Health officials have long suspected a correlation between the Zika virus and microcephaly, but they didn’t know this could occur. Working swiftly to address this urgent public health concern, researchers have
discovered a mechanism behind which brain cells are susceptible to Zika, and how infection alters brain cell growth.
This is so far the first evidence that biologically supports Zika’s link to microcephaly. Moreover, the study offers a platform to screen for drugs that could protect brain cells from Zika infections.
The Zika virus was first discovered in Africa in the 1940s, but it recently became headline news as South America reported one of the largest outbreaks to date. In particular, Brazil reported over 4,000 cases of Zika-linked microcephalic births in 2015 alone. This statistic represented a staggering 20-fold increase in the incidence of microcephaly in the nation. Microcephaly is marked by abnormally small heads and brains, leading to neurological and developmental deficits.
In exploring the link, researchers reported finding Zika in the amniotic fluids of women whose fetuses were diagnosed with microcephaly. Zika was also detected in the microcephalic fetal brain tissues. These evidence suggested the virus could indeed cross the placental barrier and the blood brain barrier.
To understand Zika’s actions in the brain, researchers from three universities asked and answered some basic questions: What kinds of cells in the brain are susceptible to Zika virus? And if infected, how are the functions of these cells altered?
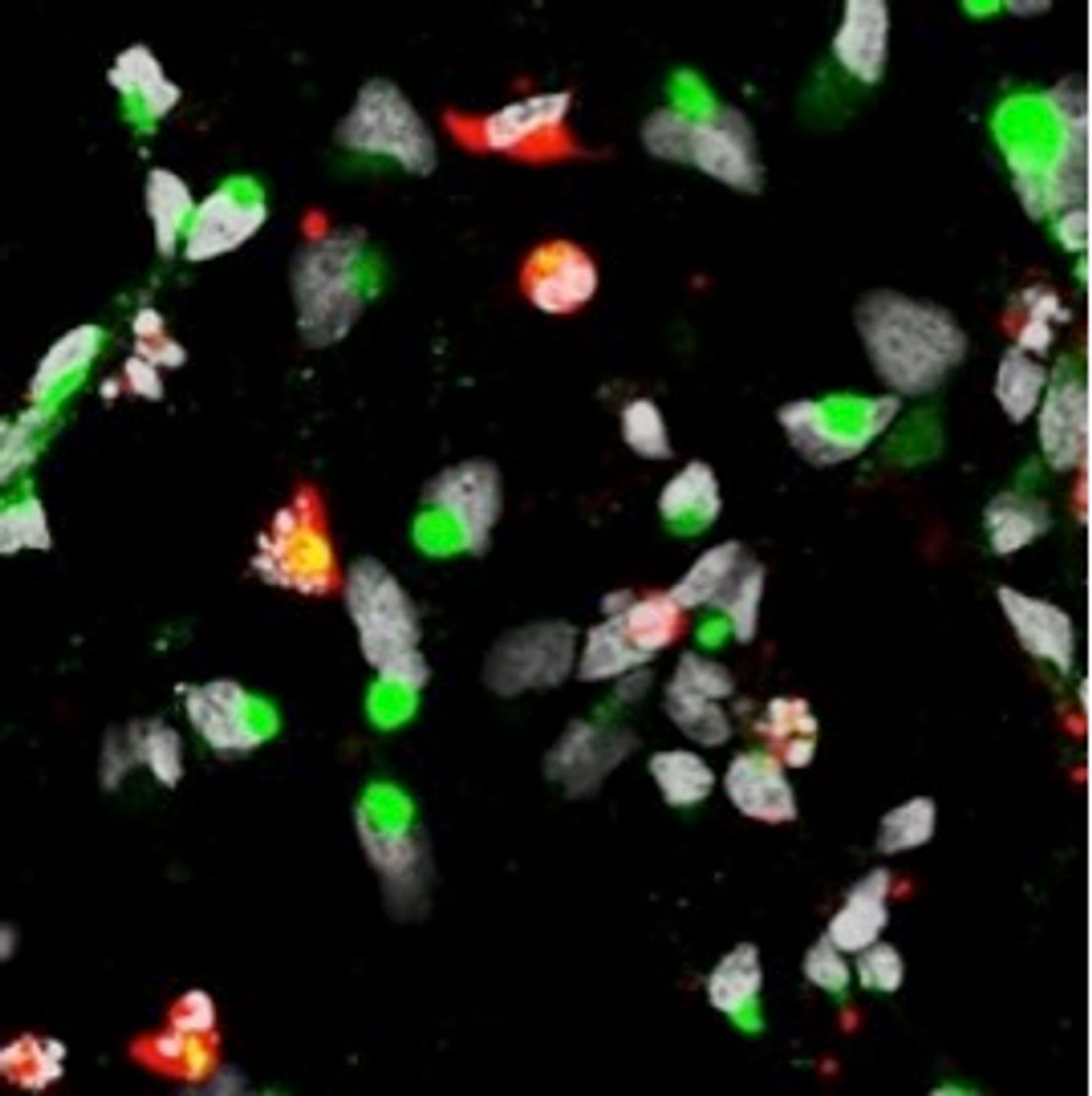
The researchers used lab-grown stem cells to model human neural cells. Specifically, they studied induced pluripotent stem cells (iPSCs), which are reprogrammed cells that can give rise to any cell in the body, including cortical neural progenitor cells. These, in turn, give rise to immature neurons in the brain. Because Zika-linked abnormalities are found in the cortex of the brain, the researchers compared Zika's effect on cortical neural progenitor cells to induced pluripotent stem cells (iPSCs) and immature neurons.
They found that the cortical neural progenitor cells were most susceptible to Zika infection. Once infected, these cells produced more of the Zika virus. This led to dysregulated cell cycle and transcription patterns that eventually caused the cells to die faster.
"While this study doesn't definitely prove that Zika virus causes microcephaly, it's very telling that the cells that form the cortex are potentially susceptible to the virus, and their growth could be disrupted by the virus," said Guo-li Ming, co-senior study author and collaborator from Johns Hopkins University.
Gene expression studies confirmed this dysregulation, as infected cells showed altered patterns of expression in genes that control cell division. In addition, genes necessary for cells to fight the infection were not turned on, which likely contributed to the cells dying so quickly.
"Now that we know cortical neural progenitor cells are the vulnerable cells, they can likely also be used to quickly screen potential new therapies for effectiveness," said Hongjun Song, one of the collaborators of the study from Johns Hopkins University.
Definitive evidence of Zika’s effect in microcephaly has to come from animal studies and clinical trials. But this research has provided a model to study how Zika mechanistically affects the brain, as well as a platform to screen potential therapeutic drugs.
Additional sources:
Johns Hopkins press release