It may not look like much – a silicone device no bigger than a USB flash drive. But researchers say this device is the first system to model one of the most mysterious organs in humans: the placenta. Dubbed the “
placenta-on-a-chip,” this system uses actual living cells that mimic the barrier that separates mom’s circulation system from that of the baby. This device will provide insight into how nutrients move across the placenta, which could then broaden potential causes and treatment for preterm births.
Even in the current wave of 20
th century medicine, the placenta remains the “least understood organ in the human body," said Dan Huh, first author of the study. This organ only develops in the uterus during pregnancy, acting to support the health and growth of the fetus. Among its many roles, the placenta allows oxygen and nutrients to get to the baby while removing waste products away from the baby’s system. Soon after giving birth to the baby, the placenta is also removed from the woman’s body.
"Beyond the scarcity of samples," said Cassidy Blundell, first author of the study, "there's a limited lifespan of how long the tissue remains viable, for only a few hours after delivery, and the system that is used to perfuse the tissue and perform transport studies is complex."
Thus, a chip that can model how the placenta supports a healthy pregnancy is extremely valuable.
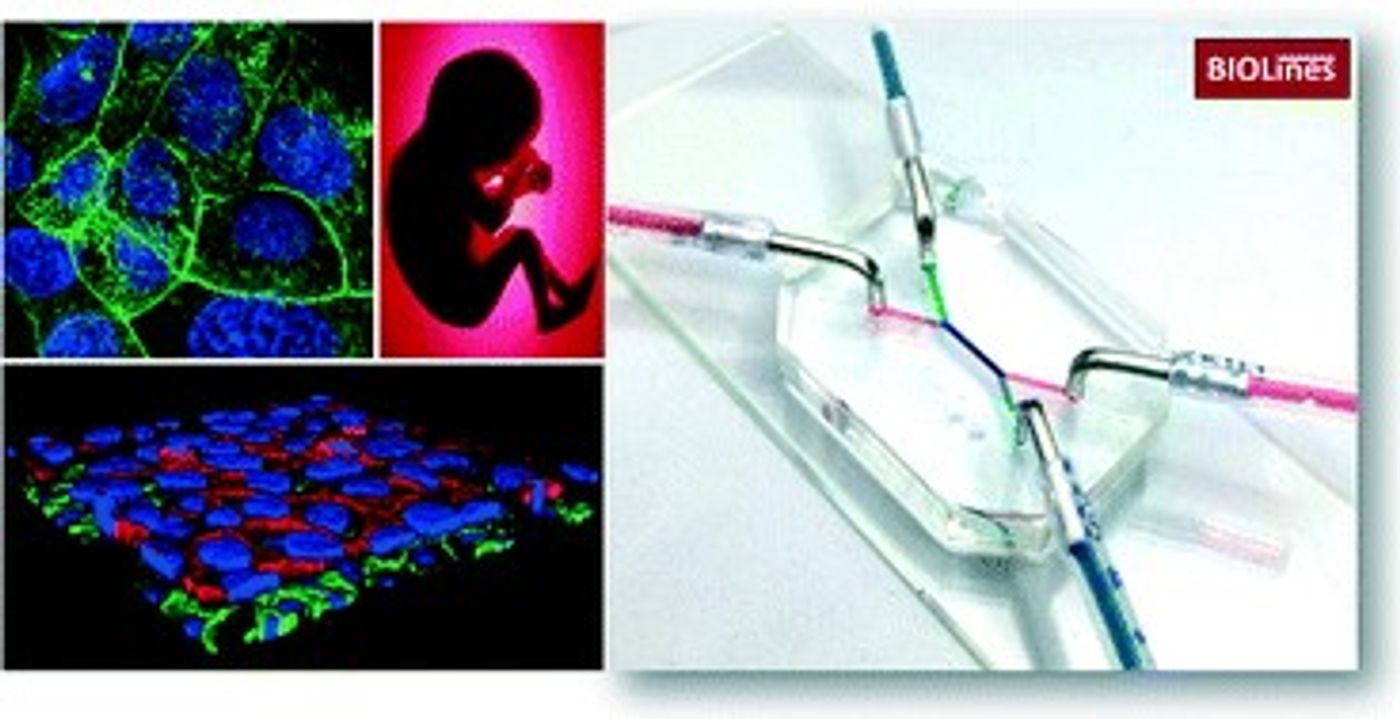
The placenta-on-a-chip consists of two microfluidic channels that are separated by a membrane. They placed trophoblast cells on one side of the membrane; these are the cells that are on the mom’s side of the placenta. On the other side of the membrane are endothelial cells, which are found in the fetus’ blood. Together, the cells and the membrane allow scientists to model nutrient flow in both directions.
"That barrier mediates all transport between mother and fetus during pregnancy. Nutrients, but also foreign agents like viruses, need to be either transported by that barrier or stopped,” said Blundell.
In addition to having the right type of cells, it was also important to mimic how the cells would change during the course of a natural pregnancy. Indeed, the team showed the cells on the chip shifted in growth.
"During pregnancy, the placental trophoblast cells actually fuse with one another to form an interesting tissue called syncytium. The barrier also becomes thinner as the pregnancy progresses, and with our new model we're able to reproduce this change,” said Dongeun Huh, the study’s senior investigator. "This process is very important because it affects placental transport and was a critical aspect not represented in our previous model."
The team hopes their model can be used to study the causes of preterm birth and possible ways this can be prevented. This is an especially important cause as preterm birth accounts for over 10 percent of all pregnancies, but we know very little about what can be done to prevent it.
Additional source:
University of Pennsylvania press release
 The placenta-on-a-chip consists of two microfluidic channels that are separated by a membrane. They placed trophoblast cells on one side of the membrane; these are the cells that are on the mom’s side of the placenta. On the other side of the membrane are endothelial cells, which are found in the fetus’ blood. Together, the cells and the membrane allow scientists to model nutrient flow in both directions.
The placenta-on-a-chip consists of two microfluidic channels that are separated by a membrane. They placed trophoblast cells on one side of the membrane; these are the cells that are on the mom’s side of the placenta. On the other side of the membrane are endothelial cells, which are found in the fetus’ blood. Together, the cells and the membrane allow scientists to model nutrient flow in both directions.