A recent study found that treating osteoporosis brought on by hyperparathyroidism with conventional drugs could actually do more harm than help. Instead of taking medicines that seemingly strengthen bones but that are linked to more fractures, the researchers say surgery to remove the overactive parathyroid gland is a more effective alternative.
Osteoporosis refers to the loss of calcium from bones, leading to thin and brittle bones that are prone to fracture. The condition is commonly known occur as the body ages normally, but it also occurs as a result of hyperparathyroidism – that is, overactive parathyroid glands. Nearly 400,000 Americans suffer from osteoporosis brought on by their hyperparathyroidism. "Hip fractures, in particular, are associated with significant rates of mortality, disability and loss of independence," said Michael Yeh, an associate professor of surgery and medicine, and first study author.
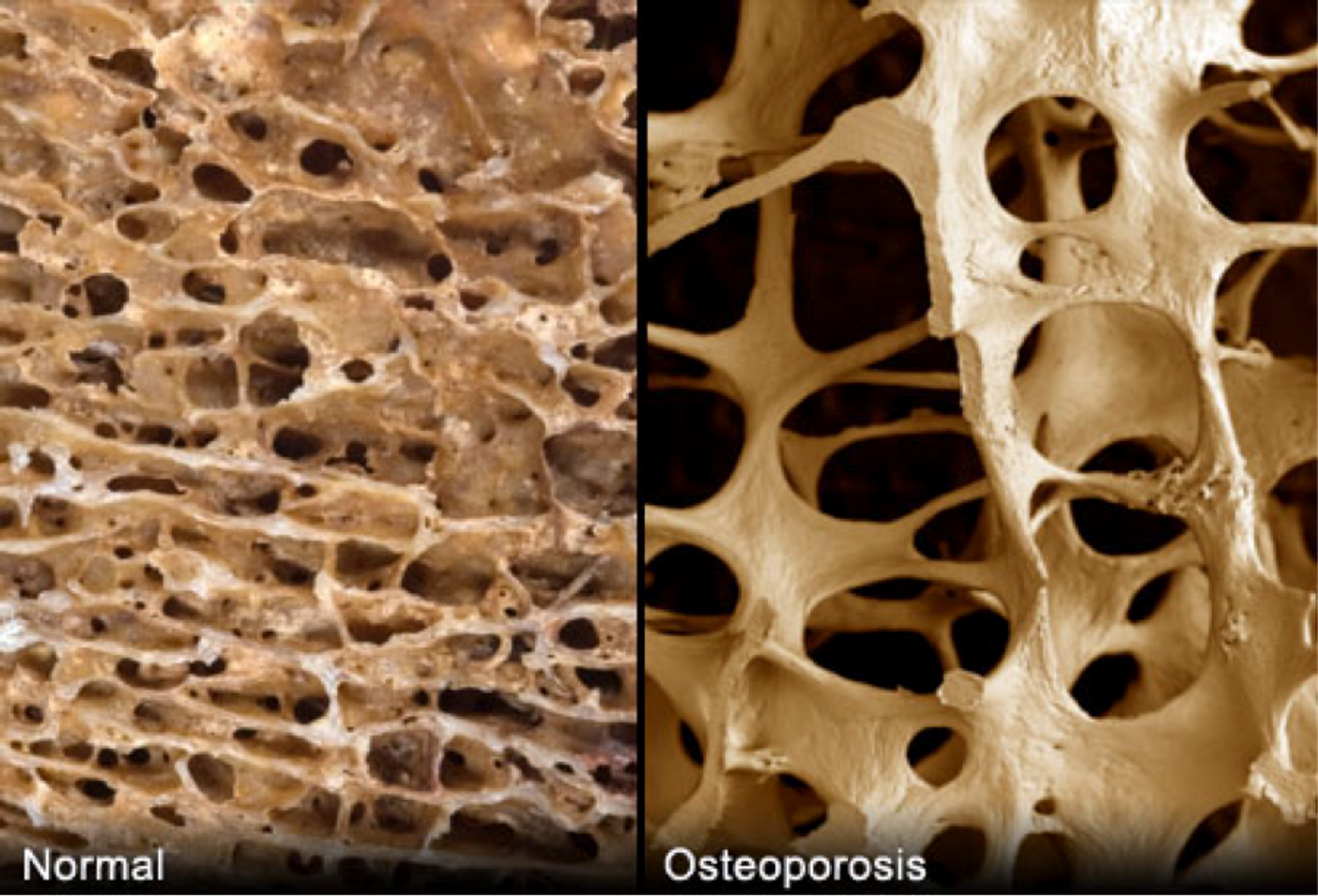
Calcium, the main component that give bones its strength and toughness, is regulated by the parathyroid hormone (PTH), which are released from the parathyroid glands, located in the neck. Normal functioning parathyroids produce PTH when the body is low on calcium, and stops PTH production when calcium levels are sufficient. In hyperparathyroidism, too much hormones over-stimulate the release of calcium from bones into the bloodstream and the subsequent reabsorption by the kidney and intestines. As a result, kidney stones accumulate more in patients with hyperparathyroidism. Moreover, bones quickly lose their calcium reserve and become thin and brittle, prone to fracture.
To combat bone loss in hyperparathyroidism, doctors routinely prescribe bisphosphonates, medicines that reduce calcium loss and strengthen bones. These include alendronate (trade name Fosamax) and ibandronate (trade name Boniva). Strangely, though X-rays show increased bone densities from these drugs, doctors didn’t see a corresponding reduction in bone fractures.
"Before this study, there was no data that compared parathyroid surgery with prescribing medication on the risk for fractures in people with hyperparathyroidism,” said Yeh. So he and his team set to describe such comparison, using data from over 6,000 people diagnosed with hyperthyroidism over a 10-year span.
They found that patients who had surgery to remove the affected parathyroid glands showed the least amount of hip fractures (20 per 1,000 people). People who received no treatment at all for their hyperparathyroidism had the next highest amount of fractures (56 per 1,000 people). The “startling” finding was in the next group: those who were treated bisphosphonates had the highest amount of hip fractures (86 per 1,000 people), which suggests taking the medicine has worse outcomes than if nothing was done at all! The team found the trend persisted when they tallied up all bone fractures of all types.
Why would medications that seemingly strengthen bones, as observed in X-rays, show higher incidences of bone fractures? The researchers were also surprised at this finding and can only speculate to the answer. "The drugs make the bones look dense on scans, but that is deceptive," Yeh said. "We must presume there is a defect in the quality of the bone. But we don't know why."
"Regardless, we were unable to demonstrate any benefit associated with this class of drugs, which have been around and routinely prescribed for more than 20 years," Yeh concluded. "These findings should make bisphosphonates less attractive as an alternative to parathyroid surgery in patients with primary hyperparathyroidism."
Additional source:
UCLA press release