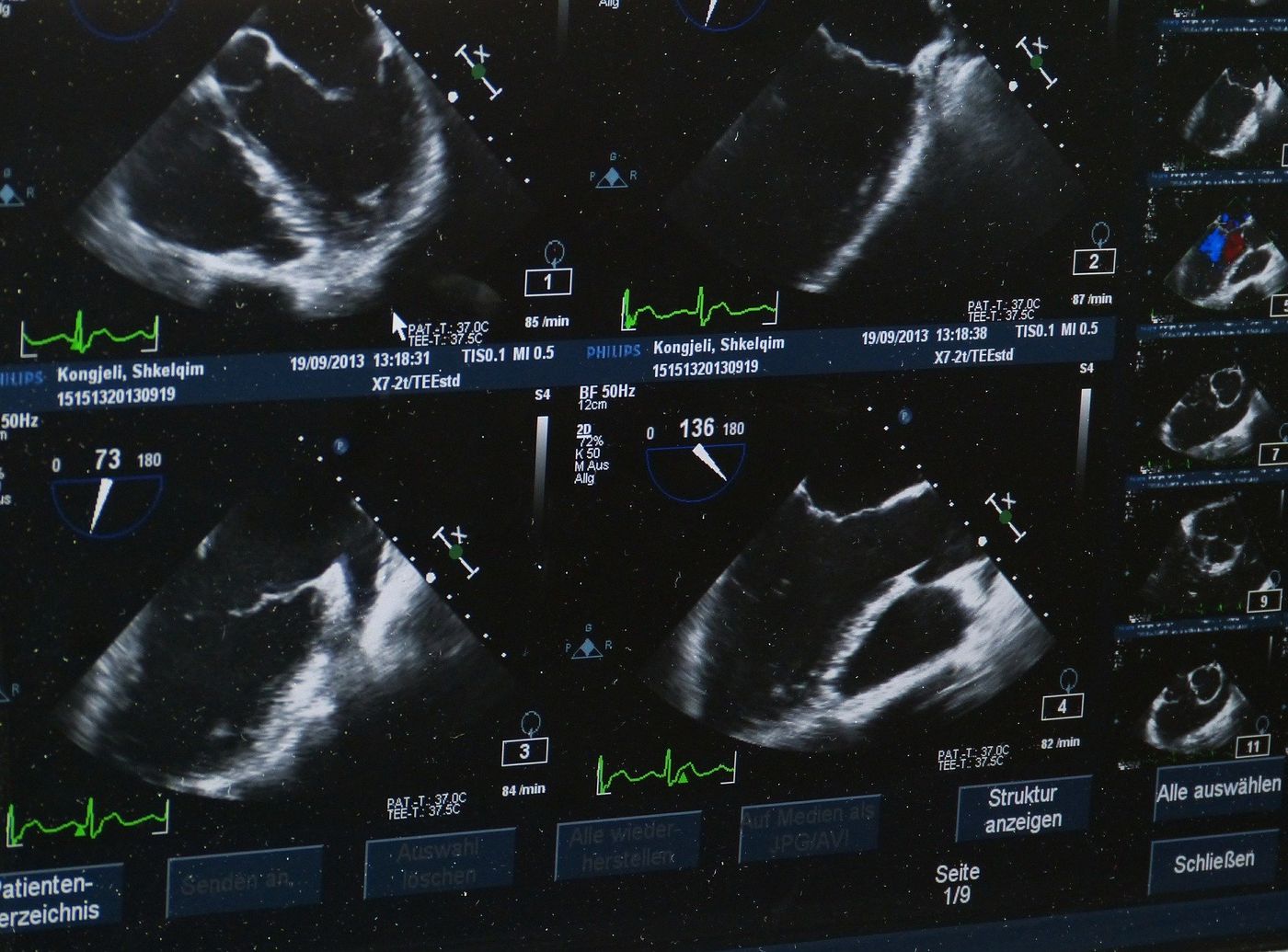
Photoacoustic imaging is an emerging tool with a vast array of biomedical applications ranging from the detection of brain lesions to imaging early signs of breast cancer. This technique leverages the imaging capacities of both light excitation and ultrasound wave detection to enable noninvasive, high-resolution imaging of tissue and organ systems within the body.
This translates to a physician being empowered with the ability to monitor, in real-time, oxygen saturation in the blood, the distribution of specific molecular biomarkers in a tumor or how a drug is being absorbed in the body of a patient after injection.
How does photoacoustic imaging work? First, pulsating laser light is applied to the part of the body to be imaged. This light is absorbed by the tissue, causing acoustic waves to be generated. These are then detected to image select biological processes occurring several centimeters beneath the surface of the skin. Contrast agents introduced systemically can drastically improve the resolution and specificity of the images captured in the area of interest.
A recent study published in WIREs Nanomedicine and Nanobiotechnology describes advancements and challenges associated with the use of different photoacoustic imaging contrast agents for medical and research applications.
Authors and imaging experts Paul Kumar Upputuri and Manojit Pramanik from the School of Chemical and Biomedical Engineering at Singapore’s Nanyang Technological University provided their insights on trends in the field.
To harness the full potential of photoacoustic imaging as a medical diagnostic platform, the clear resolution of the underlying tissue architecture is paramount. Improving this resolution is a major focus for scientists who are hoping to establish photoacoustic imaging as a widely-used diagnostic technique.
This is where nanoparticles can help. Researchers and diagnostic imagers currently have access to a toolbox of nanoparticle contrast agents including carbon nanotubes, bismuth selenide nanoplates and silver nanostructures. While such nanoparticles may possess excellent optical properties, administering them into the bloodstream of patients is not always feasible.
The next phase in the evolution of this technology will see the development of more biocompatible and biodegradable contrast nanoagents, with better safety profiles for routine internal use.
“Recent progress in the field of biodegradable and metabolizable nanoparticles with potential use in clinical applications makes us hopeful that soon these nanoagents will be traveling inside our body to reveal more than what we can see at present,” says Pramanik.
Sources: Advanced Science News, WIREs Nanomedicine and Nanobiotechnology.