In a time when precision medicine and genetic testing are booming, the Federal Drug Administration (FDA) is taking a step back and stringently re-examining the accuracy of laboratory-developed tests.
A recent
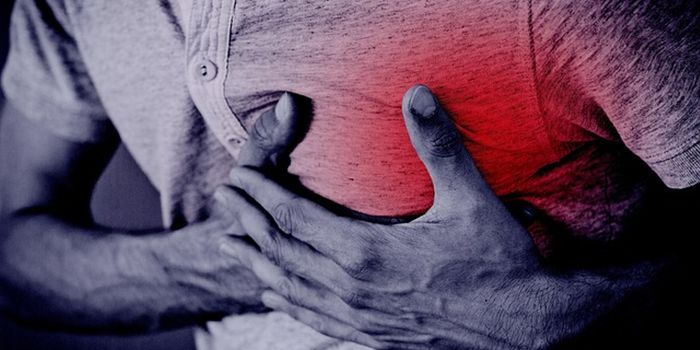
FDA report to Congress examined 20 case studies of laboratory-developed tests (LDTs) that did not meet FDA requirements. The report concluded that these tests “may have caused or have caused actual harm to patients.” Of the 20 case studies, 10 involved tests used to diagnose and treat cancer, while the remaining 10 involved heart disease, Lyme disease, and autism. In all 20, the FDA outlined many serious diagnostic problems of the LDTs and the clinical implications of such inaccurate test results.
Several ovarian cancer screening and detection tests (OvaCheck, OvaSure Screening Test) claim to use biomarkers in blood samples to detect presence of cancer cells. The FDA found that for both tests, there were no validations that the tests actually predict or detect ovarian cancer. In addition, the tests had inflated positive predictive values, meaning that their accuracy claims are unsubstantiated and the tests result in a high number of false positives. Since the screens target women at risk for ovarian cancer, false-positive results may lead women to undergo unnecessary surgery to remove their healthy ovaries, while false-negative results may lead to inappropriate treatments.
Another test that has the potential to yield too many false-negatives and false-positive results is non-invasive prenatal testing, also known as cell-free DNA testing. While these tests have been lauded for being non-invasive and safer than traditional amniocentesis and chorionic villi sampling, the FDA found a “lack of clinical validation that tests detect and predict fetal abnormalities at an appropriate rate.” Further, the report cited “many false-positive results when used in the general population.” The consequences of these inaccurate results could lead women to unnecessarily abort a normal pregnancy or “deliver a child with an unanticipated genetic syndrome.”
The report also included LDTs that claim to identify causes and treatments for a disease based on “disproven scientific concepts.” Case in point, an LTD (CARE Clinics BioMarkers) that claims to determine cause for autism spectrum disorder reportedly shows “no evidence that [causes] identified by the test correlate with autism. Even worse, the LTD recommends treatments that include chelation, hyperbaric oxygen, and intravenous vitamin therapy. These interventions have shown no evidence to be effective and have all been discredited by the medical community.
In addition to direct patient harm, the FDA cited the high financial costs of these inaccurate and unreliable LDTs. For autism, the FDA estimates the cost impact of the inaccuracy to be $66.1 million for the 2,027 children tested and treated by the CARE Clinics. And for each ovary removal due to a false-positive ovarian cancer result, the cost of the inaccuracy is over $12,000. On the other hand, for each false-negative breast cancer result, the cost of inaccuracy is near $800,000.
Results of this report will likely promote more rigorous standards for LDT validation and regulation by the FDA. Some argue that the new standards will be the most significant change in the regulation of laboratories since 1988.
Additional Source:
NY Times