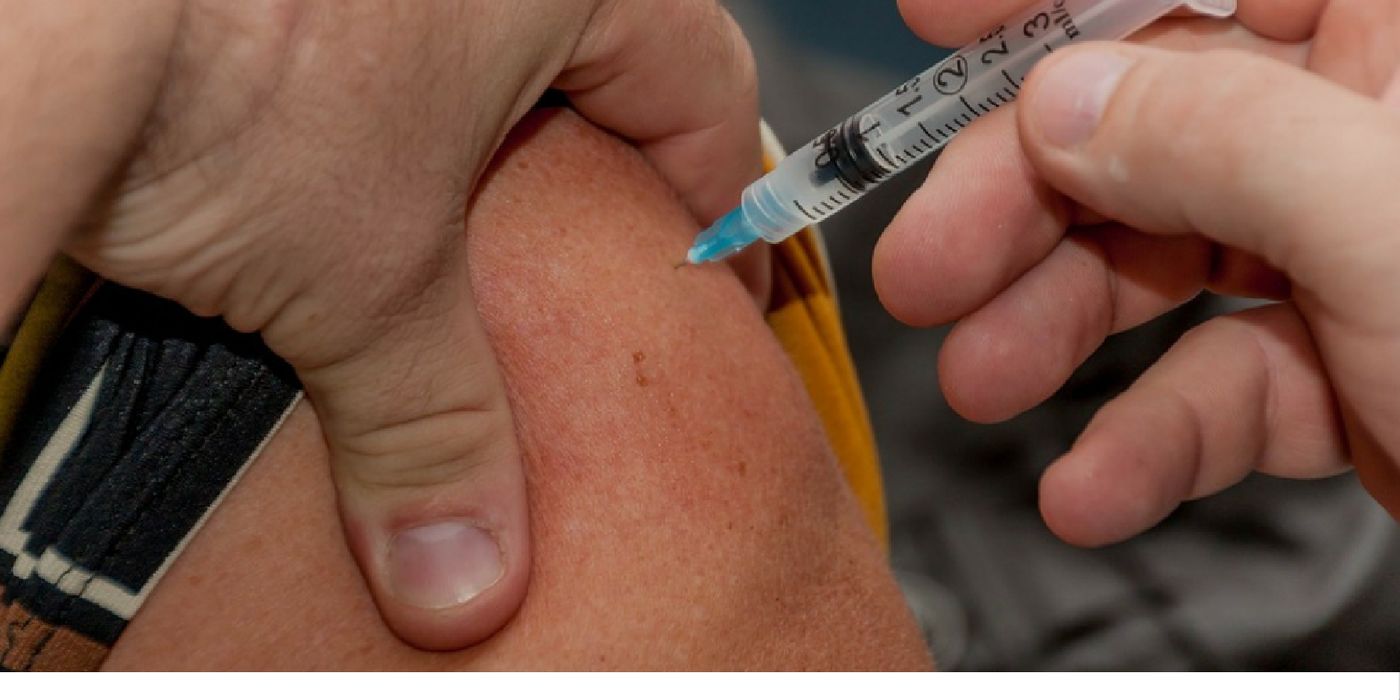
Personalized Cancer Vaccines Edge Out Melanoma Tumors
In a rare scientific double-whammy, two groups of scientists independently found that targeted, personalized vaccines stopped the growth of dangerous melanoma cancers. The groups used two different methods to arrive at a similar conclusion: cancer vaccines can be reality sooner than we think.
In the first study, Catherine Wu, associate professor at the Dana-Farber Cancer Institute in Boston, vaccinated six patients who had recently had tumor-removal surgery. The vaccine Wu’s team used contained up to 20 neoantigens - small proteins specifically found on the outside of cancer cells - all specifically picked for each patient based on their cancer profile. The dose of neoantigens works to trigger the immune system to recognize and attack the cancer cells.
Similarly, the parallel study, led by Ugur Sahin from Germany, also targeted melanoma cancer cells with neoantigens. However, the vaccines that Sahin’s group designed were made with RNA molecules, which provide the patient’s cells instructions to make their own neoantigens. But like Wu, the RNA vaccines also had to be designed specific to each patient’s mutation profile.
In both studies, patients treated with the vaccine showed cancer suppression. "We were delighted to see a strong and consistent response among the six patients we treated," said Catherine Wu, the senior author of the trial conducted in Boston. "Vaccines can focus and mobilize the body's standing army of T cells."
Of the six patients in Wu’s trial, four had stage III cancer but showed no sign of tumor after 25 months of vaccination. Of the 13 patients in Sahin’s trial, eight were completely tumor-free by 23 months. Furthermore, both studies found that using the vaccine in combination with another treatment, called checkpoint therapy, improved the patients’ responses. Patients in both trial that had relapsed showed improvement with this combination therapy.
“We can safely and feasibly create a vaccine that is personalized to an individual’s tumor,” said Wu. “It’s not one-size-fits-all—rather, it’s tailored to the genetic composition of the patient’s tumor.” Indeed, the success of these vaccines seemed to hinge on predicting the best set of neoantigens for the patient’s immune system. This crucial step personalizes the treatment for the patient, but could make it difficult to scale up for mass vaccine production.
Nevertheless, the two studies demonstrate the vast potential of cancer vaccines. “Using very different delivery systems, we arrived at very similar conclusions,” said Wu. “It gives more robust grounds for proceeding into future directions.” Researchers are looking to explore vaccines for other cancers, such as glioblastoma and ovarian cancer.
Additional sources: Live Science, Popular Science