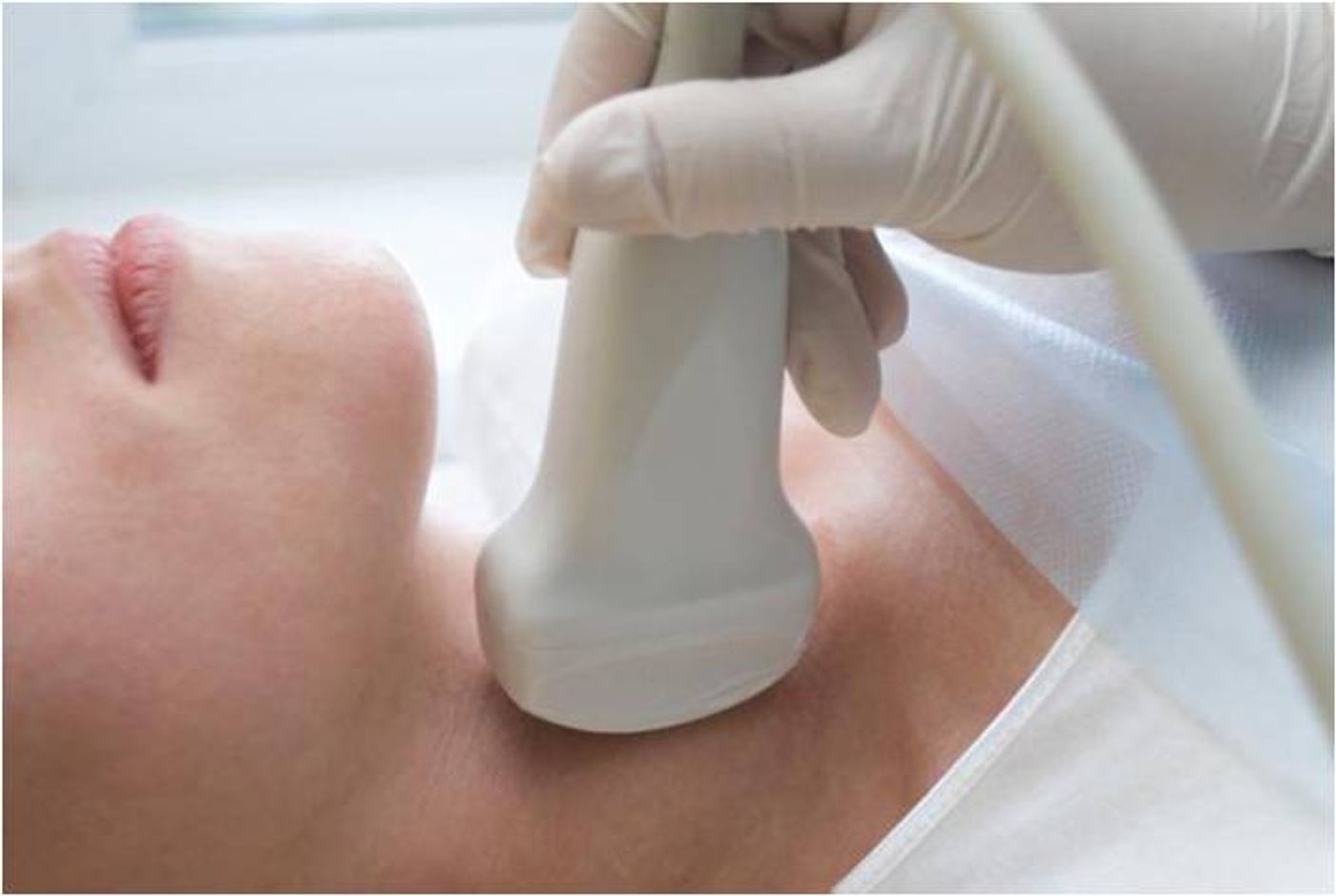
Instead of invasive biopsies, doctors could soon detect melanoma metastasis with a handheld scanning device. A team of researchers from Germany may have found a way to replace risky biopsies with audio-visual imaging techniques that detect cancer’s spread in the body.
Melanoma is the deadliest form of skin cancer caused by ultraviolet radiation damages to the skin cells. According to the Skin Cancer Foundation, melanoma kills over 9,000 Americans each year, making it the fifth most common cancer in the U.S.
According to the Melanoma Research Foundation, the most dangerous aspect of melanoma is its ability to metastasize – using the body’s lymph nodes to spread to distant sites like the liver, lung, bones, and brain. Thus, enlarged or abnormal lymph nodes can alert doctors of the cancer’s spread. But melanoma can also spread quietly, and even without enlargement, doctors perform a pre-emptive procedure known as sentinel lymph node biopsy (SLNB) to “grade” the cancer and check for metastasis.
The SLNB procedure involves injection of a radioactive substance or dye near the tumor to locate the position of the sentinel lymph node. Following the path of radioactivity or dye trail, the surgeons land upon the “sentinel” nodes, which get removed and analyzed for cancer presence.
This biopsy procedure detects metastatic melanoma in only about a third of patients; yet the procedure puts all patients at risk for infection and nerve damage to the head and neck area.
Researchers hope the new technique will bypass the biopsy all together.
The technique, called
multispectral opto-acoustic tomography (MSOT), uses light and sound to locate rogue melanin pigments in the sentinel lymph nodes. Instead of radioactive materials, researchers inject a green dye into the primary tumor site. Then the handheld MSOT illuminates the patient’s tissues with light pulses at multiple wavelengths, allowing researchers to track the dye’s path to sentinel nodes.
At the nodes, the device generates an ultrasound signal at the presence of melanin. Melanin pigment is produced only by melanoma cells, and its presence in the lymph nodes indicates that the melanoma has metastasized. Conversely no melanin indicates absence of metastasis, and prevents further unnecessary procedures.
The researchers tested the MSOT technique in 506 lymph node biopsies removed from 214 melanoma patients. Their technique reportedly outperformed the conventional diagnostic approach at correctly identifying cancer metastasis by 8.7%. Then in a group of 20 melanoma patients who had yet received surgery, the MSOT technique correctly visualized 100% cases of metastasis, ruling out cancer spread in more than 50% of patients.
A non-invasive and non-radioactive way to detect cancer metastasis sounds great! But is this technique good enough to replace biopsies? Not just yet. Though they reported 100% sensitivity, i.e. no false negatives, the specificity is low at 48-62%, meaning that around half of cases are identified as false positives. Ultimately, the researchers have to demonstrate that this technique is as good as lymph node surgery, and they can only do so with repeated trials in a much larger study size.
Source:
Science Translational Medicine,
Medline release