Glioblastomas are notorious for being inoperable. That’s why when scientists developed a laser method to “cook” the tumor from the inside, they thought it was game-over for the malignant cancer. However, doctors soon discovered other problems – the tumor became swollen and endangered patients in other ways. Now, a
combination technique may finally make it possible to effectively treat and remove the cancer.
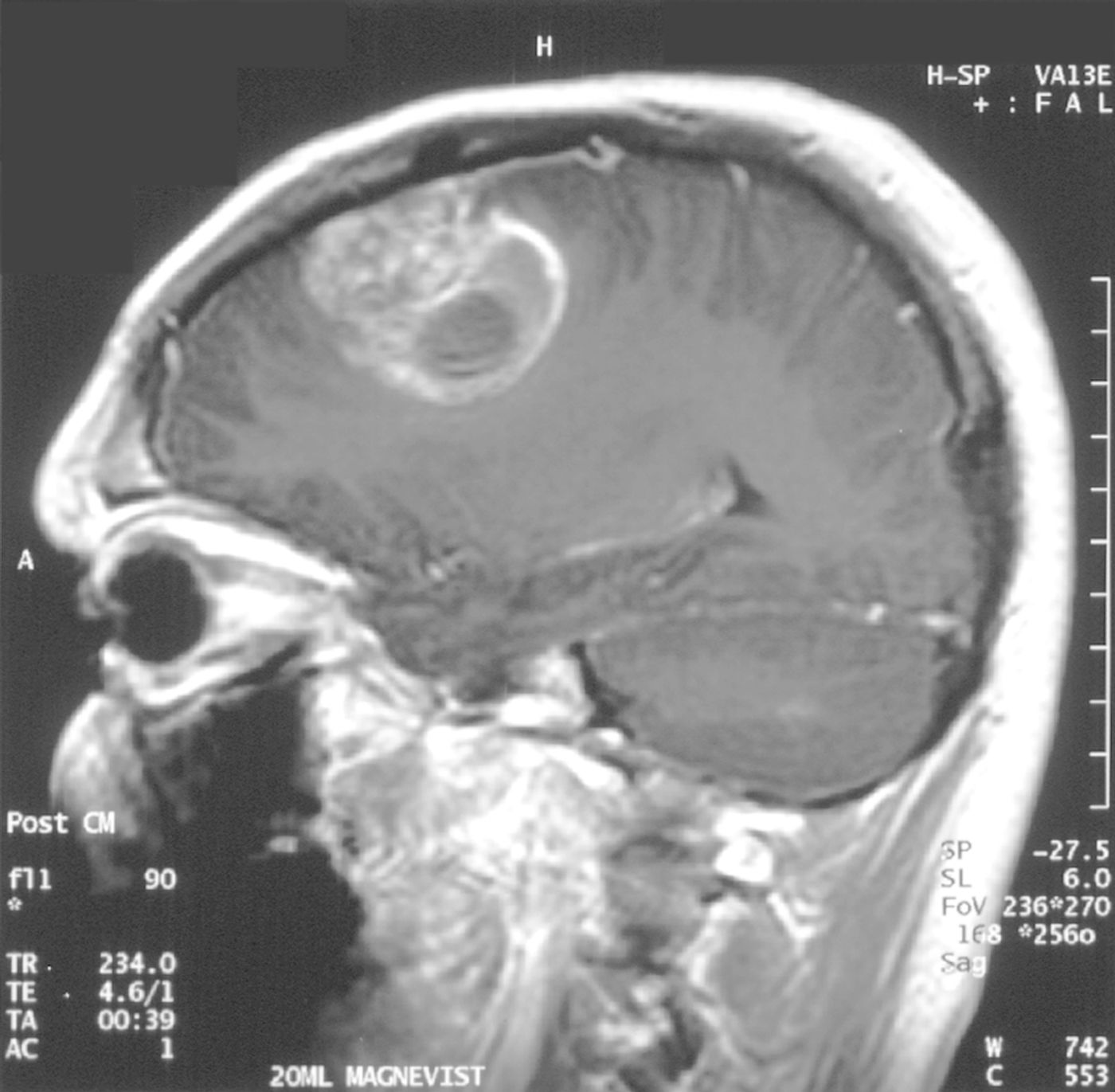
Dubbed as the “octopus tumor,” GBMs are characterized with malignant glial cells forming vast networks of tendrils throughout the brain. This makes it nearly impossible to surgically remove all the cancerous tissues. As such, this brain cancer can evade even the most aggressive surgeries, chemotherapies, and radiotherapies, leaving patients with a five-year survival rate of less than 10 percent.
In 2013, Andrew Sloan and his colleagues pioneered a technique to treat the “inoperable” tumor. Since it would be difficult to remove it with conventional scalpels, Sloan and his team thought to kill the tumor by heating it up from the inside. They team developed a technique known as laser interstitial thermotherapy (LITT), which targets the laser to the tumor via a small hole in the scalp.
While LITT was successful at attacking the tumor, doctors soon found that the treatment led to swelling. This was especially dangerous for large tumors, where the deep swelling could seriously jeopardize a patient’s health.
So the surgeons had no choice but to operate on the inoperable. But in the course of this procedure, Dr. Sloan made a starling realization: the swollen, cooked tumor was mushy instead dense, and clean instead of bloody – the heat had apparently cauterized the tumor’s blood supply. This state of the tumor was amenable to being “sucked out” through a small hole in the skull, a craniotomy.
"I am very excited by the results of this study. This procedure is a new option for patients with these large malignant tumors," said Andrew Sloan, surgeon at the University Hospitals Case Medical Center, and lead author of the new study. "We have seen similar results and overall survival compared to LITT procedures performed in patients with smaller lesions and with lower risk."
The team has since performed this combination technique on 10 patients with extremely aggressive and intractable brain tumors, with promising results. Of the 10 patients, 6 remain alive with a median progression-free survival of 280 days, and a median overall survival of 482 days.
"We feel with further studies, LITT will continue to develop into a safer, more user-friendly technique that may help remove more of these deadly tumors than surgery alone can accomplish," said Sloan.
Additional sources:
MNT
 Dubbed as the “octopus tumor,” GBMs are characterized with malignant glial cells forming vast networks of tendrils throughout the brain. This makes it nearly impossible to surgically remove all the cancerous tissues. As such, this brain cancer can evade even the most aggressive surgeries, chemotherapies, and radiotherapies, leaving patients with a five-year survival rate of less than 10 percent.
Dubbed as the “octopus tumor,” GBMs are characterized with malignant glial cells forming vast networks of tendrils throughout the brain. This makes it nearly impossible to surgically remove all the cancerous tissues. As such, this brain cancer can evade even the most aggressive surgeries, chemotherapies, and radiotherapies, leaving patients with a five-year survival rate of less than 10 percent.