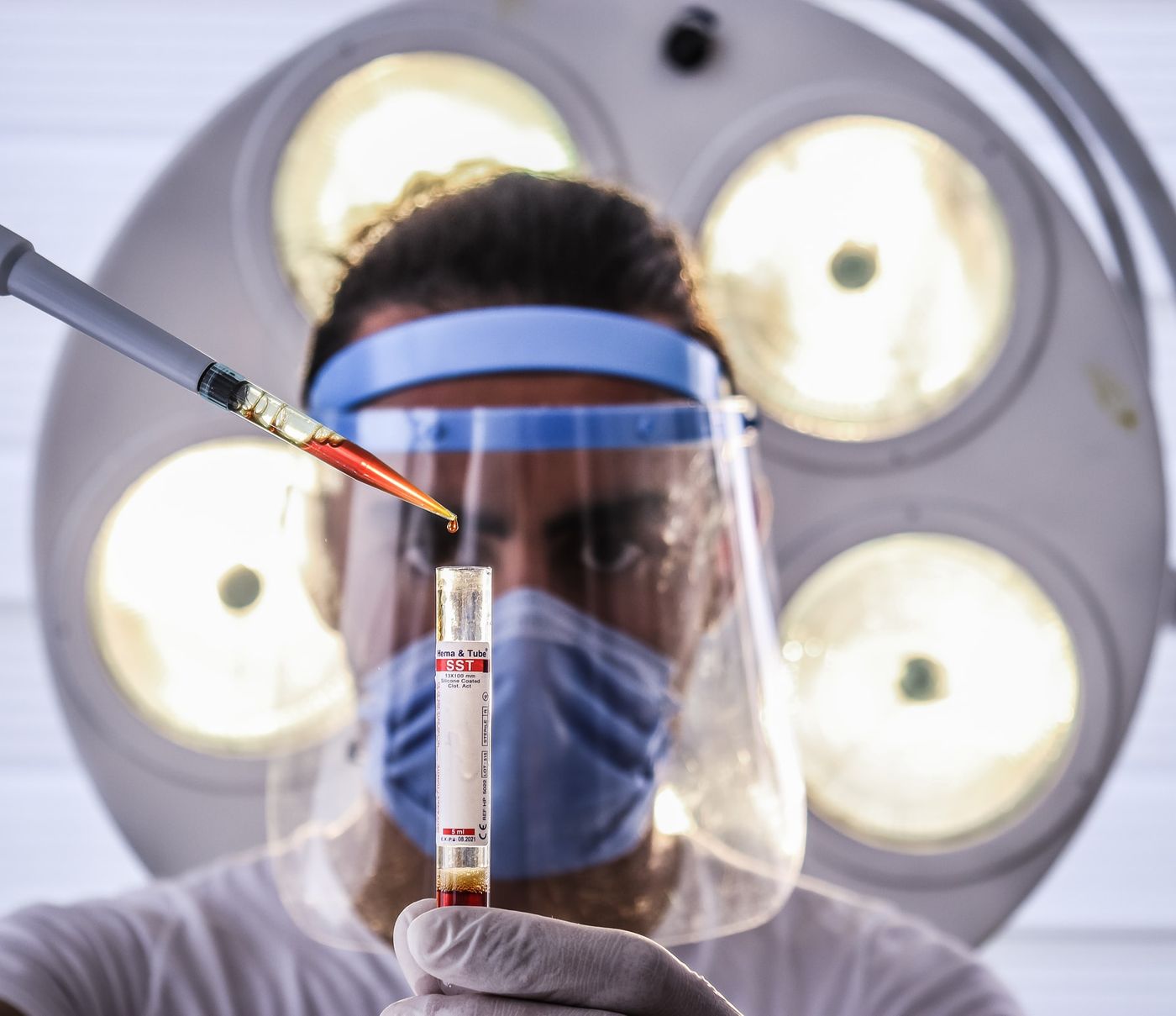
Stopping COVID False-Positives From Slipping Through the Cracks
False-positive COVID tests results—where the patient isn’t infected but receives a positive result—trigger a cascade of unnecessary patient management activities.
“False positives may lead to inappropriate quarantine, delay of other necessary medical treatment, or transfer to a COVID-19 ward,” said the University of Missouri’s Lester Layfield.
Though relatively rare, improving the accuracy of the most widely used COVID testing platform, the reverse transcriptase-polymerase chain reaction (RT-PCR), would benefit patients, healthcare systems, and public health initiatives during the pandemic.
Layfield and colleagues embarked on a mission to curtail the number of RT-PCR false positives, reporting their results in the Journal Pathology-Research and Practice.
First, the researchers developed a new protocol that acts as a safety guard for patients with no known exposure to a COVID-positive individual and no signs of infection symptoms test positive. They also deployed the quality control measure when a positive hit occurred in a well adjacent to a specimen with very high virus loads.
In their study, the team implemented the new protocol over the course of two months, where they performed over 24,700 RT-PCR COVID tests.
About a quarter of these tests came from patients who were not exhibiting any COVID symptoms. Within this group of asymptomatic patients, 288 came up as positive, but with their quality control protocol in place, repeat testing found that 20 of those were actually false positives.
According to Layfield, several factors could contribute to false positives, from sample contamination to human error. This study supports the use of additional quality control measures that diagnostic facilities should take to minimize the risk of false positives.