An effective treatment for Type 1 diabetes is to transplant new pancreatic islet cells into the patient. While this therapy has the potential to dramatically reduce and even eliminate dependence on external insulin shots, doctors still struggle with the process of preservation and handling of these islet cells. The solutions to these challenges involve seaweed, say researchers from the Okinawa Institute of Technology and Science Graduate University (OIST).
Type I diabetes usually begins in childhood, and occurs when a person's immune system destroys the islet cells in the pancreas that make insulin. Without the insulin hormone to process glucose, blood sugar levels rise dangerously high, which compromises many vital functions in the body.
Insulin-cell transplantation has improved leaps and bounds since the first procedure that was performed in 1990. The procedure is lauded for offering a more permanent solution to daily insulin shots, but at much less risk than total pancreas transplantation.
However, researchers have struggled to keep the harvested islet cells protected during the freezing and thawing process that’s required during cryopreservation and transplantation.
Islet cells are usually cryopreserved at below -190 Celsius. To get there, the cells need first to be frozen. But during the freezing process (-15 to -60 Celsius) the cells are vulnerable to ice crystals that can pierce its membranes. The same problem arises when the cryopreserved cells are thawed for transplantation.
To get around this problem, a team of researchers, led by Prof. Amy Shen from OIST in collaboration with the University of Washington and Wuhan University of Technology,
created a new cryopreservation method that prevents ice crystals from forming all together.
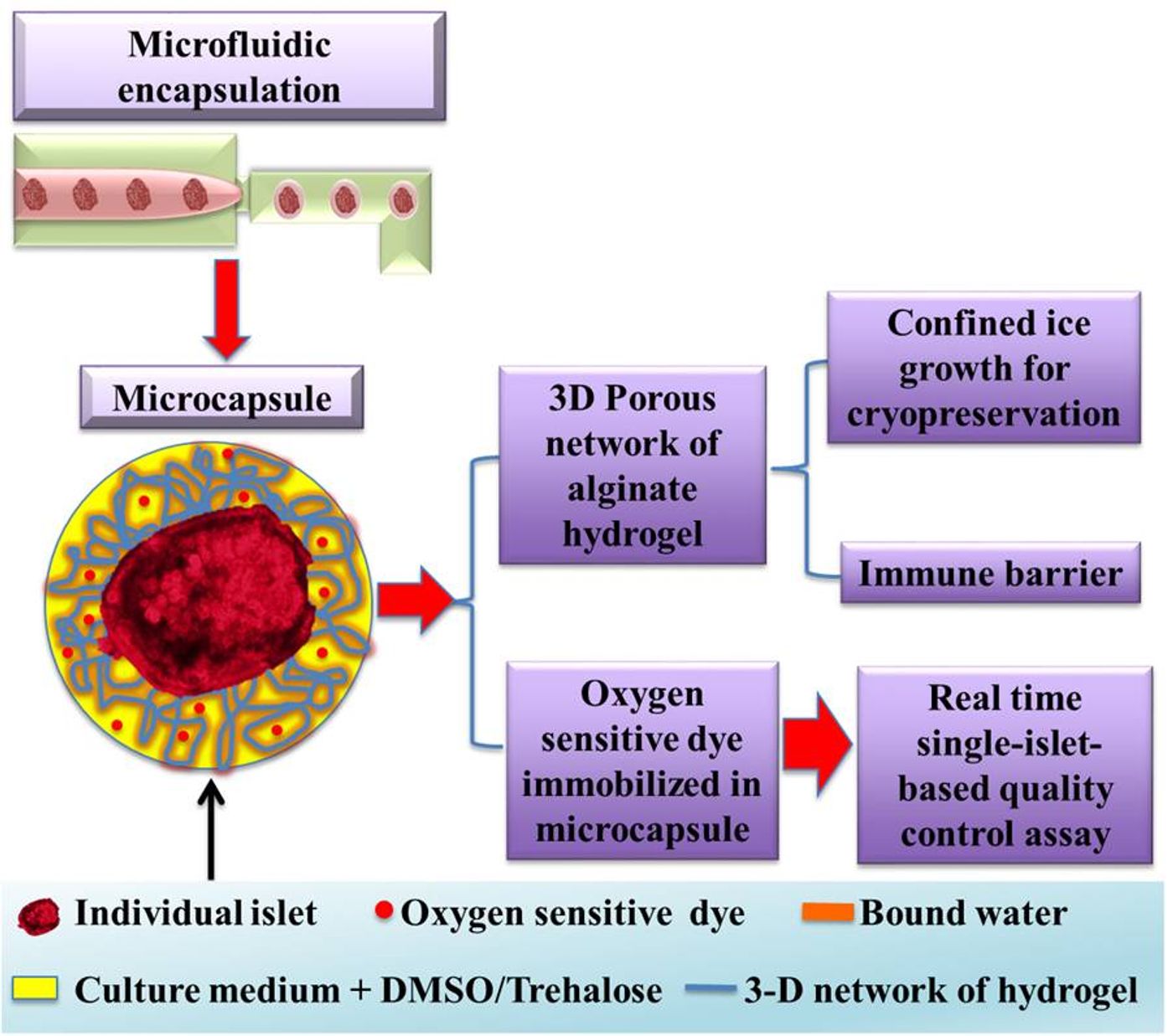
Their new technique is based on a hydrogel made from alginate, a gooey polymer extracted from seaweed. This hydrogel contains a non-freezable bound water that is immune to ice crystal formations because it does not freeze at all. Each individual islet cell is encapsulated inside this 3 dimensional network of hydrogel via a droplet microfluidic device. Essentially, the islet cell nests safely inside a protective seaweed goo that prevents ice crystals from getting in.
But this hydrogel is porous enough to let oxygen flow into the cells. To check the cell’s survival, the team attached a fluorescent oxygen-sensitive dye to the hydrogel capsules. Cells that consume oxygen, and thus alive, will fluoresce. This gives researchers a quick, real-time assessment on the health of their islet cell populations.
This study is not the first to utilize encapsulation with alginate; Barnett and his team previously paired alginate encapsulation of islet cells with magnetic resonance to create “magnetocapsules” that can be tracked during and after transplantation.
However, Shen and her team demonstrated a new practical implication of islet cell encapsulation by the seaweed-derived hydrogel. Their encapsulation process not only protects the precious islet cells from ice damage, but may also reduce transplant rejection and use of immunosuppressant drugs.
Additional Source:
OIST Press Release