Science Transforms Skin Cells into Insulin-Producing Beta Cells
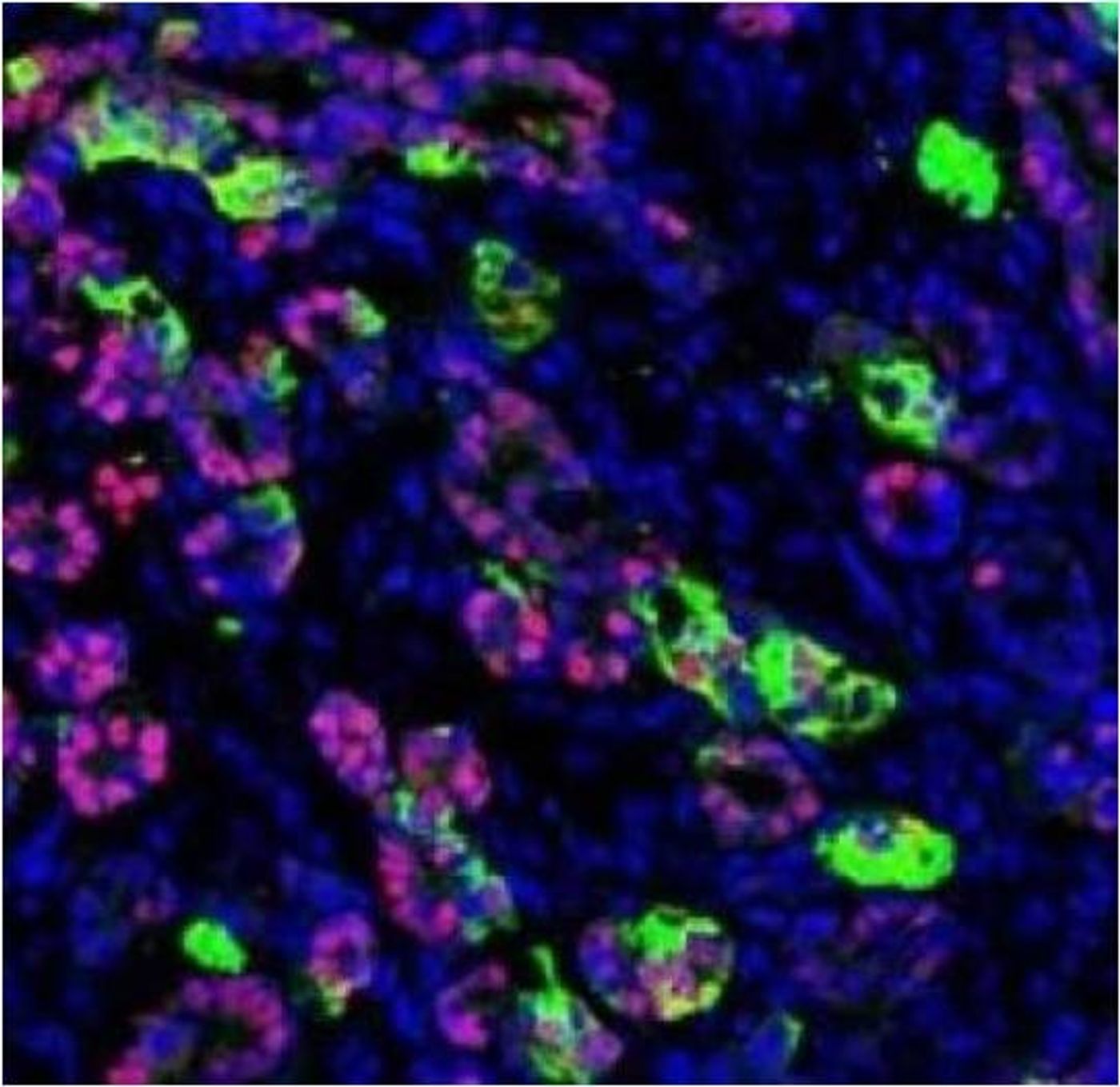
To get human skin cells to become pancreatic beta-like cells, the researchers used a cell lineage conversion method called Cell-Activation and Signaling-Directed (CASD) strategy. Effectively, they treated the skin cells with a combination of genetic and pharmaceutical agents to transform the cells into early developmental cells called endoderm progenitor cells. These cells have the potential to mature into a range of cells that make up different types of organs, including the pancreas.Our results demonstrate for the first time that human adult skin cells can be used to efficiently and rapidly generate functional pancreatic cells that behave similar to human beta cells. This finding opens up the opportunity for the analysis of patient-specific pancreatic beta cell properties and the optimization of cell therapy approaches. – Matthias Hebrok, PhD, director of the Diabetes Center at UCSF and a co-senior author on the study.
In the next steps, the researchers coaxed the early progenitor cells into pancreatic precursor cells, and then specifically into pancreatic beta-like cells. When these beta cells were transplanted into mouse models, they secreted insulin in response to glucose stimulation and effectively protected the mice from developing diabetes.
The results of this study made a great splash in diabetes research, where previous attempts at reprogramming other human embryonic stem cells into pancreatic cells proved to be too challenging. In addition to being more simple and robust, the current CASD method is faster at producing pancreatic beta cells because the reprogrammed cells don’t have to be taken all the way back to a pluripotent stem cell state. They also have greater expansion potential without compromising the new differentiated identities, a characteristic not achieved with other methods.This study represents the first successful creation of human insulin-producing pancreatic beta cells using a direct cellular reprogramming method. The final step was the most unique--and the most difficult--as molecules had not previously been identified that could take reprogrammed cells the final step to functional pancreatic cells in a dish. – Saiyong Zhu, PhD, first author and postdoctoral researcher at the Gladstone Institute of Cardiovascular Disease.
Diabetes affects nearly over 29 million Americans, and is the 7th leading cause of death in the United States (2010 data). This breakthrough research offers fresh insight into the basic understanding of pancreatic cell biology, and potentially a new way of bringing personalized cell therapy to those affected with this chronic condition.
Here's an animation of how cellular reprogramming works:
Additional source: Gladstone Institute press release








