A new study report found that at least 2,234 people contracted the human immunodeficiency virus (HIV) from blood transfusions administered in India in the past 17 months. The alarming figure renews the gap in India’s blood screening practices and highlights financial deficits that may have led to this contamination.
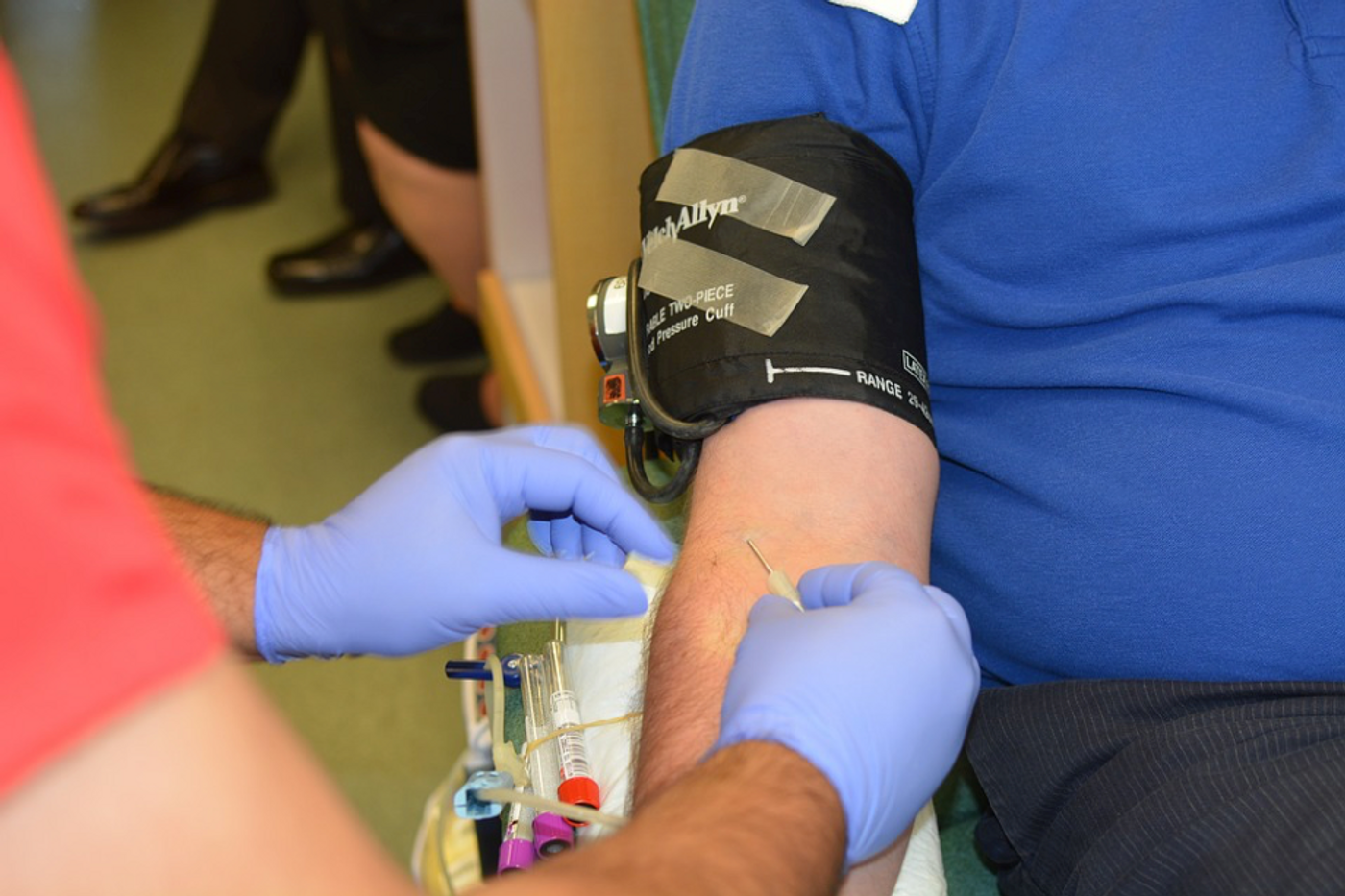
In India, about 84 percent of blood used for blood transfusions come from voluntary donations. Legally, all hospitals are supposed to have screened donated blood for contamination of HIV, hepatitis B, hepatitis C, syphilis, and malaria. But, as the figures suggest, some hospitals and clinics are non-compliant with the mandated screening practices.
According to the activist Chetan Kothari who requested the said data from the National AIDS Control Organization (NACO), which is part of the Indian Department of Health and Family Welfare, the inadequacy in screening is partly due to the lack of funding for such measures.
"Each such test costs 1,200 rupees (US$18) and most hospitals in India do not have the testing facilities," said Kothari to the BBC. "Even in a big city like Mumbai, only three private hospitals have HIV testing facilities. Even the largest government hospitals do not have the technology to screen blood for HIV. This is a very serious matter and must be addressed urgently."
There are more than 2.1 million people in India who are currently living with HIV or AIDS. Though this figure represents a slow decline in the HIV infection rates in the country – 2007 saw more than 2.2 million people infected – it nevertheless underscores why screening is so crucial in India.
While even one HIV contamination from a blood transfusion is one too many, the deputy director of NACO, Naresh Goyal, was quick to point out that India has seen a dramatic improvement in the past two decades. Compared to the 8 to 10 percent of transfusion-related HIV infections 20 years ago, the current number of infection is below 1 percent.
"These are unfortunate cases and we are working towards the goal of zero transmission. Having said that, these numbers must be looked in the context of the scale of our HIV program," said Goyal. "It is now legally mandatory for every blood bank to screening the units before giving it to a patient."
He also pointed that the latency of the virus may also contribute to the imperfect screening measures. "In some cases, the donor may be in a window period - before his HIV viral load can be detected - when he donates the blood," said Goyal. "In such cases, when screened, the blood sample shows a false negative.
India has also implemented a country-wide ban on paying donors for blood. This practice discouraged donations from people with high risk of HIV infection.
But the status of HIV infection from blood transfusion in India is still quite far from acceptable. And by calling the public’s attention to this inadequacy, activists like Kothari hope changes will happen to make receiving blood transfusions in India much less risky in the future.
Additional source:
BBC,
US News
 In India, about 84 percent of blood used for blood transfusions come from voluntary donations. Legally, all hospitals are supposed to have screened donated blood for contamination of HIV, hepatitis B, hepatitis C, syphilis, and malaria. But, as the figures suggest, some hospitals and clinics are non-compliant with the mandated screening practices.
In India, about 84 percent of blood used for blood transfusions come from voluntary donations. Legally, all hospitals are supposed to have screened donated blood for contamination of HIV, hepatitis B, hepatitis C, syphilis, and malaria. But, as the figures suggest, some hospitals and clinics are non-compliant with the mandated screening practices.