Colon Cancer Screening Via Gut Bacteria?
The gut microbiome is increasingly recognized as a vital player in the development of colon cancer. And now, this microbial knowledge could be translated into a non-invasive diagnostic test that will predict the risk of colorectal cancer.
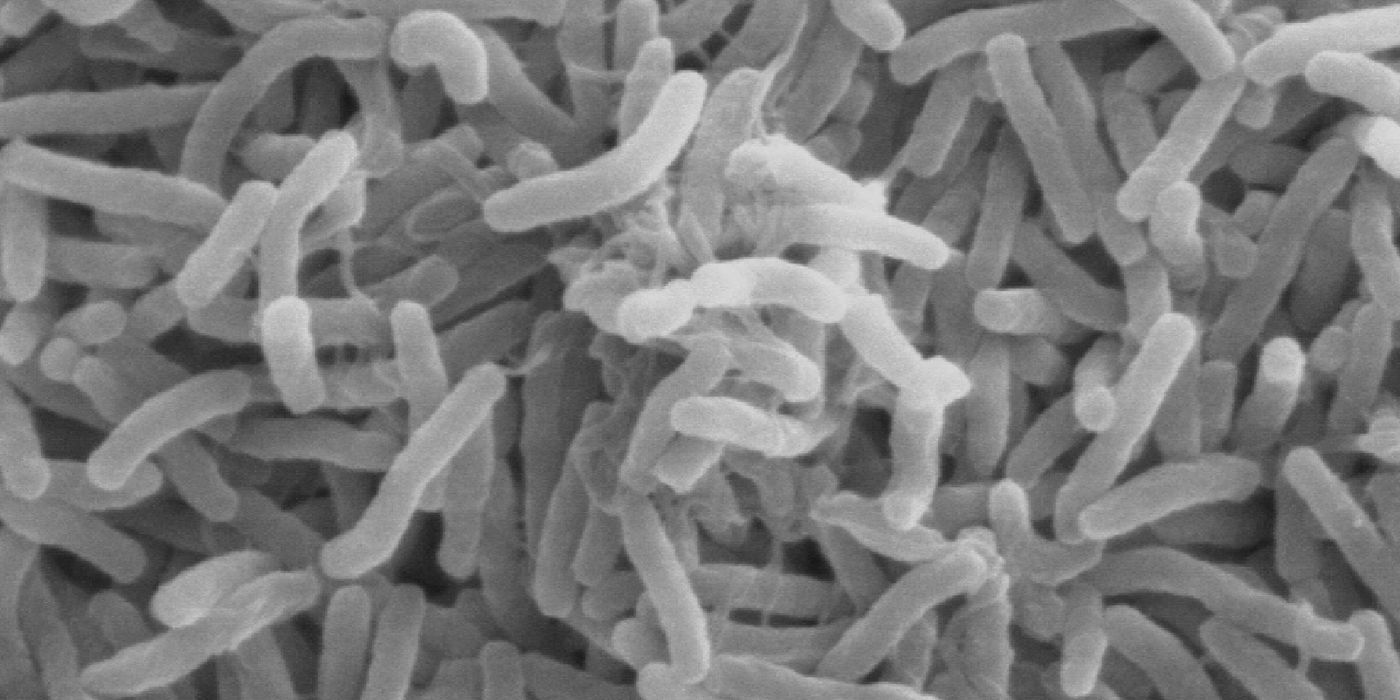
The importance of the microbiome has only being fully realized and appreciated in the recent years. The microbiome is a specialized collection of bacteria residing in specialized niches of the body. Mostly famous for their existence in the human gut, these communities of microorganisms have been known to influence processes like digestion and immune responses.
The gut microbiota, in particular, has been linked to inflammatory bowel diseases such as Crohn’s disease and ulcerative colitis. In turn, these diseases increase the risk for colon cancer. Scientists have observed a marked increase in the incidence of colon cancer since the mid-20th century, which they correlate with a shift in the intestinal microbiota.
Currently, approximately over 1 million Americans are diagnosed with colorectal cancer, which is the second leading cause of cancer-related death in the US. Despite this alarming statistics, about a third of people at high risk for the disease have never been screened. It probably doesn’t help that the most common method of screening involves a painful and highly invasive colonoscopy exam.
But researchers at the Baylor College of Medicine asked whether a diagnostic test can be created based on the gut microbiome profile of a patient. That is, can they pinpoint bacterial biomarkers that could predict the risks of colon cancer development?
To find the colon cancer microbial biomarkers, Dr. Manasi Shah opted to “leverage existing raw data across multiple cohorts and come up with a generalizable marker for the disease." She collaborated with Dr. Emily Hollister, assistant professor of pathology at Baylor and Texas Children's Hospital and director of microbial ecology for the Texas Children's Microbiome Center, to sift through large microbiome data from several studies. They were looking for bacteria that were associated with colon cancer and the DNA sequences of these bacteria.
After intensely digging and comparing the DNA sequences of many strains of bacteria, they identified some strains that were previously associated with colon cancer, as well as some new strains that had yet to be implicated.
"The fact that even when we combined several different studies we could correctly classify a sample as a colorectal cancer case or control with 80 percent accuracy solely based on microbial abundances was very encouraging," Shah said. Further validation and optimization for the diagnostic test is ongoing.
"This is a promising first step to develop a noninvasive test that might be used in the detection of colorectal cancer, supplementing colonoscopy or fecal occult blood tests," Hollister said.
Additional source: Baylor College of Medicinehttps://www.bcm.edu/news/cancer/non-invasive-colorectal-cancer-test