Digital Platform Watches for a Silent COVID Killer
“Silent hypoxia” is a phenomenon where oxygen levels in COVID-19 patients plummet to dangerously low levels, without any accompanying signs or symptoms to indicate to medical staff that something is wrong. As COVID case numbers ramped up, ER doctors began reporting more and more incidents of this silent killer. Without warnings such as shortness of breath, hospitalized COVID patients can rapidly deteriorate as organ systems fail due to a lack of oxygen.
Under normal conditions, blood oxygen saturation levels are typically around 90 to 100 percent at sea level. Once hypoxia creeps in, however, these can dip to as low as 50 percent.
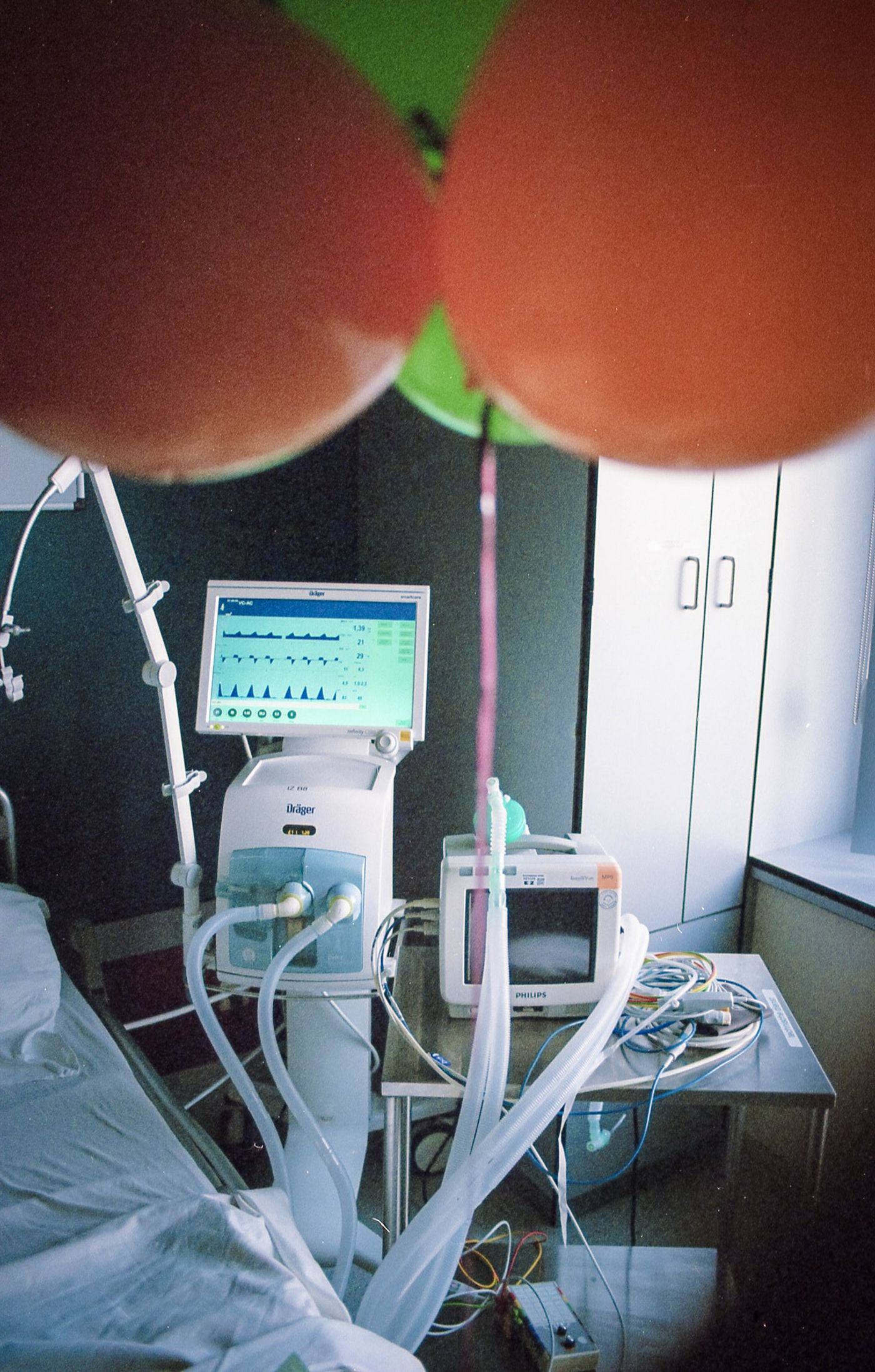
Given the life-threatening nature of this condition, healthcare personnel now primed to vigilantly monitor blood oxygen saturation levels in COVID patients using a device called a pulse oximeter. The conventional method of tracking these levels is manual — nurses and physicians take routine recordings and write them down on patients’ charts. An automated, digital process, however, is far more favorable as this frees up staff bandwidth and is more accurate and sensitive.
To this end, scientists from the National University of Singapore have created an open-sourced system that wirelessly measures oxygen levels taken from Bluetooth-enabled pulse oximeters and transmits these readings to an e-dashboard.
"Our aim is to bring the convenience of digital technology to the pen-and-paper process currently being used to take health measurements," said Assistant Professor John Ho from the Institute of Health Innovation and Technology.
The fully automated system is simple and seamless. Patients clip on the special Bluetooth-enabled pulse oximeters onto their index finger, where a measurement is taken at regular intervals, each reading taking a mere 30 seconds. The data is sent wirelessly and securely to the cloud via wi-fi stations dispersed throughout the healthcare facility. End-users (including the patients themselves) can easily track oxygen saturation levels via a smartphone or laptop. In the event of an abnormal reading, alerts are sent off to healthcare teams, triggering follow-up clinical interventions.
Pilot studies have demonstrated the accuracy and efficacy of the digital platform and the research team plans to commercialize the technology in collaboration with industry partners. "We are continually updating the system to address evolving healthcare needs surrounding care for COVID-19. We hope to add additional sensors, such as those for measuring temperature, to provide an integrated health monitoring system," commented Prof. Ho.
Sources: NUS News, Global News, The New York Times.