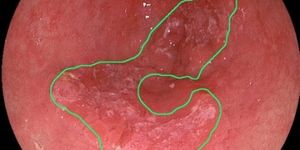
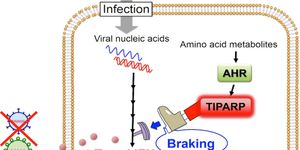
Is your sore throat caused by the
Streptococcus bacteria, or a common cold virus? It can be difficult to tell, even for trained physicians. And because of this, doctors often prescribe antibiotics when it may not be necessary or effective for the patients. Now researchers say a new blood test may discriminate infections caused by viruses versus those caused by bacteria, saving patients the need from taking antibiotics if they don’t have a bacterial infection.
According to the American College of Physicians and the Centers for Disease Control and Prevention (CDC), about 50 percent of antibiotics prescribed for respiratory infections may be unnecessary. And more is not better when it comes to undue antibiotic exposure. This can have immense negative consequences, including the risk for antibiotic resistance for the patient, and the creation of antibiotic-resistant bacterial pathogens (a.k.a. superbugs).
"If someone comes into the clinic, a bacterial or a viral infection often look exactly the same," said Timothy Sweeney, a physician and an engineering research associate at the Stanford University, and first author of the study, published in
Science Translational Medicine.
To reduce the chances of a wrong diagnosis and undue antibiotic exposure, Sweeney and his team turned to the immune response system. In particular, they focused on how the body’s immune system reacts to bacteria versus viruses. They found seven particular genes that are responsible for the body’s reaction to an infection. And the levels of these genes vary between a bacterial infection and a viral infection. This difference can be measured in a simple blood test, letting doctors know whether or not to prescribe antibiotics.
The team tested their concept in 96 children who were diagnosed with sepsis, a system-wide infection of the blood that can be lethal. Sweeney’s test correctly identified 90 percent of cases where the sepsis was caused by bacterial infection, and 55 percent of cases caused by viral infection.
While it’s a great step forward in reducing unnecessary use of antibiotics, the team admits there’s plenty more to be done before the blood test is ready for the clinic. For example, one of the next big focuses of the research is to reduce the test’s diagnostic time. Right now, it takes 4 to 6 hours to get an answer from the blood test, and that is "likely too slow for clinical application," the authors wrote. In an emergency setting where sepsis and other critical infections are concerned, the mortality rate increases dramatically for every hour antibiotics are delayed. Thus, time is crucial for such a test to be effective.
But the team is also quick to point out that the test, if successfully applied in the clinics, could save billions of dollars in the long run. This takes into account the cost of treating antibiotic-resistant infections, which is estimated to run about $100 trillion in health care costs by 2050.
Additional source:
Stanford press release